Blood test results often look confusing at first glance—filled with numbers, abbreviations, and terms like complete blood count and reference range. Many people find it difficult to understand what these results actually mean for their health.
It can feel like reading a map without knowing the symbols. While doctors use lab reports to monitor health and detect issues early, interpreting them without guidance can be challenging.
Blood tests analyze key components such as red blood cells, white blood cells, and electrolytes. These help identify conditions like anemia, infections, or dehydration. Reference ranges are based on healthy populations, but they can vary by age, gender, and lab standards—so always compare with the specific ranges provided in the report.
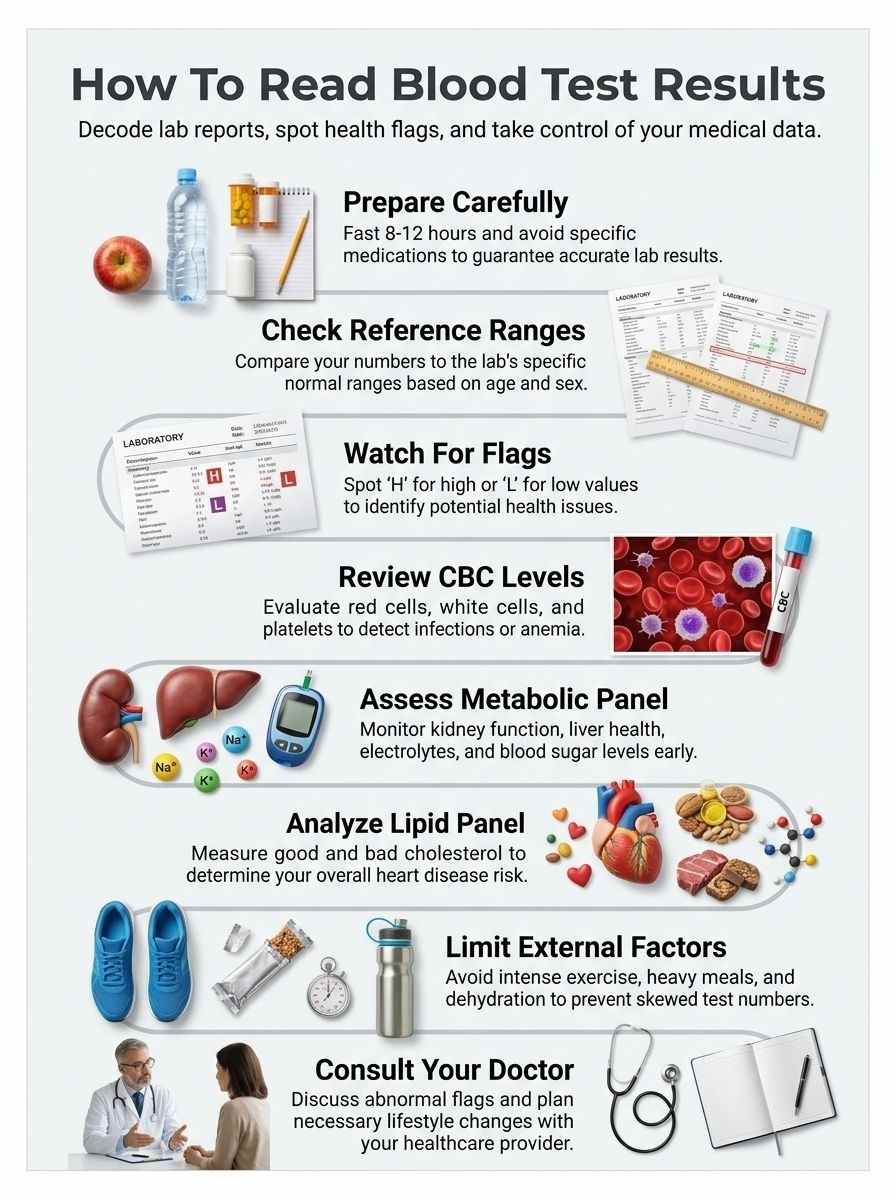
This guide to Read Blood Test Results simplifies the process step by step. Learn how to interpret common markers, understand flags like “H” (high) or “L” (low), and recognize when to consult a healthcare provider.
