When we look at global happiness and well-being rankings, one Nordic country almost always sits right at the top. You might think it is just the beautiful landscapes or the deep-rooted sauna culture, but a massive part of their national success comes down to how they look after their sick and vulnerable. The Finland healthcare system is widely regarded as a global benchmark for efficiency, equity, and sheer quality of care. If you have ever wondered how they manage to provide top-tier medical services without leaving patients in massive debt, you are certainly not alone.
Today, we are looking closely at how this infrastructure operates on a daily basis. We will walk through the core framework, the recent administrative reforms, and the day-to-day realities for the people living there. From their world-class cancer survival rates to their highly efficient digital networks, there is a lot to unpack. By the end of this guide, you will understand exactly why their medical model works so well and what other nations could learn from their approach to public welfare.
The Core Foundation of the Finland Healthcare System
Before we jump into the specific facts, you need to understand the basic mechanics of how medical care operates in this part of the world. The entire structure relies heavily on tax funding and the core belief that medical attention is a fundamental human right, not a privilege for the wealthy. Everyone living permanently in the country receives high-quality support regardless of their income level or background. This creates a powerful safety net that drastically reduces the stress and anxiety normally associated with falling ill or managing a chronic condition.
In 2023, the government implemented a massive restructuring project to streamline their operations. They shifted the responsibility of organising care from hundreds of individual municipalities to 21 larger wellbeing services counties. This move was specifically designed to standardise the quality of care across the board. It ensures that someone living in a remote northern village gets the exact same standard of treatment as someone living right in the middle of Helsinki. Funding comes primarily from municipal taxes, state subsidies, and small out-of-pocket fees from patients. Because the national government holds the reins on general policy, they can steer public health initiatives on a massive scale while local authorities manage the day-to-day clinics.
Access, Coverage, and Patient Cost Management
One of the biggest hurdles in any medical infrastructure is balancing high-quality treatment with affordable access for the general public. The government tackles this by heavily subsidising the actual cost of medical procedures, meaning patients only pay a fraction of the real bill when they visit a clinic or hospital. They have also built strict financial safeguards into the law to protect individuals who require long-term, continuous care for severe illnesses.
1. True Universal Coverage
When you move to the country permanently, you are entered into the National Health Insurance scheme and issued a Kela card. This small piece of plastic is your golden ticket to the public medical network. It proves your eligibility for social security and medical benefits instantly at any clinic or pharmacy. You do not lose your coverage if you lose your job, change careers, or decide to start your own business. It is tied entirely to your residency status, providing a continuous, unbroken blanket of security throughout your life.
This system dramatically lowers the administrative burden on patients, as they never have to worry about updating private insurance policies, arguing with adjusters over what is covered, or facing sudden cancellations due to pre-existing conditions. It creates a society where changing careers or taking time off to raise children does not mean risking your physical safety.
| Feature of Coverage | Description of Benefit | Impact on the Citizen |
| Kela Card Integration | A single identification card for all medical services. | Eliminates complex paperwork and insurance disputes at the clinic. |
| Employment Independence | Coverage is based entirely on permanent residency. | Allows people to change jobs without fear of losing health benefits. |
| Pre-existing Conditions | No penalties or exclusions for prior medical history. | Guarantees life-saving treatment for chronically ill residents. |
2. Decentralised Local Delivery
Even though the Ministry of Social Affairs and Health sets the national guidelines, the actual delivery of care is handled locally by the newly formed wellbeing services counties. The 21 wellbeing services counties manage their own health centres, specialist clinics, and regional hospitals. This allows local authorities to adapt their resources based on what their specific population actually needs right now.
