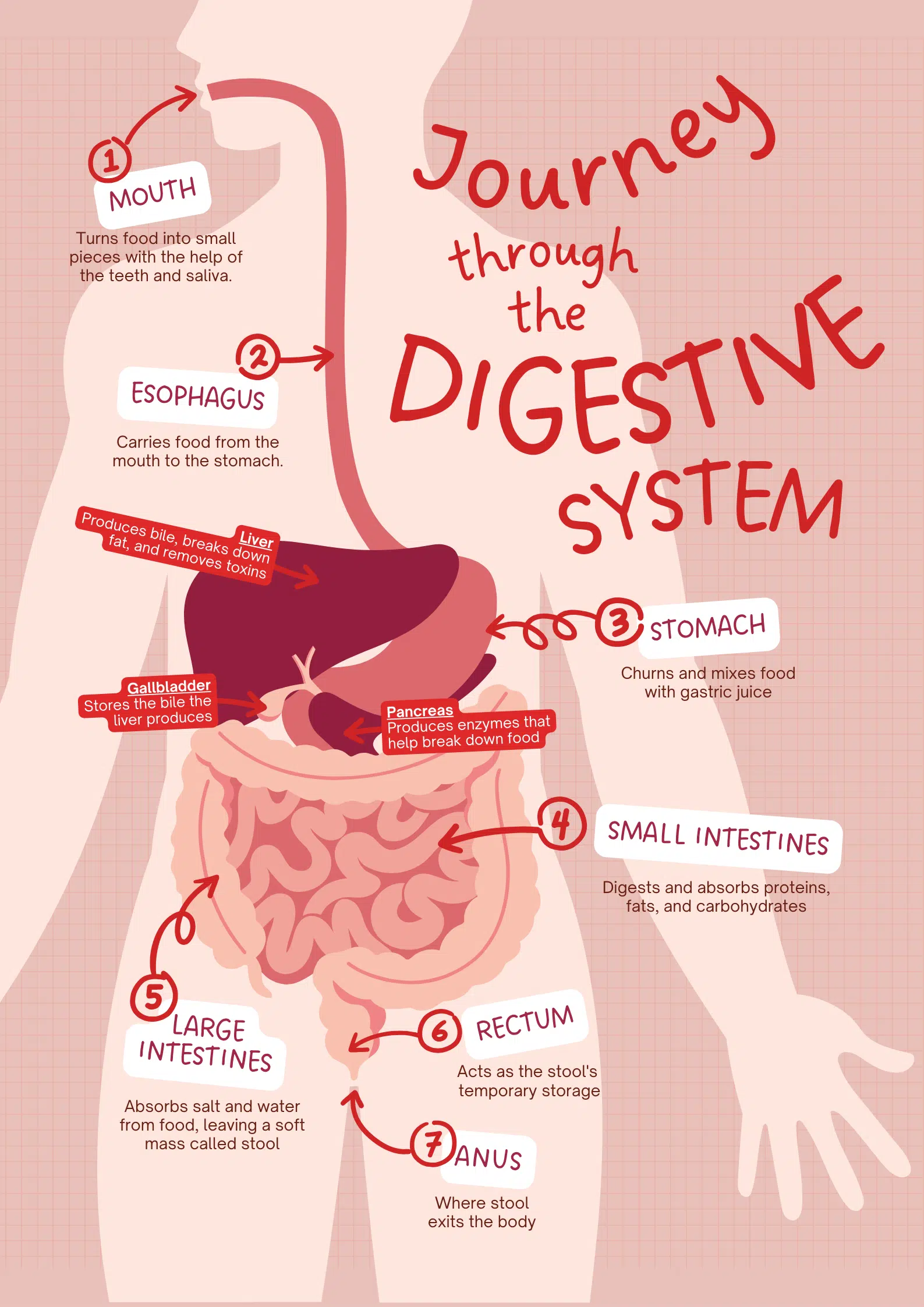
The pancreas is a vital organ that plays an essential role in regulating blood sugar levels and digestion. Unfortunately, many people are unaware of the warning signs that may indicate their pancreas is not functioning optimally. Being attuned to the symptoms of poor pancreatic function can help facilitate early detection and treatment to prevent complications.
This article will overview 30 of the top signs that your pancreas may be functioning poorly. Paying attention to these red flags and consulting your doctor promptly can be critical for supporting pancreatic and overall health.
Content Highlights
- Pay attention to the emergence of multiple symptoms concurrently, like unexplained weight loss combined with repeated vomiting or nausea after eating. Notice correlations between symptoms.
- Do not ignore “red flag” symptoms like greasy, foul-smelling stools, jaundice (yellowing eyes/skin), or unintentional significant weight loss, which warrant immediate further evaluation.
- Schedule routine screenings if at increased risk for pancreatic illness based on family history, pancreatitis, obesity, diabetes diagnosis, or lifestyle factors like smoking and alcohol overuse.
- Communicate with your doctor about risk factors and symptoms because early detection and treatment improve outcomes for pancreatic conditions. Diabetes complications, digestive issues, and deterioration of function can often be prevented with swift action.
