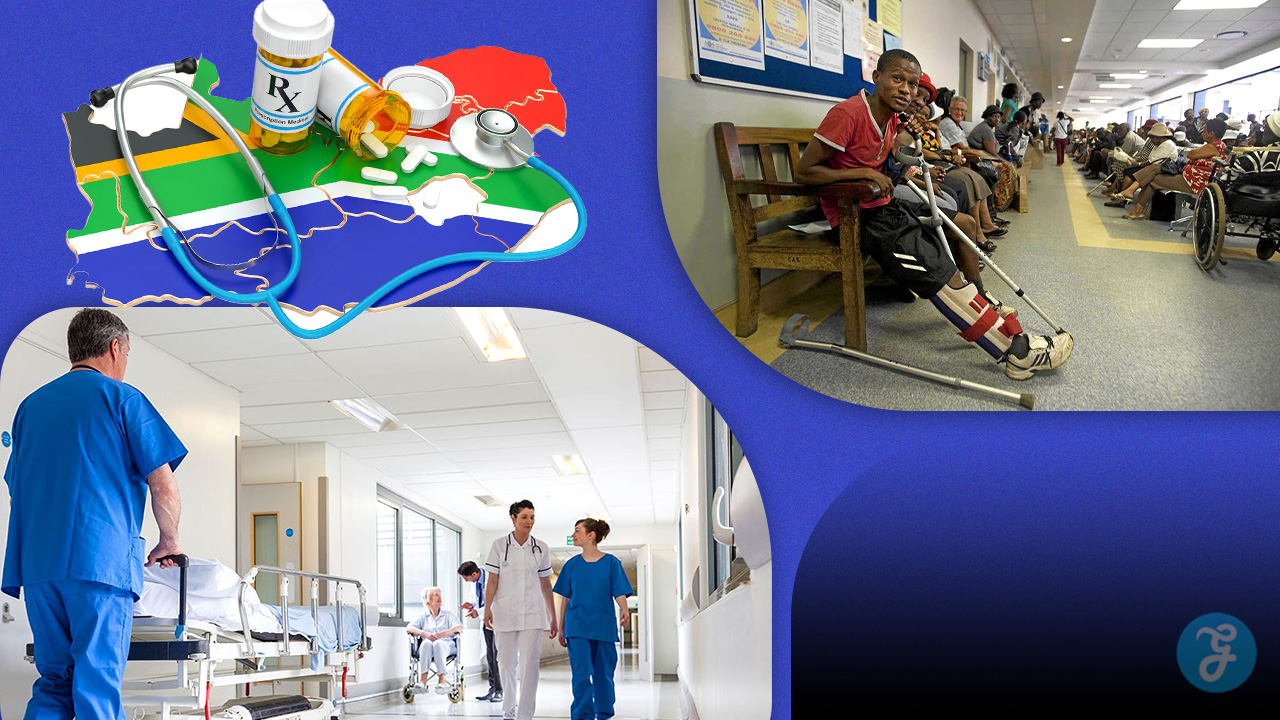
Navigating the dual nature of medical services in the southern tip of Africa requires a deep understanding of how resources are allocated across the population. The current landscape is defined by a sharp divide between state-funded facilities and high-end corporate medical groups. This separation affects everything from daily checkups to life-saving surgeries for millions of citizens and residents.
How We Selected Our 10 Best Private vs Public Healthcare South Africa Differences
To identify the most significant points of divergence in the current medical sector, we analyzed current 2026 data regarding patient outcomes and facility management. Our selection process prioritized factors that directly influence the quality of life and financial stability of those seeking medical attention.
The following benchmarks provided the foundation for our assessment of the two parallel systems.
-
Resource Allocation: Measuring the distribution of medical professionals against the total number of patients they serve.
-
Financial Sustainability: Evaluating how services are funded and the impact of the current 2026 legal freeze on national insurance.
-
Infrastructure Quality: Assessing the age and maintenance levels of buildings and specialized medical equipment.
-
Service Speed: Comparing the time from initial consultation to the completion of specialized procedures.
Once these benchmarks were established, we synthesized the data into the primary factors that define the patient experience in both sectors.
