Do you ever wake up in the morning and feel like something is just completely off? Your bed feels heavier than usual, and getting out of it takes all your energy. Maybe you have felt this way for weeks or even months. You tell yourself it is just a bad day, but deep down, you know something is different. I want you to know right now that you are definitely not alone in this struggle. Millions of people experience depression every single year, and many of them feel totally confused about what is happening to them. I have found that understanding the facts makes the journey much easier.
Here is a secret a lot of people miss. Depression is not just sadness. Sadness comes and goes like clouds passing through the sky. Depression sticks around and affects how you think, feel, and move through your day.
It can make you feel empty, tired, and disconnected from the world around you. Understanding depression means recognizing that this condition is real, medical, and treatable. I am going to walk you through exactly what you need to know. We will break down what depression actually is, what causes it, and practical strategies that work. So, grab a cup of coffee or tea, and let’s go through it together.
Understanding Depression: Beyond Sadness And Emptiness
Depression goes far beyond feeling sad or down for a day or two. It is a serious mental health condition that affects how you think, feel, and function in daily life.
Definition of Depression
Clinical depression is a serious mood disorder that shifts your brain chemistry. Your energy drains, and even simple tasks feel like climbing a mountain. Mental health professionals define depression as a persistent state of emotional distress that lasts for weeks or months, not just a temporary bad mood. This condition impacts your well-being in ways that sadness simply cannot.
A 2025 Gallup survey revealed an eye-opening statistic. They found that 18.3 percent of United States adults currently have or are being treated for depression. That is roughly 47.8 million Americans going through exactly what you might be feeling.
Depression is not a sign of weakness; it is a sign that you have been strong for too long.
Numbness often replaces sadness in clinical depression, leaving you feeling hollow or disconnected from life. You might go through the motions without feeling much of anything, which can feel even scarier than crying.
How Depression Differs from Sadness or Grief
Sadness hits you like a storm, but it passes. Grief wraps around your heart after loss, yet it slowly loosens its grip over time. Depression operates on a different level entirely. This mood disorder does not need a specific trigger to show up at your door.
Research from the Queensland Brain Institute points out that clinical depression actually causes your amygdala to become overactive. This means your brain overemphasizes negative emotions, creating a heavy fog that sadness alone cannot produce.
The key difference lies in duration and intensity. Sadness typically lasts days or weeks, while depression can linger for months or years. Mental health professionals recognize that depression operates differently, affecting your sleep, appetite, energy, and ability to concentrate. You might still laugh at a joke while grieving, but depression often steals that ability entirely.
Common Symptoms of Depression
Depression shows up differently for each person, and the symptoms go way beyond just feeling sad all the time. Your body, mind, and daily life can all feel the weight of depression in ways you might not expect.
Internal Feelings
The way you process emotions can change dramatically when depression takes over your mental health.
- Persistent sadness creeps in and stays around for weeks or months, coloring everything you do.
- Numbness takes over your emotional world, leaving you unable to feel joy, excitement, or even anger.
- Hopelessness wraps around your thoughts, making you feel like things will never get better.
- Guilt weighs heavily on your shoulders, even when you have done nothing wrong.
- Low self-worth makes you question your value and abilities constantly.
Reactions to the World
Depression also changes how you interact with the people and responsibilities around you.
- Irritability and anger flare up more often than they used to, sometimes over small things.
- Anxiety creeps alongside your mood disorder. A 2026 National Institutes of Health report notes that 19.1 percent of adults face anxiety disorders, which frequently overlap with depression.
- Loss of interest in activities you once loved hits hard and fast.
- Difficulty concentrating affects your work, school, and relationships.
- Emotional distress manifests as feeling overwhelmed by ordinary situations, making simple decisions monumental.
Energy and Sleep Issues
Depression shows up in your body, draining your physical reserves and disrupting your natural rhythms.
- Sleep problems hit hard. According to sleep specialists, waking up at 3 AM and being unable to fall back asleep is a classic sign called terminal insomnia.
- Fatigue and low energy make even simple tasks feel impossible, turning a walk to the kitchen into a battle.
- Slowed movements and speech patterns develop gradually, making your body feel heavy.
