Do you ever feel like your own mind is playing tricks on you? Maybe negative thoughts keep looping. Your mood suddenly drops, and you feel stuck in exhausting patterns. You want to feel better, but you are probably wondering where to start or if anything will genuinely help. Here is the good news. Cognitive Behavioral Therapy really does work.
In fact, 2025 data shows that it helps about 60 percent of people with anxiety and depression feel significantly better within just a few months. It does not ask you to fake happiness or ignore your real problems. Instead, it gives you practical tools. You learn to catch unhelpful thoughts before they spiral. You can shift your behaviors and build skills that last a lifetime.
I am going to show you exactly how Cognitive Behavioral Therapy (CBT) actually works. We will look at what happens during a session and why this approach is so popular in the United States.
Grab a comfortable seat, and let us go through this together. You will quickly see how your thoughts can become your greatest strength.
What Is Cognitive Behavioral Therapy (CBT)?
Cognitive Behavioral Therapy, or CBT, is a highly effective form of psychotherapy. Dr. Aaron Beck developed this approach in the 1960s at the University of Pennsylvania. It focuses on how your thoughts shape your feelings and actions.
This treatment technique works on a simple idea. The way you think about situations directly influences how you feel and what you do next. If you catch yourself thinking negative thoughts, those thoughts trigger bad emotions. Those emotions then push you toward unhelpful behaviors.
CBT helps you break this vicious cycle. You learn to spot these thought patterns, challenge them, and swap them out for healthier ones. You and your therapist work as a team. Together, you identify the specific thoughts and behaviors that cause you trouble.
The greatest glory in living lies not in never falling, but in rising every time we fall. – Nelson Mandela
CBT stands apart because it is highly practical and goal-focused. This is not just talk-based therapy where you sit and chat about your past for months. Sessions are structured around real problems you face right now.
According to 2025 guidelines from the American Psychological Association, CBT is considered a gold-standard treatment. It works incredibly well for anxiety, depression, obsessive-compulsive disorder, and post-traumatic stress disorder.
The beauty of CBT lies in its directness. Therapists teach you emotional regulation skills and problem-solving techniques that stick with you long after therapy ends. You become your own therapist, spotting cognitive distortions on your own.
Core Principles of CBT
CBT rests on a simple idea. Your thoughts shape how you feel and act. When you change your thinking patterns, your emotions and behaviors shift too.
Identifying negative thought patterns
Negative thought patterns act like clouds that block your mental sunshine. Your brain gets stuck in loops, replaying the same unhelpful stories over and over. These patterns shape how you see yourself, others, and the world around you.
Mental health professionals at the Beck Institute call these “cognitive distortions.” A therapist helps you spot these distorted thoughts before they take control. You learn to notice when your mind jumps to the worst possible outcome.
Some of the most common cognitive distortions in the US include:
- Catastrophizing: Assuming the absolute worst-case scenario will happen.
- All-or-Nothing Thinking: Viewing situations as complete successes or total failures.
- Personalization: Blaming yourself entirely for things outside your control.
- Mind Reading: Believing you know exactly what other people are thinking.
Identifying these patterns takes honest self-reflection and practice. You start paying attention to what your mind says during tough moments. Once you see the pattern clearly, you gain the power to change it.
