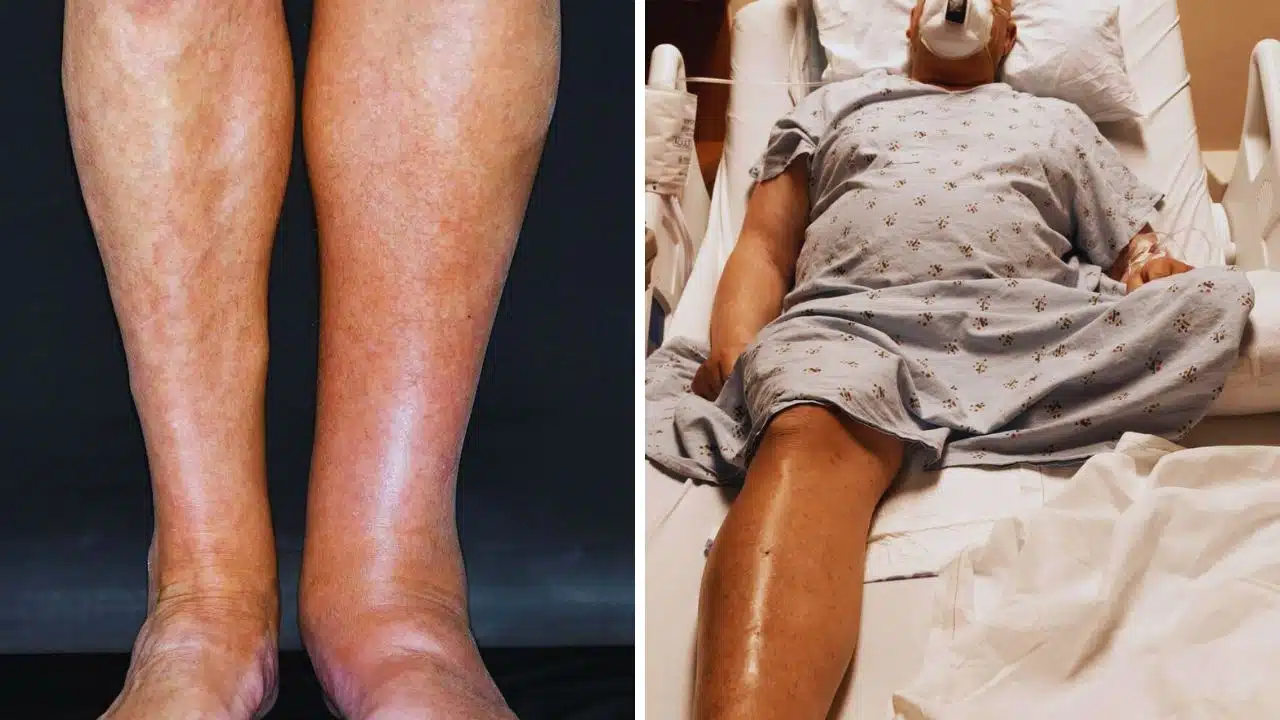
Deep vein thrombosis (DVT) poses a significant health risk, particularly when blood clots form in the legs. This condition can lead to severe complications such as pulmonary embolism, where a clot travels to the lungs, potentially causing life-threatening consequences.
Prompt medical intervention is crucial to manage DVT effectively and prevent complications. Treatment typically involves anticoagulant medications to prevent clot enlargement and recurrence. In some cases, clot-dissolving drugs or placement of filters to trap clots may be necessary.
This article explores comprehensive approaches to treating DVT, including supportive therapies and lifestyle adjustments aimed at minimizing long-term complications like post-thrombotic syndrome.
Understanding these treatment options is essential for anyone at risk or diagnosed with DVT, highlighting the importance of early diagnosis and proper medical management.
Understanding Deep Vein Thrombosis (DVT)
DVT occurs when a clot forms in a deep vein, usually in the legs. This clot can break loose, travel through the bloodstream, and block the lungs’ arteries, leading to a pulmonary embolism—a life-threatening condition.
Causes and Risk Factors
Venous Stasis: Reduced blood flow due to prolonged immobility, such as during long flights or bed rest.
Endothelial Injury: Damage to the inner lining of the blood vessels, which can occur from surgery, trauma, or inflammation.
Hypercoagulability: Conditions or medications that increase blood clotting risk, such as pregnancy, hormonal therapy, or certain genetic disorders.
Symptoms
- Swelling in the affected leg, often in the calf or thigh.
- Pain or tenderness is usually described as a cramping or soreness.
- Red or discolored skin on the leg.
- Warmth over the affected area.
- Swelling or pain in one leg, without an obvious cause, should prompt immediate medical evaluation.
Medical Treatment: Anticoagulants
The cornerstone of DVT treatment is anticoagulant therapy, commonly known as blood thinners. These medications do not dissolve existing clots but prevent them from enlarging and reduce the risk of new clots. Types of anticoagulants include:
- Direct Oral Anticoagulants (DOACs): Such as Eliquis (apixaban), Pradaxa (dabigatran), Savaysa (edoxaban), and Xarelto (rivaroxaban), taken orally.
- Low Molecular Weight Heparin (LMWH): Injected under the skin, like Lovenox (enoxaparin) and Fragmin (dalteparin).
- Warfarin: A pill that requires regular blood monitoring.
The choice of anticoagulant depends on factors like bleeding risk, medical history, and patient preference.
Thrombolytics: Dissolving Blood Clots
In severe cases or when anticoagulants are ineffective or contraindicated, thrombolytic drugs can be used. These drugs, administered either through catheters directly into the clot (catheter-directed thrombolysis) or intravenously (systemic thrombolysis), dissolve clots by activating plasmin.
This enzyme breaks down fibrin strands holding clots together. Thrombolytics are reserved for high-risk situations due to their potential for significant bleeding complications.
IVC Filter: Preventing Pulmonary Embolism
For individuals unable to tolerate anticoagulants, an inferior vena cava (IVC) filter may be implanted. This device traps clots before they reach the lungs, reducing the risk of pulmonary embolism. However, IVC filters do not prevent new clots from forming and are not as effective as anticoagulation in the long term.
Management of Post-Thrombotic Syndrome
Post-thrombotic syndrome, a common complication of DVT, can lead to chronic venous insufficiency. Symptoms include leg pain, swelling, and skin changes. Preventive measures include:
- Compression Stockings: Aid in improving blood flow and reducing swelling.
- Elevating Legs: Reduces pressure and promotes circulation.
- Exercise: Helps maintain calf muscle strength and flexibility.
In severe cases, surgical interventions like stenting may be considered to improve vein function.
Prevention and Lifestyle Tips
Maintaining a healthy lifestyle can significantly reduce the risk of DVT:
- Stay Active: Regular movement, especially after surgery or during prolonged immobility, reduces clotting risk.
- Healthy Diet: A diet rich in anti-inflammatory foods, like the Mediterranean diet, can lower clotting risks.
- Avoid Risk Factors: Quit smoking, manage weight, and avoid prolonged sitting or crossing legs.
Wrap up
Prompt medical intervention is crucial in managing DVT to prevent serious complications like pulmonary embolism and post-thrombotic syndrome.
While supportive measures and lifestyle changes play a role, medical treatment with anticoagulants remains the foundation for managing and preventing blood clots in the legs.
By understanding these treatment options and preventive measures, individuals can effectively manage DVT and reduce associated risks, ensuring better long-term vascular health.
Always consult a healthcare provider for personalized advice and treatment options tailored to individual needs and medical history.
The information is taken from various journals and recent research.