- Appetite changes come with mood disorders, causing some to lose weight and others to eat constantly for comfort.
- Sexual dysfunction affects intimacy and relationships, adding shame to your well-being struggles.
Pain and Discomfort
Many people do not realize that clinical depression can actually hurt physically.
- Physical pain and aches spread across your body without clear cause, leaving your back and neck stiff.
- Headaches strike frequently and last for hours or days, resisting standard medication.
- Digestive issues create stomach problems, nausea, and discomfort as your gut rebels against mental stress.
- Chest tightness and heart palpitations cause real alarm, though they are often linked to accompanying anxiety.
- Tremors or shaking occur in your hands and limbs, reflecting the turmoil happening inside.
Symptoms in Children, Teens, and Older Adults
Depression shows up differently depending on a person’s age, and knowing what to look for matters a lot.
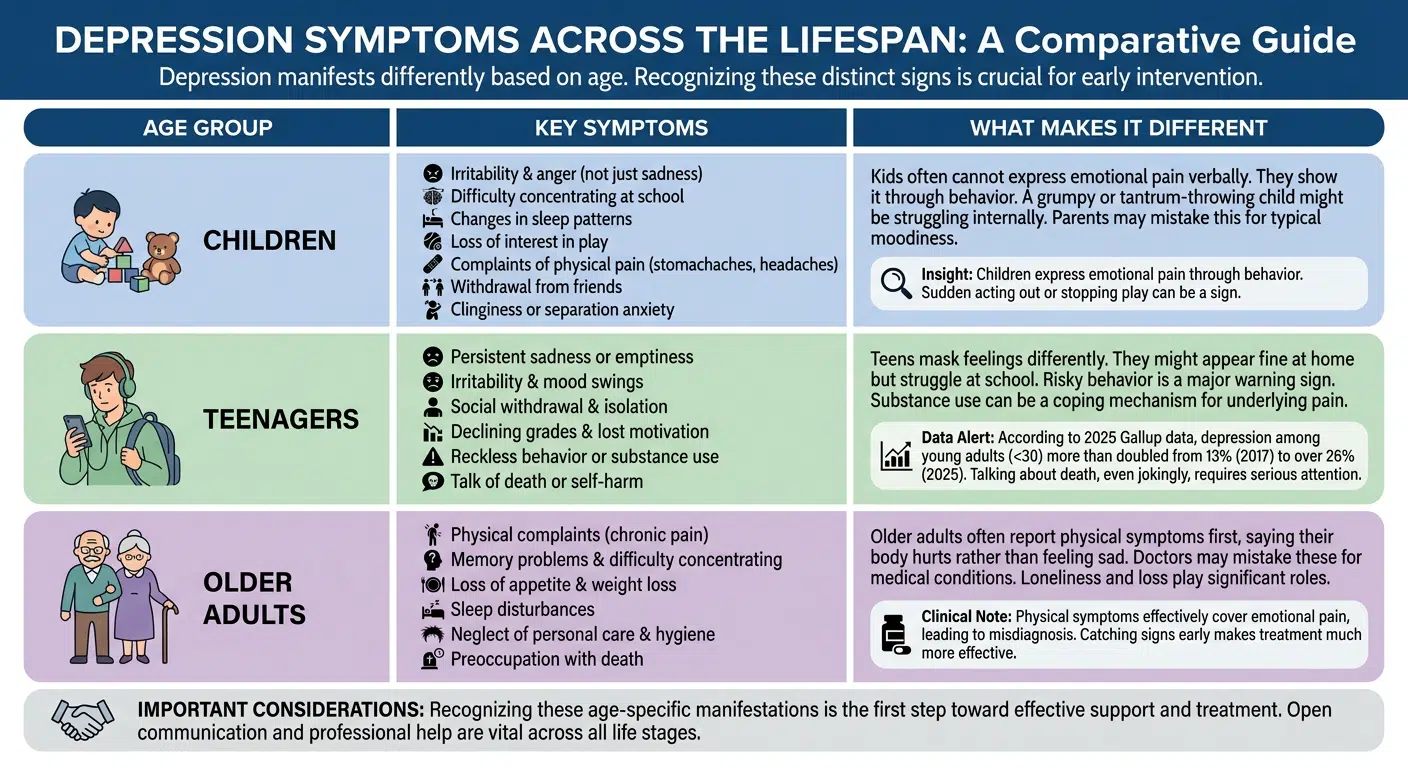
| Age Group | Key Symptoms | What Makes It Different |
|---|---|---|
| Children |
|
Kids cannot always express emotional pain in words. They show it through behavior instead. A child might seem grumpy or throw tantrums when really they are struggling inside. Parents often miss it because they chalk it up to typical moodiness. |
| Teenagers |
|
Teens mask feelings differently than younger kids do. They might seem fine at home, but struggle at school. Risky behavior becomes a warning sign. Some teens use substances to cope with pain underneath. |
| Older Adults |
|
Older adults often report physical symptoms first. They might say their body hurts instead of saying they feel sad. Doctors sometimes mistake these for medical conditions, missing the real issue. Loneliness and loss play major roles in this age group. |
Children express emotional pain through behavior, making it tricky to spot. A kid who suddenly acts out or stops playing might be depressed, not just being difficult.