A county with a higher population of elderly residents in the east can direct more funding towards geriatric care and home nursing, while a younger, urban county in the south might prioritise paediatric clinics and youth mental health services. It is a highly practical approach that prevents a rigid, top-down bureaucracy from ignoring local health trends. Local residents also vote for the county councils, meaning the people making decisions about hospital funding are directly accountable to the patients they serve.
| Administrative Level | Main Responsibility | Practical Outcome |
| National Government | Sets general laws, public health goals, and major funding. | Ensures standardisation and prevents massive regional inequality. |
| Wellbeing Counties | Organises local clinics, hospitals, and social work. | Tailors daily medical services to the actual local demographics. |
| Local Clinics | First point of contact for routine checkups and triage. | Keeps minor issues out of expensive specialist hospitals. |
3. Capped Out-of-Pocket Expenses
You do have to pay small client fees when you see a doctor, but these are strictly controlled by national law to prevent price gouging. For example, a primary care visit might cost around 28 euros, while an emergency department visit could cost nearly 39 euros. To stop these fees from piling up and ruining someone financially, the government enforces a strict annual out-of-pocket maximum. In 2024, this general cap was set at roughly 762 euros.
Once you hit that specific number, your public medical services become completely free for the rest of the calendar year. They also maintain separate, highly regulated price caps for prescription medications and medical travel expenses. This multi-layered safety net provides incredible peace of mind for anyone diagnosed with a chronic condition requiring frequent hospital visits, ensuring that nobody has to choose between buying food and paying for chemotherapy.
| Expense Category | How the Cost is Managed | Maximum Annual Limit |
| Public Clinic Visits | Small flat fees for doctor visits and hospital stays. | Capped at approximately 762 euros per calendar year. |
| Prescription Drugs | Subsidised at the pharmacy counter instantly via Kela. | Capped at approximately 600 euros per calendar year. |
| Medical Travel | Reimburses travel to hospitals if a taxi or train is needed. | Capped at approximately 300 euros per calendar year. |
Preventive Measures and Family Welfare Integration
Treating a disease after it has already caused severe damage is expensive, difficult, and painful for the patient. The smartest medical networks understand that stopping the illness from happening in the first place is always the better option. Here, the primary care network acts as the first line of defence against chronic diseases.
4. Deep-Rooted Focus on Preventive Care
The national medical philosophy heavily leans toward preventing illnesses before they require expensive hospital treatments. Public health campaigns promoting healthy diets, exercise, and smoking cessation are incredibly common and highly effective. They run extensive, free screening programmes for breast, cervical, and bowel cancers across the entire adult population. By catching these potential issues early when they are most treatable, the system saves thousands of lives and millions of euros every single year.
Doctors also routinely prescribe lifestyle interventions, such as guided exercise programmes or dietary counselling, rather than immediately jumping to heavy pharmaceutical solutions for minor blood pressure or cholesterol issues. Furthermore, the government actively uses taxation as a health tool, placing higher taxes on alcohol, tobacco, and sugary items to gently steer the public towards healthier daily choices.
| Preventive Strategy | Method of Implementation | Long-Term Benefit |
| National Screenings | Automatic invitations sent by post for cancer checks. | Drastically lowers mortality rates through early intervention. |
| Lifestyle Prescriptions | Doctors assign diet and exercise plans before medication. | Reduces national reliance on pharmaceuticals for mild conditions. |
| Taxation Policies | Higher taxes placed on tobacco, alcohol, and sugar. | Lowers the national rates of obesity and alcohol-related liver diseases. |
5. The Legendary Neuvola System for Families
One of the absolute crown jewels of their infrastructure is the maternity and child health clinic network, locally known as Neuvola. These clinics offer free, comprehensive monitoring and support for pregnant women and children up to school age. Expectant mothers receive roughly 15 regular checkups, ultrasound scans, and nutritional advice at zero cost before the baby is even born. This system is a huge reason why the country boasts one of the lowest infant and maternal mortality rates on the planet today.