The Essential Landscape of Private vs Public Healthcare South Africa
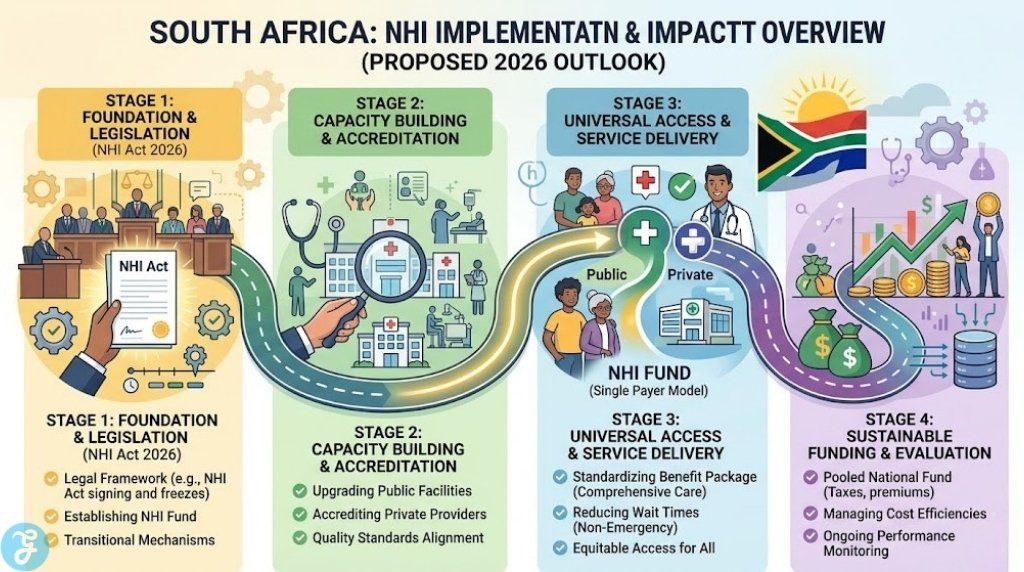
The current structure of medical care in the region is undergoing a period of intense scrutiny as the government attempts to unify services under a single fund. Understanding these differences is vital for navigating the system while the 2026 legal challenges remain ongoing in the courts.
1. Funding and Financial Structures
The primary difference between the two sectors lies in how they generate the revenue required to operate. Public facilities are almost entirely funded by the national government through general taxation and provincial budgets. Private healthcare relies on monthly premiums paid to medical aid schemes or direct out of pocket payments from patients.
Best for:
-
Understanding the economic divide between state reliance and private insurance.
Why We Chose It:
-
Funding determines the availability of medicine and staff across all nine provinces.
-
It highlights the current 50/50 split in spending despite a massive population imbalance.
-
Financial models are at the center of the 2026 National Health Insurance debate.
Things to consider:
-
Public care is often free or highly subsidized for those without any form of income.
While funding sets the stage for what is possible, the actual availability of care depends heavily on who is allowed to enter which facility.
2. Population Coverage and Accessibility
Public health services are mandated to serve any person who enters their doors, regardless of their nationality or financial status. This results in a system that caters to roughly 85 percent of the total population. Private facilities are restricted to those who can prove they have the means to pay or possess an active medical aid membership.
Best for:
-
Assessing the sheer scale of the patient load on the government sector.
Why We Chose It:
-
It explains the overcrowding seen in urban hospitals like Chris Hani Baragwanath.
-
Coverage ratios are a primary driver for the proposed universal health coverage reforms.
-
It illustrates why only about 15 percent of the country uses private services.
Things to consider:
-
Private facilities are often geographically concentrated in affluent urban areas.
The disparity in population coverage leads directly to significant variations in how long a patient must wait for treatment.
3. Patient Waiting Times and Service Speed
Wait times in the public sector are notoriously long for non-emergency procedures and specialist consultations. It is common for patients to wait months or even years for elective surgeries like hip replacements or cataract removals. Private hospitals offer significantly faster turnaround times because they have more staff relative to their patient numbers.
Best for:
-
Patients who require immediate elective procedures without the delay of a queue.
Why We Chose It:
-
Speed of service is often cited as the top reason for joining a medical aid.
-
Long queues in public clinics can lead to poorer health outcomes for chronic conditions.
-
It reflects the efficiency of administrative systems in both types of institutions.
Things to consider:
-
Emergency trauma cases are prioritized in both systems regardless of wait times.
Wait times are not just a matter of staff numbers but also the physical quality of the environment where care is delivered.