Teenagers face unique pressure from peers, school, and social media. According to 2025 Gallup data, depression among young adults under 30 more than doubled from 13 percent in 2017 to over 26 percent in 2025. Talking about death, even as jokes, requires having serious conversations with adults.
Older adults experience different life circumstances that fuel despair. Physical symptoms cover emotional pain so effectively that doctors prescribe pills for the wrong thing. Catching these signs early makes treatment much more effective.
Causes and Risk Factors of Depression
Depression does not spring from nowhere. It develops through a mix of brain chemistry, life experiences, and outside pressures.
Biological Factors
Your brain chemistry plays a massive role in how you feel each day. Neurotransmitters like serotonin, dopamine, and norepinephrine act as messengers in your brain, controlling mood, motivation, and energy levels.
Imbalances in these chemical messengers can directly affect your emotional well-being. Genetics matter too. If your parents or grandparents struggled with mood disorders, you face a higher risk yourself.
A 2021 clinical review published by Talkspace noted that chronic depression can literally cause your hippocampus to shrink over time. Fortunately, the same research confirms that proper treatment can heal and reverse this shrinkage.
Physical health conditions can trigger mood changes as well. Hormonal shifts, thyroid problems, and chronic illnesses all connect to symptoms of emotional distress.
Psychological and Social Factors
Your thoughts and experiences shape depression in powerful ways. Trauma from childhood, stress at work, or loss of a loved one can trigger emotional distress that develops into clinical depression.
Social isolation makes things worse because humans need connection to thrive. A 2025 World Health Organization report identified teenagers as the loneliest age group worldwide and linked severe social disconnection to hundreds of thousands of premature deaths annually.
People who face rejection, loneliness, or major life changes struggle with mood disorders more often. Negative thinking patterns, low self-esteem, and perfectionism create mental traps that feed depression.
Support systems matter more than most people realize. Strong friendships, caring family members, and community connections act as buffers against depression, helping people recover faster and experience better well-being.
Life Changes and Loss
External stressors can push someone into a depressive episode, even if they have no family history of mental health struggles.
- Major life changes like job loss, divorce, or moving to a new city can spark depression by shaking your routine.
- Grief from the loss of loved ones opens the door to depression, transforming into a clinical condition if it persists too long.
- Social isolation cuts people off from meaningful connections, increasing vulnerability when established relationships fade.
- Trauma and abuse create deep wounds that trigger depressive symptoms, setting the stage for mood disorders later in life.
Stress and Health Factors
Physical tolls and daily pressures also weigh heavily on your emotional state.
- Chronic illness and pain drain physical and emotional energy, leaving little room for joy.
- Substance abuse and addiction fuel depressive episodes, altering brain chemistry in ways that deepen sadness.
- Stress at work or school piles up over time, damaging self-esteem and confidence through constant pressure.
- Seasonal changes affect mood through reduced sunlight exposure. Experts highly recommend using a 10,000-lux light therapy box to combat this specific environmental trigger.
Types of Depression
Depression shows up in different forms. Knowing which type affects you matters more than you might think, so keep reading to learn what sets each one apart.