Clear, simple, and practical—no confusion, just answers.
What Are Blood Tests?
Blood tests, those quick draws from your vein, act like a snapshot of your health, revealing how your body fights off bugs or handles sugar levels. Doctors order them for check-ups, to spot issues like anemia or infections, so you can chat with your healthcare provider about what comes next.
Definition and purpose
Labs analyze samples like blood, urine, or other body fluids and tissues. They assess health by spotting substances and their levels. For instance, a pregnancy test spots a clear sign of a condition.
A comprehensive metabolic panel (CMP) gives broad health clues instead. Docs order these tests to peek into specific health spots or snap a complete health picture. Common ones include complete blood count (CBC), metabolic panels, and checks for hormone or vitamin levels.
Tests team up with physical exams, your health story, family health past, and imaging results for the full view. They prove key for tracking cancer treatment impacts and general wellness.
Providers request them to probe health worries, spot or nix diseases, watch conditions, and shape treatment paths. Some, like blood glucose tests or thyroid function tests, target issues such as diabetes or kidney disease.
Others, including lipid panels or cholesterol tests, flag risks for heart disease.
Laboratory tests are ordered to gain insight into specific health aspects or establish a complete health snapshot, notes the National Library of Medicine.
Common reasons for blood tests
Doctors order blood tests for many reasons. These tests help spot health issues early and keep you on track.
- Routine health screening tops the list for common reasons. You get these during check-ups to catch risks for diseases like diabetes or heart problems. General health tests can indicate risk for specific diseases and the need for further testing. Think of screening tests as your body’s early warning system, spotting issues before they grow big. Blood tests can evaluate kidney and liver function, electrolyte levels, and cholesterol, among others. For example, a basic metabolic panel checks your kidney function, calcium, and bicarbonate levels. Healthcare providers use these to guide next steps, like a colonoscopy if results hint at problems.
- Diagnosis of new symptoms prompts many blood tests. Say you feel tired all the time, your doctor might order tests to find the cause. Lab tests may be ordered for routine health screening, diagnosis of new symptoms, or ongoing monitoring of chronic conditions. A complete blood count (CBC) looks at white blood cells (WBC), red blood cells (RBC), hemoglobin (HGB), platelets (PLT), and hematocrit (HCT). This helps diagnose infections or anemia. COVID-19 tests are examples of tests indicating presence or absence of a specific germ in the sample. Your healthcare professional reviews these with you, explaining proteins, minerals, hormones, and enzymes in the mix.
- Ongoing monitoring of chronic conditions keeps blood tests in play. If you have something like high blood pressure, tests track how it’s going. Blood tests are used to monitor conditions, evaluate progression, or assess treatment efficacy. During cancer treatment, a Complete Blood Count (CBC) is the most commonly performed lab test. It checks mean corpuscular volume (MCV), erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) to see how your immune system responds. Tumor marker tests, like prostate-specific antigen for prostate cancer, help too. Kidneys, liver function tests, and lipid panel results guide adjustments in your care.
- Evaluation during treatments makes blood tests crucial. Doctors use them to see if meds work or cause side effects. At-home test kits are available for various lab tests but should not substitute for provider-ordered tests. A metabolic panel or electrolyte panel monitors levels of albumin, TP, bilirubin, GGT, and LDH. Physical activity before the test can skew results, so follow prep tips. Your health care provider accesses these via electronic health record for quick chats.
- Special checks for things like vitamin deficiencies or hormone levels round out reasons. Feeling off? Tests pinpoint lacks in vitamins or odd hormone shifts. Specialized blood tests, like those for genetic mutations, dig deeper. MedlinePlus or Cleveland Clinic resources explain these well. Mean corpuscular hemoglobin concentration (MCHC) and mean platelet volume (MPV) give clues about blood health. Talk to your healthcare provider about any flags, they make sense of it all.
Key Components of a Blood Test Report
Ever stared at that lab sheet, feeling like it’s written in code? Your blood work lists the test, like red cell count, right next to your number, and compares it to standard levels to spot if you’re off track, say with a high mark on glucose.
Test name and your result
Your blood test report lists each test name right next to your personal result. Labs show these as numbers, like in a basic metabolic panel (BMP) or complete metabolic panel, to highlight how your body functions.