4. Infrastructure and Maintenance Standards
Private hospitals are generally characterized by modern architecture and high end interior finishes that resemble hotels. Public facilities range from world class academic hospitals to rural clinics that struggle with basic maintenance issues. The state of the buildings often reflects the management quality of the specific province or district.
Best for:
-
Identifying the physical environment and comfort levels provided during a hospital stay.
Why We Chose It:
-
Infrastructure maintenance is a key performance indicator for health departments.
-
Private wards often offer private rooms with en suite bathrooms and WiFi.
-
Modern facilities tend to attract and retain the most skilled medical professionals.
Things to consider:
-
Many public academic hospitals still possess the most specialized surgical theaters.
The physical environment is secondary to the presence of doctors, where the divide is perhaps most visible.
5. Specialist Concentration and Staffing Ratios
There is a significant drain of medical professionals from the public sector into the private domain. Roughly 80 percent of the nation’s doctors work in private practice to serve only a small fraction of the population. This leaves public hospitals severely understaffed and forces junior doctors to take on massive workloads.
Best for:
-
Understanding the availability of highly specialized surgeons and consultants.
Why We Chose It:
-
It is the primary cause of burnout among public sector healthcare workers.
-
The lack of specialists in rural areas remains a critical challenge in 2026.
-
High salaries and better working conditions lure top talent to private groups.
Things to consider:
-
Medical students are still required to complete community service in the public sector.
Staffing levels are only one part of the equation when it comes to the technical tools used for diagnosis.
6. Diagnostic Technology and Equipment Availability
Private facilities typically have shorter upgrade cycles for high cost equipment like MRI and PET scanners. Public hospitals often face challenges with broken equipment or a lack of specialized technicians to operate them. However, major public research hospitals remain some of the best equipped centers for rare medical conditions.
Best for:
-
Patients requiring advanced imaging or experimental medical treatments.
Why We Chose It:
-
Technology access determines how quickly a disease can be accurately diagnosed.
-
Private groups often invest in robotic surgery and advanced cancer treatments.
-
Public sector procurement delays can lead to long periods of equipment downtime.
Things to consider:
-
Certain specialized scans are only available in a handful of centers nationwide.
Technology and staffing are managed differently depending on whether the entity is a state department or a corporation.
7. Governance and Administrative Oversight
Public healthcare is governed by the National Department of Health and provincial authorities with political oversight. Private groups are corporations listed on the stock exchange and are answerable to their boards and shareholders. This difference in motivation often leads to varied approaches in cost management and service delivery.
Best for:
-
Evaluating the transparency and accountability of medical service providers.
Why We Chose It:
-
Governance affects how budgets are spent and how corruption is managed.
-
Private hospitals must remain profitable while the state must fulfill a human right.
-
Legislative changes in 2026 are forcing both sectors to align their reporting.
Things to consider:
-
Public sector managers are often limited by rigid civil service regulations.
Administrative oversight also impacts the specific types of medications and supplies that are kept in stock.
8. Medicine Supply and Procurement Policies
The public sector uses an Essential Medicines List to ensure the most cost effective drugs are available to the masses. Private doctors have the freedom to prescribe the latest global medications, provided the patient or their medical aid can cover the cost. This can result in a significant difference in the types of chronic medications available to patients.
Best for:
-
Understanding which medications are stocked and how they are dispensed.
Why We Chose It:
-
Procurement cycles in the public sector are prone to stockouts and delays.
-
The private sector uses competitive bidding to source a wider variety of brands.
-
Universal health coverage aims to standardize the formulary across both sectors.
Things to consider:
-
Generic medications are used extensively in both systems to manage total costs.
The choice of medication often comes down to the individual legal and contractual rights of the person receiving care.
9. Legal Protections and Patient Rights
Patients in public hospitals are protected by the Constitution and the Patients’ Rights Charter. Private patients have these same rights plus a contractual agreement with their medical aid and the hospital group. If a dispute arises, the path to resolution can vary between the Health Ombud and private legal channels.
Best for:
-
Understanding the recourse available if medical malpractice or negligence occurs.
Why We Chose It:
-
The Bill of Rights guarantees everyone access to healthcare services in the state.
-
Private contracts often include complex terms and conditions for coverage.
-
Recent legal reforms in 2026 have increased the power of the Health Ombud.
Things to consider:
-
Legal action against the state can be a long and arduous process for patients.
These legal rights finally intersect with the practical reality of how information is stored and shared between doctors.