Major Depressive Disorder (MDD)
Major Depressive Disorder strikes millions of people each year, making it one of the most common mental health conditions worldwide. In fact, roughly 21.4 million people in the United States experienced a major depressive episode in 2024 alone.
MDD differs from regular sadness because it involves a serious condition that demands proper treatment and support. Your brain chemistry shifts during this time, making it much harder to regulate emotions and motivation.
According to clinical guidelines, you might experience several of these core signs:
- An overwhelming sense of numbness or emptiness.
- A complete loss of interest in activities you once loved.
- Severe changes in your appetite or daily sleep habits.
- Fatigue that weighs on you like a heavy blanket you cannot shake off.
Persistent Depressive Disorder (Dysthymia)
While major depressive disorder hits hard and fast, persistent depressive disorder takes a different route. This condition, also called dysthymia, operates like a low-grade fever that never quite breaks.
People with dysthymia experience a depressed mood that sticks around for at least two years in adults, or one year in children and teens. The symptoms feel less intense than major depression, but they refuse to leave.
Persistent depressive disorder creates a sneaky trap. You adapt to the low mood over the years and simply forget what feeling normal actually feels like.
The good news is that therapy and other interventions work extremely well for persistent depressive disorder. Building a solid support system makes a real difference in helping someone break free from dysthymia’s long-term grip.
Seasonal Affective Disorder (SAD)
Unlike dysthymia, which lingers year-round, seasonal affective disorder has a recurring seasonal pattern. This mood disorder appears when daylight hours shrink, typically during fall and winter months.
Reduced sunlight disrupts your body’s natural rhythms, lowering serotonin levels and throwing your internal clock off balance. Symptoms mirror major depressive disorder, including emotional distress, numbness, and low energy.
Light therapy is the primary, proven treatment for seasonal affective disorder. Sitting in front of a 10,000-lux bright light box for thirty minutes each morning can lift your mood significantly and reset your internal clock.
Treatment Options for Depression
Depression responds exceptionally well to treatment. Doctors combine medication, talk therapy, and lifestyle changes to help people feel better, and you have real options that work.
Pharmacological Interventions
Medications called antidepressants work to fix chemical imbalances in your brain that fuel mood disorders. Finding the perfect fit takes time, so patience matters here as your doctor adjusts your plan.
Science has advanced rapidly in recent years, offering powerful new options beyond standard daily pills:
- Auvelity: Approved by the FDA in August 2022, this oral pill works in just one week by targeting NMDA receptors. This is a huge shift from traditional SSRIs that often take four to six weeks to kick in.
- Zurzuvae: Approved in August 2023, this is the very first oral pill specifically designed to treat postpartum depression rapidly through a 14-day course.
- SSRIs: Selective serotonin reuptake inhibitors remain the most common daily medications for correcting chemical imbalances safely over time.
Mixing medication with therapy creates powerful results for managing emotional distress. Well-being improves significantly when you stick with your treatment plan and give it enough time to work.
Psychological Therapies
Psychological therapies work by helping you change how you think and feel about your life. Cognitive behavioral therapy, or CBT, teaches you to spot negative thought patterns and swap them for healthier ones.
A therapist guides you through this process, asking questions that help you see situations from fresh angles. Interpersonal therapy focuses on your relationships and how they directly affect your mood disorder symptoms.
Your therapist becomes a true partner in your recovery journey, not just someone who listens and nods. Acceptance and commitment therapy teaches you to live with difficult feelings instead of fighting them constantly.
Many people find that combining talk therapy with other treatment options works best for their specific needs. These approaches give you real tools to manage anxiety and build resilience when depression tries to pull you down.
Advanced Medical Procedures
Science keeps pushing mental health treatment forward for those who need extra support.
- Transcranial Magnetic Stimulation (TMS) uses magnetic pulses to activate nerve cells in the brain. Studies show that about 50 percent of patients respond well to standard TMS, and up to 30 percent achieve full remission.
- Ketamine Infusion Therapy delivers small doses of ketamine through an IV, acting quickly on brain chemistry to produce results in hours or days.