These numerical values get compared to a reference range, which marks the normal zone for most people. For example, a white blood cell count might appear as 6.2, a simplified way to say 6,200 without all the zeros cluttering things up.
Units vary too, such as mcg/dL for micrograms per deciliter, micromole/L for micromoles per liter, or pg/mL for picograms per milliliter, keeping everything clear and precise.
You might spot your results through patient portals or grab printed copies at places like cancer facilities. Thanks to the CURES Act, you often see these medical tests at the same time as your doctor does.
Results fall into categories that give insights into your health, like lipid labs checking cholesterol levels. Grab a copy of your lab results, folks, and chat them over with your care team to make sense of where your numbers land in that specific normal range.
Reference range (normal range)
Reference ranges show the normal high and low values for blood tests. Labs base these on results from big groups of healthy people. Think of them like a yardstick that measures what’s typical for most folks.
These ranges differ by age and sex, for sure. Take red blood cells, or RBCs, as an example. Women often see a normal span from 4.2 to 5.4 million per microliter. Men get 4.7 to 6.1 million per microliter.
Platelets sit in a normal zone of 150,000 to 450,000 cells per microliter. White blood cells, WBCs, range from 5 to 10 times 1,000 per cubic millimeter. Hemoglobin, Hgb, hits 12 to 18 grams per deciliter.
Hematocrit, Hct, spans 37 to 52 percent.
Labs tweak these ranges based on their methods, so they vary from place to place. Stick to the specific range in your own report; that’s the smart move. Populations shift them too, like kids versus grown-ups.
You can’t compare results across different labs, no way. For spotting trends over time, use the same lab each go-round. Reports always list normal ranges for each test, adjusted by age and sex.
Platelets again clock in at 150 to 450 times 1,000 per cubic millimeter. RBCs cover 4.2 to 6.1 times 1,000,000 per cubic millimeter.
Flags for abnormal results (H for high, L for low)
Labs often mark your blood test results with flags to highlight anything unusual. They use “H” for high values that exceed the normal range, and “L” for low ones that fall below it.
Imagine it like a traffic light signaling you to pay attention. These flags help spot potential issues, but they don’t always mean trouble brews. Healthy people sometimes show flagged results, and normal ones don’t promise perfect health.
Take anemia, for instance, where a patient’s hemoglobin might read 9 g/dL, flagged as low against the usual 12 to 18 range.
Low flags can point to conditions like thrombocytopenia, which means a drop in platelet count. Doctors label this as mild, moderate, or severe based on the numbers. Platelets control bleeding, so low levels lead to easy bruising or bleeding.
Risks jump when counts dip below 20,000, raising chances of severe bleeding. Neutropenia shows up with an absolute neutrophil count under 1,500, graded as mild, moderate, or severe too.
Infection dangers spike if that count falls below 500. These flags guide you, hey, talk to your doctor about what they mean for you.
Common Types of Blood Tests
You know, blood tests come in all shapes and sizes, like a toolkit for peeking inside your body’s engine. Stick around, and we’ll chat about the ones that spot everything from red blood cell counts to cholesterol levels, making sense of what your doc might order next.
Complete Blood Count (CBC)
A complete blood count, or CBC, checks the main parts of your blood. Doctors use it to spot issues like infections or anemia. This test measures red blood cells, white blood cells, and platelets.
Red blood cells carry oxygen around your body. Their normal count runs from 4.2 to 5.4 million per microliter for women, and 4.7 to 6.1 million per microliter for men. Hemoglobin, the protein in red cells that grabs oxygen, should sit between 12 and 18 grams per deciliter.
Hematocrit shows the percentage of blood made up of red cells, with a normal range of 37% to 52%. Imagine your blood as a busy highway; these numbers tell if traffic flows right.
White blood cells fight germs, and their count normally falls between 5 and 10 times 1000 per cubic millimeter. Types include neutrophils, lymphocytes, monocytes, eosinophils, and basophils, each with a job like soldiers in an army.
The absolute neutrophil count comes from multiplying your total white cell count by the neutrophil percentage, aiming for 2,500 to 6,000. Platelets help clot blood to stop bleeding, with a normal range of 150 to 450 times 1000 per cubic millimeter.