It also helps families transition smoothly into parenthood by offering psychological support, breastfeeding guidance, and parenting classes. They also distribute the famous maternity package, a large cardboard box filled with baby clothes, blankets, and care items, which doubles as a safe first bed for the newborn, ensuring every child gets an equal start in life.
| Neuvola Support Stage | Services Provided to the Family | Main Objective |
| Prenatal Care | Ultrasounds, blood tests, and maternal health checks. | Ensures a safe pregnancy and catches complications early. |
| Postnatal Care | Home visits, breastfeeding support, and infant weighing. | Lowers infant mortality and spots postpartum depression quickly. |
| Early Childhood | Vaccination schedules and speech development tracking. | Prepares the child physically and mentally for the school system. |
6. Seamless Integration of Social and Health Services
They recognise that physical health is deeply connected to a person’s social and financial circumstances. You cannot simply treat a patient’s physical symptoms if they are homeless, struggling with severe addiction, or completely isolated at home. The system integrates medical care directly with social welfare services, such as elder care, mental health support, and substance abuse rehabilitation programmes.
This holistic approach ensures that vulnerable individuals receive comprehensive, wrap-around help rather than just a quick medical fix before being sent back into a harmful environment. For example, social workers often operate in the exact same buildings as general practitioners, allowing doctors to instantly refer a patient who might be suffering from domestic violence or severe financial stress, addressing the root cause of their physical ailments.
| Integrated Service | How It Connects to Healthcare | Target Demographic |
| Housing First | Provides permanent housing before treating addictions. | Chronically homeless individuals with complex medical needs. |
| Co-located Social Work | Social workers share office space with primary care doctors. | Families facing financial ruin, domestic abuse, or severe stress. |
| Addiction Rehab | Medical detox combined with long-term social reintegration. | Patients struggling with severe alcohol or substance dependencies. |
Medical Expertise and Specialised Treatment
Having a highly accessible medical network means very little if the actual quality of care is poor. Thankfully, the standards for medical practice and clinical outcomes in this Nordic nation are incredibly high. They maintain strict educational requirements for their clinical staff and invest heavily in modern medical infrastructure.
7. Highly Educated Medical Professionals
Becoming a doctor or a nurse here is highly competitive and requires years of rigorous academic training. Because university education is entirely free, medical schools can select candidates purely based on academic merit and aptitude rather than their financial ability to pay massive tuition fees. This creates a workforce that is exceptionally bright and deeply committed to the profession. Nurses also hold a significant amount of responsibility and autonomy within the primary care network.
In many health centres, an experienced nurse will be your first point of contact, fully trained to assess your condition, prescribe basic medications, and provide medical advice without needing a doctor in the room. This efficient delegation of tasks allows fully trained doctors to focus their time strictly on complex diagnostic puzzles and severe medical emergencies.
| Profession | Educational Requirement | Role in the System |
| General Practitioner | Six-year university degree plus practical licensing. | Handles complex diagnoses, chronic disease management, and referrals. |
| Registered Nurse | Three to four-year university of applied sciences degree. | Conducts first-line triage, minor treatments, and patient education. |
| Specialist Doctor | Five to six additional years of training after basic degree. | Operates in regional hospitals handling surgeries and severe illnesses. |
8. Top-Tier Cancer Survival Rates
When we look at serious illnesses, the clinical outcomes speak for themselves on the global stage. The country consistently reports some of the highest cancer survival rates across the whole of Europe. Once a patient is diagnosed through their aggressive screening programmes or a primary care visit, they are quickly routed into specialised hospital districts like the Helsinki University Hospital network.
These tertiary care centres house state-of-the-art oncology departments, giving patients immediate access to the latest therapies, targeted radiation, and clinical trials without facing administrative delays. They utilise a highly personalised medicine approach, sequencing the genetics of tumours to find the exact chemical compound that will destroy the cancer cells with the least amount of collateral damage to the patient.
| Cancer Care Aspect | How the System Handles It | Outcome for the Patient |
| Early Detection | Free national screening for bowel, breast, and cervical cancers. | Tumours are found at stage one when they are highly curable. |
| Specialised Hubs | Complex cases are routed to massive university research hospitals. | Access to the absolute best surgeons and oncologists in the region. |
| Personalised Therapy | Genetic testing of tumours to match specific pharmaceutical drugs. | Higher survival rates with fewer severe side effects from treatments. |
9. Efficient Emergency Response Networks
Because the country has vast, sparsely populated areas, especially in regions like Lapland, moving patients quickly in an emergency is a massive logistical challenge. They solve this through a highly coordinated national emergency response grid. You simply dial 112, and a centralised dispatch unit assesses the situation instantly using advanced triage protocols.