- Esketamine Nasal Spray (Spravato) offers a faster-acting option for treatment-resistant depression. While treatment can cost up to $1,500 per session without insurance, Janssen Pharmaceuticals reported in 2024 that the average out-of-pocket cost with insurance is under $500 per month for eligible patients.
- Deep Brain Stimulation (DBS) involves surgeons implanting electrodes to help restore normal brain function in severe cases.
New Approaches and Devices
Modern therapy now includes unique tools to rewire your brain safely.
- Psychedelic-Assisted Therapy incorporates controlled doses of substances like psilocybin alongside professional counseling.
- Light Therapy Boxes expose your eyes to bright light that mimics natural sunlight to treat Seasonal Affective Disorder.
- Virtual Reality Exposure Therapy places patients in computer-generated environments to practice coping skills safely.
- Mindfulness-Based Cognitive Therapy combines meditation practices with cognitive techniques to prevent depression relapse.
- Neurofeedback Training teaches your brain to self-regulate by monitoring your brainwaves in real-time.
Strategies for Managing Depression
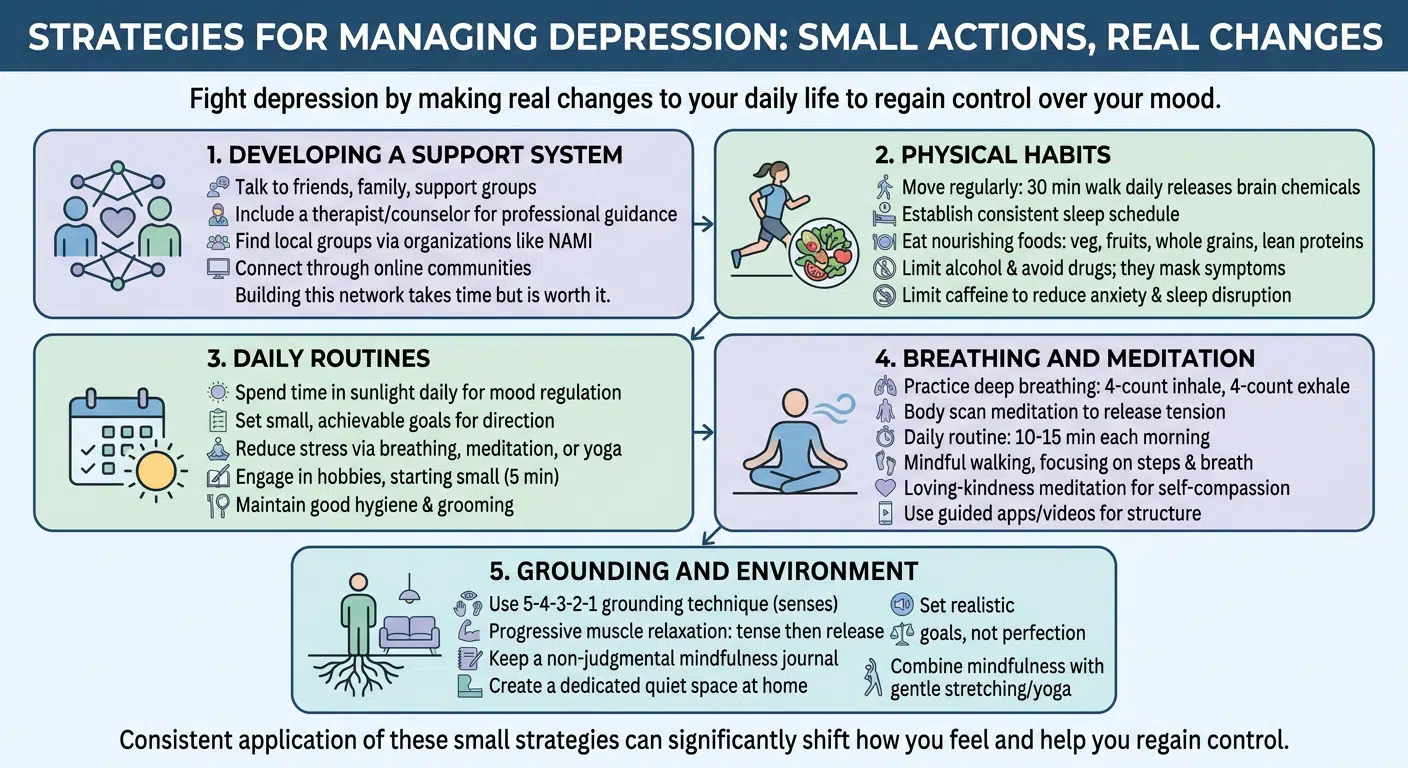
You can fight depression by making real changes to your daily life. Small actions can dramatically shift how you feel and help you regain control over your mood.