Low platelets? You might bruise easily, like bumping into furniture too often. High counts could signal other problems. Talk to your doctor about what these mean for you.
Metabolic Panel
Doctors call the metabolic panel by a few names, like Comprehensive Metabolic Panel or CMP, Blood Chemistry Profile, or Basic Metabolic Panel. This test checks key parts of your blood.
It measures proteins, fats known as lipids, sugar called glucose, electrolytes such as potassium, magnesium, sodium, and calcium, plus enzymes. You might not feel sick until these levels hit critical lows or highs, so the test spots issues early.
The panel assesses kidney function with Blood Urea Nitrogen, or BUN, and creatinine. Normal BUN sits at 7 to 19 mg/dL, while creatinine ranges from 0.6 to 1.1 mg/dL. For liver checks, doctors use a Liver Panel, or LFT, as a specific chemistry test.
Electrolyte shifts, like sodium at 135 to 145 mEq/L, potassium from 3.5 to 5.0 mEq/L, chloride between 96 and 106 mEq/L, or bicarbonate from 22 to 28 mEq/L, might mean doctors adjust your care, say by giving fluids or changing meds.
Glucose should stay between 65 and 99 mg/dL, and calcium from 8.2 to 10.2 mg/dL. Imagine your body as a busy factory; this panel ensures all machines run smooth, catching glitches before they cause big problems.
Lipid Panel
A lipid panel checks the fats in your blood, like cholesterol, to spot risks for heart disease. Doctors call it a cholesterol test too. This common blood draw measures total cholesterol, which mixes LDL, HDL, and 20% of your triglycerides.
LDL earns its nickname as “bad cholesterol” because it can build up in arteries, like unwelcome guests clogging a busy highway. Think of HDL as the helpful cleaner, sweeping away those fats.
The panel often adds non-HDL cholesterol and triglyceride levels for a fuller picture.
High cholesterol boosts heart disease risk, especially if you’re a cancer survivor battling back from treatment. Labs use this test to watch cardiovascular health during cancer care, keeping things in check.
Normal ranges shift based on the lab and your own risk factors, so one person’s okay might flag as high for another. Stay hydrated and chat with your doc about meds before the draw, as they can sway results.
Picture your blood as a river; fats float along, and this panel maps the flow to guide your health journey.
Specialized blood tests (e.g., hormone levels, vitamin deficiencies)
Specialized blood tests dig deeper into your health, like checking hormone levels for thyroid or reproductive issues. Doctors use these to spot problems early. For example, they assess vitamin shortages, such as B12 or folate, which can zap your energy.
Tumor marker tests help in oncology, tracking cancer progress or treatment success. Some tests give clear answers, confirming pregnancy or infections right away.
Results show up in units like mcg/dL or pg/mL, based on what’s tested. Reference ranges vary by lab and your own traits, so one size doesn’t fit all. At-home kits exist for certain checks, but they can’t replace what your doctor orders.
You feel off, get tested for hormone dips, and bam, you find the fix. Stay curious about these tools; they guide better choices.
How to Prepare for a Blood Test
You know that jittery feeling before a blood draw, like waiting for your turn on a roller coaster? Check with your doctor about fasting, say skipping breakfast for eight hours, and hold off on pills like ibuprofen or vitamins that might skew results, so you get the clearest picture of your health.
Fasting requirements
Doctors often ask you to fast before certain blood tests, like those for glucose or cholesterol. This means no food or drink except water for 8 to 12 hours. Think of it as giving your body a clean slate, so results come out spot on.
Your healthcare provider will tell you exactly if you need to fast and for how long. Skip that morning coffee or snack, and you’ll avoid messing up the numbers.
Eating certain foods or drinks right before can throw off your results, especially in lipid panels. One time, a friend of mine chugged orange juice and had to redo the whole test, what a hassle.
Always check with your provider ahead of the blood draw to dodge repeats. They stress this for accurate glucose and cholesterol checks, keeping things smooth for everyone.
Medications and supplements to avoid
Blood tests can reveal a lot about your health, but certain meds and supplements might throw off the results. Talk to your doctor about what to skip before your test, as this keeps things accurate and avoids mix-ups.