They use a mix of highly trained paramedics, rapid response vehicles, and even rescue helicopters known as FinnHEMS to reach remote patients within minutes. Paramedics here are highly educated, often holding degrees in nursing, meaning they can start advanced life-saving treatments right there on the living room floor before the ambulance even begins moving. Emergency departments are also specifically geared to handle multimorbid patients safely.
| Emergency Asset | Primary Function | Operational Advantage |
| Centralised 112 Dispatch | Single contact number for police, fire, and medical rescue. | Eliminates confusion and deploys the closest correct unit instantly. |
| FinnHEMS Helicopters | Airborne medical units with doctors on board. | Reaches isolated rural patients within a 30-minute critical window. |
| Advanced Paramedics | University-educated medical staff operating mobile clinics. | Begins complex medical interventions at the scene of the accident. |
Digital Innovation and Future Preparedness
A modern medical network cannot survive on paper records and outdated administrative processes. Finland is widely recognised as a global pioneer in digital health technology. They have spent the last two decades building an interconnected digital infrastructure that eliminates paperwork, reduces medical errors, and gives patients total control over their own health data.
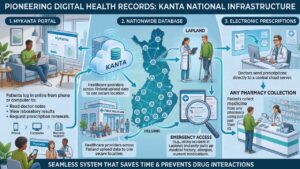
10. Pioneering Digital Health Records
They are way ahead of the curve when it comes to medical technology. The national digital infrastructure, called Kanta, allows patients to log in and view their medical records, check laboratory results, and request prescription renewals online from their phone or computer. Healthcare providers across the entire country can access these records securely with your permission.
This means that if you live in Helsinki but have a skiing accident while holidaying in Lapland, the attending emergency doctor can instantly pull up your medical history, allergies, and current medications on their tablet. It is a seamless system that saves incredible amounts of time, prevents dangerous drug interactions, and completely eliminates the need for patients to carry paper files between different specialist appointments.
| Kanta Digital Feature | How It Works | Benefit to the System |
| MyKanta Portal | Patients log in online to read doctor notes and test results. | Empowers patients to take charge of their own health information. |
| Electronic Prescriptions | Doctors send prescriptions directly to a central cloud server. | Patients can collect medicine from any pharmacy using just their ID. |
| Nationwide Database | All public and private clinics upload data to one secure location. | Prevents duplicate blood tests and ensures doctors have full context. |
11. Heavy Investment in Research and Development
The government and private sectors invest heavily in health technology, genetics, and biotechnology to stay ahead of future diseases. The country passed a specific Biobank Act to securely collect and store tissue samples and genetic data from hundreds of thousands of willing citizens. These Finnish biobanks are highly valued globally for medical research, helping scientists understand complex hereditary diseases on a much deeper level.
This heavy investment drives incredible innovations that eventually trickle down into everyday patient care at the local clinic level. They are actively developing and deploying artificial intelligence tools to help radiologists read X-ray scans faster and to help primary care doctors spot early statistical warning signs of chronic diseases buried deep in patient bloodwork data.
| R&D Focus Area | Current Application in the Country | Future Potential |
| National Biobanks | Collecting genetic data via the massive FinnGen research project. | Discovering the genetic roots of rare diseases and common cancers. |
| Artificial Intelligence | Using software to analyse medical imaging and hospital workflows. | Speeding up diagnoses and reducing the administrative workload on doctors. |
| Health Tech Startups | Incubating companies that build wearable health monitors like Oura. | Shifting healthcare from hospital beds to continuous daily monitoring. |
12. Proactive Adaptation to an Ageing Population
Like many developed nations, they are facing the severe demographic challenge of a rapidly ageing population. As people live much longer, they naturally require significantly more medical support. The system is actively adapting by investing heavily in home-care services, geriatric medicine, and smart assistive technologies rather than just building more traditional hospitals.