Developing a Support System
People who struggle with depression desperately need others around them. Talking to friends, family members, or support groups makes a real difference in your recovery speed.
A therapist or counselor becomes a vital part of your support system, too. They offer professional guidance and tools to help you manage emotional distress safely.
Building this network takes time and effort, but it is entirely worth it. Organizations like the National Alliance on Mental Illness offer free, local support groups across the United States to help you connect.
Online communities and support groups connect you with others facing similar challenges. Your support system becomes stronger as you let more people in and accept their care.
Physical Habits
Lifestyle changes form the backbone of managing depression naturally.
- Move your body regularly. Just 30 minutes of walking a day can significantly reduce symptoms by releasing natural brain chemicals.
- Sleep matters deeply, so establish a consistent bedtime and wake time that your body can count on.
- Eat foods that nourish your brain, focusing on vegetables, fruits, whole grains, and lean proteins.
- Limit alcohol and avoid drugs, since both can mask depression symptoms temporarily but make them stronger over time.
- Limit caffeine intake, which can amplify anxiety and disrupt the sleep patterns that depression already attacks.
Daily Routines
Adding structure to your day gives you a sense of purpose and stability.
- Spend time in sunlight each day, as natural light regulates your mood and energy levels through your brain’s chemistry.
- Build structure into your days by setting small, achievable goals that give you clear direction.
- Reduce stress through breathing exercises, meditation, or yoga to calm your nervous system.
- Engage in hobbies and activities that used to bring you joy, starting small with just five minutes a day.
- Maintain good hygiene and grooming habits, as caring for your appearance sends signals to your brain that you matter.
Breathing and Meditation
Mindfulness practices help calm your mind and build resilience against life’s challenges.
- Practice deep breathing exercises by inhaling slowly for four counts and exhaling for four counts.
- Engage in body scan meditation, mentally moving through each part of your body to release physical tension.
- Start a daily meditation routine for just ten to fifteen minutes each morning to rewire your brain.
- Include mindful walking in your routine by focusing completely on each step and your breath.
- Practice loving-kindness meditation by directing compassion toward yourself to combat self-criticism.
- Explore guided meditation apps or videos that offer structured sessions for anxiety and depression.
Grounding and Environment
Creating a calm environment and staying present are powerful coping mechanisms.
- Use the 5-4-3-2-1 grounding technique when anxiety strikes by identifying things you can see, touch, hear, smell, and taste.
- Try progressive muscle relaxation by tensing each muscle group for five seconds then releasing.
- Keep a mindfulness journal where you write observations without analysis or harsh criticism.
- Create a quiet space in your home dedicated entirely to your mindfulness practice.
- Set realistic goals for your practice rather than expecting perfection every single time.
- Combine mindfulness with gentle stretching or yoga to integrate mind and body awareness.
When to Seek Professional Help for Depression
Knowing when to reach out for professional help can literally change your life. Spotting these signals early helps you get support before things get worse.
Emotional Shifts
Pay close attention to how your feelings change over a two-week period.
- Persistent sadness or emptiness creates a heavy fog that does not lift with time or distraction.
- Loss of interest in activities you once loved signals a major shift in your emotional well-being.
- Irritability or anger outbursts happen much more often, causing tension with people around you.
- Anxiety accompanies depression frequently, creating a worry that compounds your emotional distress.
- Numbness replaces normal emotions, leaving you feeling entirely disconnected from life.
Cognitive Changes
Depression severely impacts how your brain processes information and makes choices.
- Difficulty concentrating or making decisions leaves you stuck and unable to focus on work or school.