10. Digital Health Records and Portability
The private sector has made significant strides in implementing electronic health records that follow a patient between specialists. Most public clinics still rely heavily on paper based filing systems which can lead to lost records and repeated tests. The new e-Impilo system in 2026 is attempting to bridge this gap in the government sector.
Best for:
-
Ensuring that your medical history is easily accessible to any doctor you visit.
Why We Chose It:
-
Digital records reduce errors and improve the speed of patient referrals.
-
Paper systems are vulnerable to physical damage and administrative errors.
-
Portability of data is a core requirement for the future National Health Insurance.
Things to consider:
-
Privacy concerns remain a major talking point for both digital and paper systems.
An Overview Of Private vs Public Healthcare South Africa in 2026
Viewing the healthcare system as two separate entities helps clarify the options available to a diverse population. The following comparison highlights the core operational differences between the state-run and corporately managed health sectors.
The data provided below reflects the general experience of users within each system based on the current 2026 metrics.
| Feature | Public Sector Realities | Private Sector Realities |
| Population Share | Approximately 85 percent | Approximately 15 percent |
| Funding Source | Taxes and Government Budget | Medical Aid and Out of Pocket |
| Wait Times | Lengthy for non-emergencies | Typically short and predictable |
| Staff Ratios | High patient to doctor volume | Low patient to doctor volume |
| Facility Access | Open to all residents | Reserved for members or payers |
Our Top 3 Picks and Why?
While every difference is important, three factors stand out as the primary drivers of the South African medical experience.
-
Staffing Ratios: This is the root cause of the quality gap between the two sectors.
-
Funding Models: The way money flows into each system dictates the level of equipment and comfort available.
-
Wait Times: This factor has the most direct and immediate impact on the daily lives of patients.
How to Choose the Right Private vs Public Healthcare South Africa Service?
Deciding which path to take depends entirely on your financial capacity and the urgency of your medical needs. By following a structured decision framework, you can determine which sector will provide the most appropriate care for your specific situation.
-
Assess Financial Capability: Determine if you can afford a monthly medical aid premium or if state care is a necessity.
-
Evaluate Medical Urgency: Identify if your condition requires immediate specialist attention that may be delayed in a public queue.
-
Research Local Facilities: Check the reputation and equipment of the specific hospitals and clinics in your immediate area.
-
Review Chronic Needs: Ensure that the system you choose can provide the specific long term medications you require.
The choice often comes down to a balance between cost and the speed of the service you expect to receive.
| Choose Public Care if… | Choose Private Care if… |
| You have no active medical insurance. | You require elective surgery without a wait. |
| You are seeking basic primary health care. | You prioritize privacy and room comfort. |
| You live in a rural area with no private hospital. | You want to choose a specific specialist. |
The Final Checklist
-
[ ] Confirm your current medical aid status or plan for out of pocket costs.
-
[ ] Locate the nearest government day clinic for your primary health needs.
-
[ ] Secure a copy of your basic medical history in case of a system change.
-
[ ] Identify which specialists are available through your chosen medical plan.
-
[ ] Understand your rights under the South African Patients’ Rights Charter.
Navigating the Future of South African Health
The divide between state and private care remains a defining feature of life in the country as we move through 2026. While the legal battles over national insurance continue, the most effective approach is to remain informed about your rights and the resources available in both sectors. Balancing your personal health needs with a realistic view of the system ensures you receive the best care possible in a changing regulatory landscape.
Frequently Asked Questions About Private vs Public Healthcare South Africa
Is public healthcare in South Africa free?
Answer: It is generally free or highly subsidized at the point of use for the unemployed and low income earners. Higher earners are charged according to a sliding scale based on their annual income and family size.
Can a private doctor refer me to a public hospital?
Answer: Yes, referrals between the two sectors are possible if a patient can no longer afford private care or if a specific specialized service is only available in a public academic hospital.
Is the National Health Insurance (NHI) active in 2026?
Answer: The Act has been signed but implementation is currently frozen due to ongoing legal challenges in the Constitutional Court. A major ruling on the rollout is expected in the second quarter of 2026.
Do public hospitals have the same quality of doctors?
Answer: The doctors in public hospitals are highly skilled and often manage more complex cases than those in private practice. The challenge in the public sector is the lack of resources rather than a lack of medical talent.
How do I join a medical aid for private care?
Answer: You can apply directly to one of the many registered medical schemes in the country or go through an independent broker. There is usually a three month general waiting period before you can claim for most services.