Instead of automatically placing elderly citizens into crowded care homes, they provide visiting nursing support, home physical therapy, and house modifications to help seniors live independently and safely in their own familiar surroundings for as long as possible. They utilise automated medicine dispensers and remote vital sign monitors to keep a close eye on elderly patients without forcing them to travel to a clinic every single week.
| Ageing Care Strategy | Method of Delivery | Benefit to the Senior Citizen |
| Preventive Home Visits | Nurses visit citizens over 75 to assess fall risks and memory. | Catches dementia early and prevents devastating hip fractures. |
| Assistive Technology | Installing automated pill dispensers and emergency wristbands. | Allows seniors to manage their medication safely without daily nurses. |
| Home Nursing Support | Medical staff visit daily to assist with hygiene and wound care. | Keeps the elderly comfortable in their own homes instead of wards. |
Workplace Support, Mental Health, and Public Trust
A truly effective medical model does not just exist inside hospitals; it extends into the workplace, schools, and the general community. The country places a heavy legal obligation on employers to keep their staff healthy, which takes a massive burden off the public clinics.
13. A Robust Occupational Healthcare Network
Employers are legally required to provide preventive occupational healthcare for all their employees. Many modern companies actually go way above and beyond the legal minimum, offering free access to private general practitioners, specialists, and physiotherapists. Because employees can use these private occupational clinics for free, it takes a massive amount of pressure off the public health centres.
It allows workers to bypass public wait times for minor ailments like a sinus infection or a sprained ankle, ensuring the workforce stays healthy, productive, and off long-term sick leave. This dual-track system means that those who are employed get fast private care, which ironically shortens the queue in the public system for the unemployed, children, and the elderly who rely entirely on the state clinics.
| Occupational Care | Legal Requirement vs Reality | Systemic Impact |
| Preventive Checks | Employers must ensure the workspace is physically safe. | Reduces chronic back pain and repetitive strain injuries in workers. |
| Private Clinic Access | Many firms pay for staff to see private doctors instantly. | Keeps employees working and slashes wait times in public hospitals. |
| Mental Health Focus | Firms increasingly offer free therapy sessions for burnout. | Prevents long-term disability leave caused by severe workplace stress. |
14. Growing Focus on Mental Health
Historically, mental health was somewhat stigmatised around the world, but the government has made massive strides in bringing it to the absolute forefront of their public health strategy. There is a strong national push to make mental health services much more accessible, particularly for young people. They are integrating psychological support directly into schools and basic healthcare centres, normalising the act of asking for help before a crisis hits.
They have introduced low-threshold walk-in clinics for youth experiencing anxiety and have debated therapy guarantee laws to ensure rapid access to psychotherapy. By treating mental health with the exact same urgency and funding as physical health, they are actively working to reduce the rates of severe depression and behavioural disorders across the population.
| Mental Health Initiative | How It Is Implemented | Expected Outcome |
| School Psychologists | Placing trained counsellors directly inside educational buildings. | Catches anxiety and bullying issues in teenagers before they escalate. |
| Low-Threshold Clinics | Walk-in centres where no prior doctor referral is needed. | Removes the bureaucratic barriers to getting immediate emotional help. |
| Therapy Subsidies | Kela reimburses a large portion of long-term rehabilitative therapy. | Makes multi-year psychological treatment affordable for the middle class. |
15. Unwavering Public Trust
A public health strategy only works if the people actually believe in it. Surveys consistently show that Finnish citizens have an incredibly high level of trust in their medical professionals, scientists, and government health institutions. When the authorities issue health guidelines, advise dietary changes, or roll out seasonal vaccination programmes, the public generally complies without widespread resistance or conspiracy theories.