- Specific medications or supplements can mess with the accuracy of your blood test results, like when NSAIDs, those over-the-counter pain relievers, tweak platelet counts or kidney function tests, so chat with your provider to dodge any surprises.
- Your healthcare provider might tell you to avoid certain drugs or vitamins before the test, especially if you’re on vitamin supplements like B12 or iron that could sway specialized blood test results, and hey, it’s like giving your blood a clean slate for the real story.
- Discuss all medications and supplements you take with your provider prior to testing, because skipping this step is like playing Russian roulette with your health data, and you want clear, reliable info.
- Over-the-counter medications such as NSAIDs can affect platelet counts or kidney function tests, imagine popping an ibuprofen and then getting a wonky result that sends you into a worry spiral, so always check in first.
- Vitamin supplements like B12 or iron may influence specialized blood test results, and if you keep taking them against advice, you risk false positives or negatives that could lead to needless stress or wrong next steps.
- Medication instructions vary based on the test being performed, for instance, what you avoid for a lipid panel might differ from a hormone check, so treat it like a custom recipe for success and follow your provider’s lead.
- Not following medication guidelines can lead to false positives or negatives, for example, you ignore the rules, get an off result, and suddenly you’re chasing shadows instead of real health fixes.
- Always follow your provider’s instructions about medication use before testing, it’s your best bet to keep results spot-on, and think of it as teaming up with your doc for the win.
Interpreting Your Blood Test Results
You got your blood test report, and now those numbers stare back at you like a puzzle waiting for a solution. Dive right in by spotting if your results show positive for health wins, negative for clear sails, or inconclusive like a foggy morning that needs more checks, and watch out for tricky false positives that might ring false alarms or false negatives that hide real issues.
Positive, negative, and inconclusive results
Blood tests give results as positive, negative, or inconclusive. Negative or normal results mean the test did not spot the substance, germ, cell type, or gene it checked for. These suggest a lower chance of the health issue, but you might need more tests to confirm.
Positive or abnormal results show the test found what it sought, like a germ or gene. They often call for extra checks to verify a disease or infection.
Inconclusive or uncertain results sit in the middle, not clearly positive or negative. Factors such as bad sample collection or test limits can cause them. Take COVID-19 tests, for instance, they hunt for a specific germ in your sample to show presence or absence.
Always chat with your healthcare provider about any result, they help make sense of it all. False positives happen when a test flags something that’s not there, while false negatives miss what is present, so context matters a lot.
Understanding false positives and false negatives
False positives happen when a blood test points to a disease or condition that you don’t really have. Think of it like a smoke alarm going off from burnt toast, not a real fire. These mix-ups spark unnecessary anxiety for many folks.
False negatives occur when the test misses a problem that’s actually there, like overlooking a hidden leak in your roof. Such errors lead to missed diagnoses, which nobody wants. They stay uncommon, yet pop up due to the test type or sloppy conditions.
Pre-test prep plays a big role here; skip fasting, and results might skew. Sample handling matters too, along with the assay’s built-in limits. Test sensitivity and specificity shape how often these slip-ups strike.
Doctors spot inconsistencies with your symptoms, so they often call for repeat tests to confirm.
You know, I’ve heard stories from patients who got a false positive on a cholesterol check, freaking out over nothing until a follow-up cleared it up. Empathy kicks in here, because facing these can feel like a rollercoaster.
Inaccuracies tie back to diet, hydration, or even meds messing with the outcome. Physical activity right before? That throws things off sometimes. Providers step in to sort it out, ordering extra checks if needed.
Always chat with your doctor about what your specific results mean; they guide you through the fog. Imagine joking with a friend, “Hey, my test said I’m superhuman, but turns out it was just a glitch!” These quirks highlight why we double-check everything.
Factors That Can Affect Blood Test Results
Imagine, you chug a big soda before your blood draw, and suddenly your glucose levels spike like a rocket. That quick run to the lab, or popping an aspirin, can twist those hemoglobin counts too, so dig in to learn how everyday choices tweak your lab report.