- Feelings of worthlessness or guilt consume your thoughts, making you blame yourself for things beyond your control.
- Thoughts of death or suicide demand immediate attention and professional medical care right away.
- Social withdrawal pulls you away from friends and family, as you prefer complete isolation over connection.
- Reckless behavior includes substance abuse or risky activities that put your safety at risk.
Physical Warning Signs
Your body often sounds the alarm before your mind fully realizes what is happening.
- Changes in sleep patterns emerge when you sleep too much or struggle to fall asleep at night.
- Appetite shifts occur as you eat significantly more or less than usual, sometimes without noticing.
- Fatigue and low energy make even simple tasks feel impossible, like climbing a mountain just to get out of bed.
- Physical aches and pains appear without clear medical reasons, affecting your back, head, or joints.
- Neglect of personal hygiene or appearance shows when you stop caring about basic grooming.
Immediate Crisis Lines
Crises demand immediate action, and you need to know exactly where to turn right now.
- The National Suicide Prevention Lifeline operates 24/7 at 988. You can call or text this number for free, confidential support anytime.
- Crisis Text Line lets you text HOME to 741741, connecting you with trained crisis counselors if you prefer not to speak aloud.
- SAMHSA’s National Helpline answers calls at 1-800-662-4357, providing free referrals to local treatment facilities.
- International Association for Suicide Prevention maintains a comprehensive directory of crisis centers worldwide.
- Your local emergency room accepts walk-ins experiencing severe symptoms, offering immediate psychiatric evaluation around the clock.
Community and Medical Support
You can also lean on local resources to catch you before a crisis escalates.
- Mental health crisis teams in your community respond to homes when individuals face acute emotional distress.
- Trusted friends or family members can serve as your first line of support, offering immediate comfort.
- Employee Assistance Programs through your workplace provide confidential counseling sessions at no cost.
- University counseling centers serve students with free therapy sessions and emergency consultations.
- Peer support hotlines staffed by individuals with lived experience offer relatable guidance and practical coping strategies.
The Bottom Line
Depression goes far beyond feeling sad or empty. It is a serious mental health condition that affects how you think, feel, and function in daily life. You might experience emotional distress, physical symptoms, or a heavy numbness that makes everything feel completely gray. The good news is that treatment really does work. Therapy helps, and building a solid support system matters.
Reaching out to a professional, talking to loved ones, or exploring new coping mechanisms can completely shift your path toward recovery and true wellbeing. Your mental health deserves the exact same attention you give to your physical health.
If you are struggling with mood disorders, anxiety, or emotional distress, taking action today creates real change. Self-care practices, simple lifestyle adjustments, and professional help form a powerful combination for healing. You do not have to face this alone, and seeking support shows incredible strength, not weakness.
Understanding depression means recognizing that your pain is real, and your future can absolutely get brighter. Your journey toward resilience and psychological wellness starts with one single step, and that step is yours to take today.
Frequently Asked Questions (FAQs) on Understanding Depression
1. What is depression, and how does it differ from just feeling sad or empty?
Depression is a medical condition where symptoms stick around for at least two weeks (the marker doctors use for diagnosis), draining your energy, messing with sleep and appetite, and stealing joy from things you used to love. It’s not just a bad mood that passes after a rough day; it’s a persistent heaviness that makes even brushing your teeth feel like a marathon.
2. Can someone look happy but still be dealing with depression?
Absolutely, and many call this high-functioning depression. They crack jokes, show up to work on time, and keep up appearances while fighting an invisible battle no one else can see.
3. What are some signs of depression besides sadness?
Watch for major sleep changes (insomnia or sleeping way too much), appetite shifts, trouble focusing on anything, unexplained aches, and pulling away from hobbies or people. The National Institute of Mental Health reports that depression affects about 21 million US adults each year, making these symptoms more common than you might think.
4. How do I help someone who seems lost in their own darkness?
Start by listening without judgment and showing up consistently, even in small ways like sending a quick text or sharing a coffee. Gentle gestures remind them they’re not facing this alone. If things feel heavy, encourage them to reach out to the 988 Suicide & Crisis Lifeline or talk to a doctor, because professional support can truly turn things around.