This high level of cultural trust encourages people to seek care early when they need it, follow the medication instructions their doctor gives them, and makes managing national health crises significantly easier for the government. The authorities maintain this trust by communicating transparently, relying entirely on peer-reviewed science, and keeping political interference out of basic medical policies.
| Source of Public Trust | How It manifests in Society | Benefit to Public Health |
| Transparent Institutions | Health agencies publish all data and reasoning openly online. | Prevents the spread of medical misinformation and panic. |
| Scientific Reliance | Policies are drafted by medical experts, not just politicians. | Ensures that health laws actually make medical and logical sense. |
| High Compliance Rates | Citizens voluntarily take vaccines and attend cancer screenings. | Creates herd immunity and keeps the overall population healthier. |
Comparing the Finland Healthcare System to the World
When you place this Nordic model side-by-side with systems like the United States, the differences in philosophy are instantly obvious. In the US, care is largely tied to private insurance provided by employers, leading to incredibly high administrative costs, massive co-pays, and crippling medical debt for citizens who happen to fall through the cracks of the economy. The Finnish approach prioritises human equity above all else, ensuring that a person’s bank account never dictates the quality of life-saving care they receive in an emergency.
Even when compared to other highly developed European nations, they stand out significantly. While countries like Germany or France have excellent medical outcomes and brilliant doctors, the Finnish integration of digital records through the Kanta system is miles ahead of the curve. Their ability to track a patient’s digital footprint seamlessly from a local community pharmacy all the way to a specialist surgical ward in the capital is a logistical dream that many other advanced nations are still struggling to build today.
Navigating Challenges and Wait Times
No system is completely perfect, and they certainly face their own ongoing logistical hurdles. The most persistent complaint from citizens usually revolves around long waiting times for non-urgent, specialised care. Because the system logically prioritises severe and life-threatening conditions first, someone needing an elective knee replacement or a non-urgent dermatology check might have to wait several months. There is also a growing concern about a severe shortage of nurses and care workers, especially as the older population continues to grow rapidly and demand more daily assistance in their homes.
To combat this, the government introduced a strict statutory care guarantee. As of recent updates, the law dictates that a patient must receive access to non-emergency primary care within 14 days of their initial contact. The massive restructuring into the 21 wellbeing services counties was specifically executed to help manage these exact administrative bottlenecks and staffing challenges, though it will naturally take some time to see the final results of such a massive shift in national policy.
Final Thoughts
The success of the Finland healthcare system is not just a happy accident of geography or wealth. It is the direct result of deliberate policy choices, a deep cultural commitment to social equality, and a willingness to embrace new digital technology to make life easier for patients. By focusing heavily on preventive care, supporting families from the moment a child is conceived, and capping out-of-pocket costs, they have built a resilient and highly effective medical infrastructure.
While they certainly face modern challenges with staffing and wait times, their model continues to offer incredibly valuable lessons for any nation striving to improve the health, happiness, and security of its citizens.
Frequently Asked Questions (FAQs) About Finland healthcare system
1. Is healthcare completely free in Finland?
No, it is not completely free at the point of use. While the infrastructure is heavily subsidised by public taxes, adults do pay small out-of-pocket fees for doctor visits, hospital stays, and prescriptions. However, the government sets a strict annual cap on these costs to prevent financial hardship. Services like maternity checkups and child clinic visits are completely free.
2. Can international students or expats use the public medical network?
Yes, if you have a registered municipality of residence, you are legally entitled to use the public services on the exact same basis as a native citizen. International university students are also covered by the Finnish Student Healthcare Service, which provides excellent primary and mental health support for a small annual union fee.
3. What is the statutory care guarantee?
This is a strict legal framework designed to cut down on long wait times. Following recent legal amendments, the law requires that patients seeking non-emergency primary care must be given an appointment within 14 days. If the public clinic cannot meet this deadline, they must arrange and pay for the patient to be treated elsewhere, often at a private clinic.
4. How are pharmacies regulated differently here?
Unlike many countries where you can buy basic pain relief at a grocery store or petrol station, you can only buy medications from officially approved, highly regulated pharmacies. The national health agency strictly regulates these pharmacies to ensure patient safety and to manage the distribution of digital e-prescriptions safely.
5. How do digital prescriptions work if I travel abroad?
Because the country uses an advanced digital database for all prescriptions, your doctor simply uploads the details to the central cloud. You can walk into any pharmacy in the country, hand over your ID, and collect your medicine. If you are travelling within certain other European countries, you can often use your passport to access these digital prescriptions across borders thanks to cross-EU data integration.