Diet and hydration
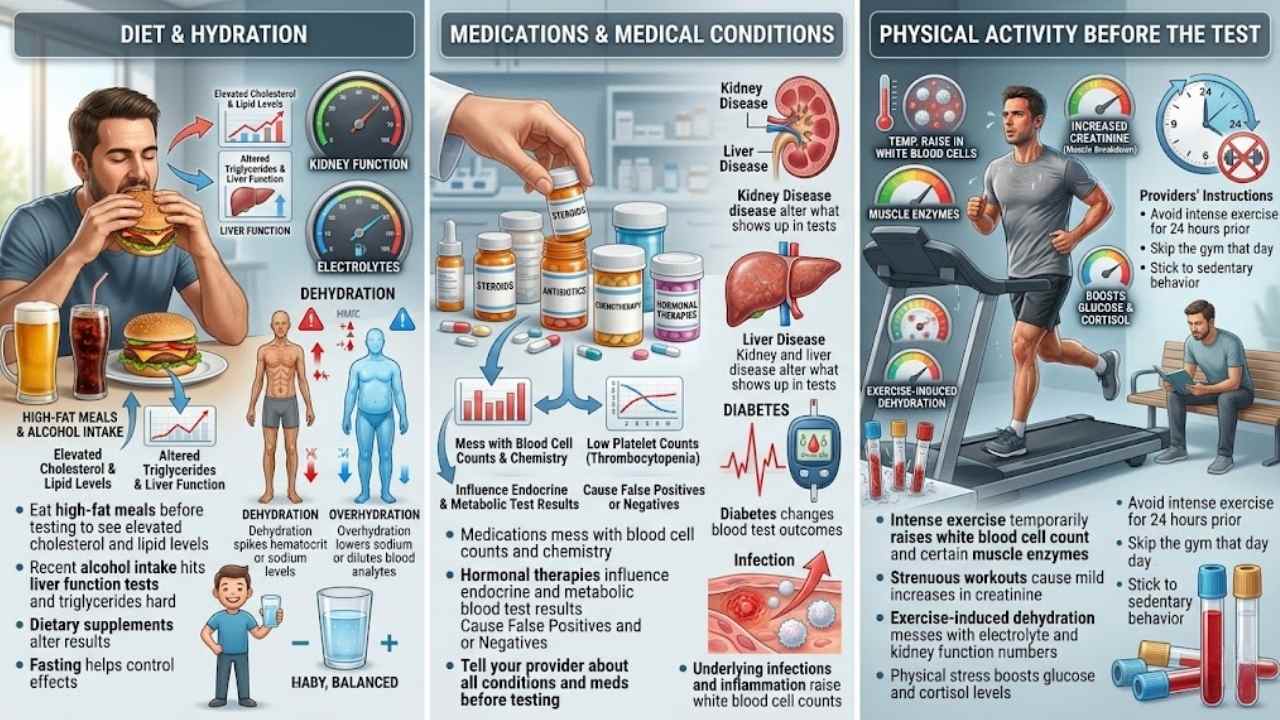
Your diet plays a big role in blood test results, folks. Eat high-fat meals before testing, and you might see elevated cholesterol and lipid levels. Chomp on certain foods or sip beverages, and they can mess with test accuracy.
Recent alcohol intake hits liver function tests and triglycerides hard. Dietary supplements like vitamins and minerals alter results too. Fasting helps control these effects on specific tests, as doctors recommend.
Hydration status changes everything for tests on kidney function and electrolytes. Get dehydrated, and you face falsely elevated hematocrit or sodium levels. Drink too much water, overhydration lowers sodium or dilutes other blood analytes.
Stay balanced, my friends, it’s like keeping your body’s engine running smooth before the big check-up.
Medications and medical conditions
Medications play a big role in your blood test results. Take steroids, they can mess with blood cell counts and chemistry. Antibiotics do the same thing. Chemotherapy often leads to low platelet counts, known as thrombocytopenia.
Hormonal therapies influence endocrine and metabolic blood test results too. Some drugs cause false positives or negatives in diagnostic tests. They create variability in lab results, like a wildcard in a card game.
Medical conditions throw curves at your results as well. Kidney disease alters what shows up in tests. Liver disease does that too. Diabetes changes blood test outcomes. Underlying infections raise white blood cell counts.
Inflammation spikes them even more. These issues act as silent influencers, shifting numbers without warning. Tell your provider about all conditions and meds before testing, it keeps things accurate.