- Commit to adopting a preventive lifestyle approach through a healthy diet, regular exercise, stress moderation, and avoidance of smoking and excessive alcohol intake. These factors impact pancreatic function over the long term.
Top 30 Signs Your Pancreas is Functioning Badly
1. Frequent abdominal pain, especially after eating
2. Unexplained weight loss
3. Oily, smelly stools
4. Diabetes or elevated blood sugar
5. Unexplained nausea and vomiting
6. Greasy stool with a particularly bad odor
7. Bloating, abdominal swelling, gas
8. Fever or fatigue
9. Increased thirst and frequent urination
10. Skin rash or itching
11. Confusion or impaired brain function
12. Jaundice (yellowing skin/eyes)
13. Shaking or trembling
14. Difficulty breathing
15. Blood clots
16. Indigestion and heartburn
17. Bulky, frothy stools
18. Dull pain in the back or abdomen
19. Cravings for sweets
20. Vision changes or blurriness
21. Missed menstrual cycles
22. Swelling in legs or feet
23. Weight gain, high BMI
24. Bruising easily
25. Muscle aches or joint pain
26. Anxiety or irritability
27. Acne, oily skin, or patches of skin darkness
28. Bouts of pancreatitis
29. Greasy oil droplets in stool
30. Family history of pancreatic conditions
Analysis of Key Signs
While individual symptoms may indicate various benign conditions, experiencing multiple symptoms concurrently or in combination with risk factors like family history may be a reason for concern about the functioning of the pancreas. For example, while temporary nausea or fatigue occurs commonly and may not signal pancreas issues when appearing alone, pairing vomiting with unexplained weight loss necessitates medical attention to check pancreas health.
Likewise, while stools may occasionally appear oily or foul-smelling after a particular meal, consistent greasy and smelly stools are linked to insufficient pancreatic lipase production needed to digest fats properly. Pancreatic exocrine insufficiency causes food particles to appear in stools, giving them an unpleasant, smelly, oily quality.
Furthermore, while urinating frequently may not intrinsically indicate pancreatic troubles, when combined with increased thirst, confusion, and abdominal pain, pancreatic diabetes becomes more suspected. High blood sugars associated with pancreatic diabetes cause glucose to spill into the urine, pulling fluids from tissues and causing frequent thirst and urination.
In this way, observing correlations between symptoms provides vital insight. Patience also plays a role, as the onset of pancreatic diabetes—a key sign of pancreas dysfunction—can be gradual, accruing symptoms over years. Committing to regular screenings and communicating about risk factors offers the best odds for the early detection and prevention of serious pancreatic disease.
Takeaway
Catching signs of inadequate pancreas function early is crucial for guiding medical intervention to manage diabetes and digestive conditions while preventing deteriorating function or pancreatic cancer. If experiencing multiple symptoms on the list of 30 warning signs, schedule a doctor’s visit for evaluation. Blood tests, MRI scans, and stool samples help diagnose common pancreatic conditions.
Though lifestyle factors like diet, exercise, sleep, and stress levels also influence pancreatic function, promptly treating any underlying condition or dysfunction is key to restoring health. Paying attention to risk factors and warning signs allows patients to partner with providers to safeguard pancreatic health.
Frequently Asked Questions (FAQs)
Check the answers to some commonly asked questions related to pancreas problems.
1. What are 5 of the most serious red flags that something is wrong with my pancreas?
Five of the most concerning potential signs of pancreas dysfunction include:
1) Repeated episodes of severe abdominal pain, especially after eating
2) Unintended weight loss of 10 lbs or more
3) Onset of diabetes or repeated high blood sugar readings
4) Yellowing skin or eyes (jaundice)
5) Greasy, foul-smelling stools or oil droplets in stool
Paying attention to these “red flag” symptoms in combination with risk factors like family history and correlated symptoms warrants promptly scheduling an appointment with your doctor for evaluation.
2. If I notice oily spots and foul smells in multiple stool movements, could that definitely indicate my pancreas is having issues?
Yes, repeatedly observing greasy, smelly stools is a definite red flag for potential problems with the pancreas. Specifically, it likely signals “pancreatic exocrine insufficiency,” meaning your pancreas cannot produce enough digestive enzymes (like lipases) to break down food properly.
Without adequate lipase, fats pass through undigested, causing stool to contain a high percentage of fat, which carries a foul odor and greasy appearance. If this symptom persists, a stool test and evaluation are needed to confirm pancreatic exocrine insufficiency and guide appropriate treatment to help manage symptoms.
3. Does having pancreatitis mean you’ll always have problems with your pancreas later on?
Not always, but a history of pancreatitis does increase risks for chronic pancreatic conditions down the road. The pancreas contains many tiny ducts that can be scarred and damaged during pancreatic inflammation. About 20% of individuals with a bout of acute pancreatitis develop lasting pancreatic damage impacting endocrine and exocrine function.
So, pancreatitis often serves as an early indicator of underlying issues that could impair pancreas function over time when left unaddressed; for those predisposed, lifestyle factors like obesity and alcohol use also compound risks after pancreatitis. Committing to a healthy diet and lifestyle and abstaining from triggering substances can help prevent the recurrence of pancreatitis or the development of secondary pancreatic illnesses.