Physical activity before the test
Intense exercise hits your blood test results hard. Think of it like stirring up a calm pond, it muddies the water. Physical activity temporarily raises your white blood cell count and certain muscle enzymes.
Strenuous workouts cause mild increases in creatinine from muscle breakdown. Exercise-induced dehydration messes with electrolyte and kidney function numbers. Physical stress boosts glucose and cortisol levels too.
Providers often give specific instructions on activity limits before testing.
Stick to sedentary behavior, it cuts down variability and boosts accuracy. Doctors recommend you avoid intense exercise for 24 hours prior. You skip the gym that day, your results stay clear and true.
Imagine your body as a quiet machine, no revving up needed. This simple step keeps things on track.
What to Do After Receiving Your Results
You got your blood test report in hand, now chat with your doctor about those numbers, because they can explain what stands out and why it matters to your health. If any value sits outside the normal range, ask about follow-up checks or diet tweaks to get things back on track, and keep digging into more tips in the sections ahead.
Discussing results with your healthcare provider
Talk to your healthcare provider about those blood test results right away. They help you grasp what the numbers mean for your own body, like decoding a secret message made just for you.
Imagine, you spot something odd, and bam, your doctor explains if it’s a big deal or no sweat at all. Providers break down normal ranges versus wonky ones that fit your health story, keeping things crystal clear.
Ask questions upfront before the test even happens, hey, what should I expect, and how do I check these results? Chat about ways to connect after, like a quick call or secure message, so you’re not left hanging.
The CURES Act lets you see results at the same time as your provider, so pick who to ping with worries. If things look off or unclear, they guide you on extra tests or fixes. Even normal results deserve a chat for top-notch care, like catching a curveball early.
Next steps if results are abnormal
You got abnormal blood test results, and that can feel scary. Stay calm, because quick action often turns things around.
- Contact your healthcare provider right away if you spot an abnormal result, especially with symptoms like fatigue or pain; they might order further testing, tweak your treatment, or send you to a specialist for a closer look.
- Doctors often change or add medications when they see odd chemistry or blood count results, so share all your current pills and habits to help them decide.
- Severe issues, like an absolute neutrophil count below 500 or a platelet count under 20,000, call for urgent intervention, so head to the emergency room if your provider says so, no delays.
- Keep an eye on trends over time by using the same lab for repeat tests; this consistency helps spot real changes versus one-off flukes.
- Your provider could suggest lifestyle shifts, like better eating or more exercise, plus extra screenings or follow-up visits to track progress.
- Some abnormal results stem from short-term stuff, such as dehydration or a recent cold, and they might fix themselves on a repeat test, so don’t panic yet.
- For folks with cancer, these odd findings shape treatment choices and supportive care, like adjusting chemo or adding pain relief, to keep you strong.
Final Thoughts
You’ve learned how blood tests reveal your health secrets, from CBC details to reference ranges that guide what “normal” means. These tips make reading results as simple as flipping through a favorite book, no medical degree needed.
Think about your last test; could you spot those high or low flags now? Grasping this stuff empowers you to chat confidently with your doctor, turning confusion into clear next steps.
Talk to your healthcare team about any odd results, like low hemoglobin signaling anemia, and ask for copies under the CURES Act. For more help, check online resources from trusted labs or join health forums to swap stories.
Take charge of your health today; after all, knowledge is the best medicine.
Frequently Asked Questions (FAQs) About Reading Blood Test Results
1. What do those numbers on my blood test report really mean?
Hey, think of your blood test results like a report card from your body, showing levels of things like red blood cells or cholesterol. Don’t sweat it if they seem confusing at first; they’re just snapshots of your health. Chat with your doctor to decode them, like unraveling a mystery novel.
2. How do I know if my blood test results are normal?
Normal ranges vary, like how one size doesn’t fit all in shoes. Check the reference values next to your numbers; if yours fall inside, you’re likely good to go.
3. What if my blood test shows something off?
Oh boy, spotting an abnormal result can feel like finding a flat tire on your car. First, take a deep breath, it’s not always a big deal. Talk to your doctor right away for the full story and next steps.
4. Why are there so many abbreviations on blood test results?
Abbreviations like CBC or LDL are shortcuts, kind of like texting lingo to save space. They stand for specific tests, and most reports include a key to explain them.