Understanding the connection between thoughts, emotions, and behaviors
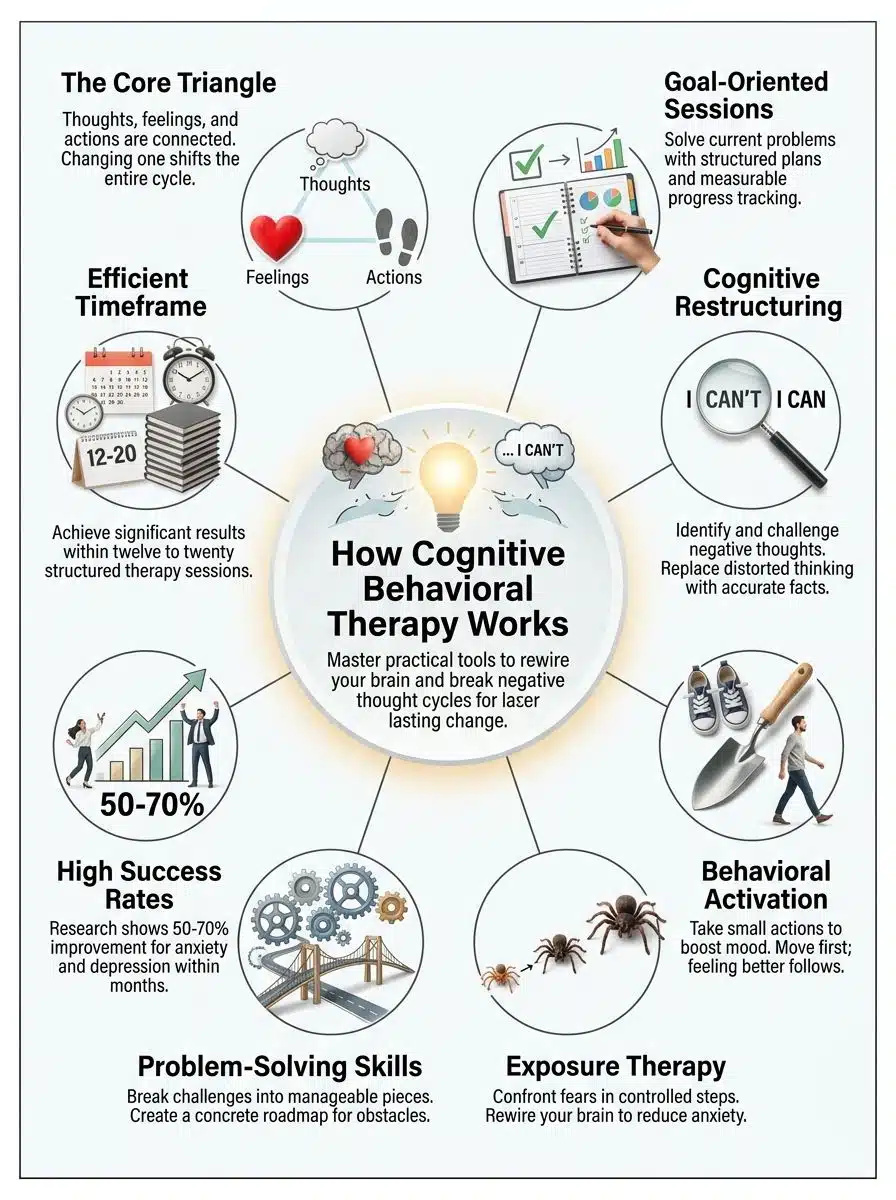
Once you spot those negative thought patterns, the real magic happens. Psychologists refer to this connection as “The CBT Triangle.” Your thoughts, emotions, and behaviors form a connected loop. Changing one side shifts the entire shape.
Think of it like this. Your mind tells you that you will fail a presentation. Your body responds with severe anxiety, and suddenly, you avoid preparing altogether. That avoidance reinforces your original thought, creating a loop that spins tighter and tighter.
CBT breaks this cycle by helping you see how these three elements talk to each other. Your emotions do not just pop up out of nowhere. They follow your thoughts closely. When you think catastrophic thoughts, your body tenses up, your heart races, and you feel scared.
You gain the power to interrupt the pattern by shifting your thinking. This naturally calms your emotions, which then changes your actions. This three-part relationship sits at the heart of behavior modification.
Replacing unhelpful behaviors with constructive actions
Your brain runs on patterns. Some patterns help you thrive, while others trap you in cycles that drain your energy. CBT targets these unhelpful behaviors head-on. You swap them out for actions that actually move you forward.
If you scroll through your phone for three hours when stress hits, your therapist helps you identify this escape route. Then, you build a new, healthier response instead. Recent 2026 mental health data shows that replacing screen time with a simple 15-minute walk significantly boosts mood and focus.
Action precedes motivation. You do not wait to feel better before you move. You move, and feeling better follows.
These constructive actions interrupt the old pattern and create fresh neural pathways. Your therapist does not just tell you what to do. You work together to design solutions that fit your specific life.
Behavioral modification is not about willpower or forcing change overnight. It is about small, intentional shifts that compound over time. Each positive action you take proves to your brain that the old behavior was not serving you.
How CBT Works
You and your therapist work as a team to spot your thought patterns. You challenge them and swap them out for healthier ones that actually stick.
A collaborative approach between the therapist and the individual
CBT therapy works best when you and your therapist team up. You solve the puzzle together. The therapist does not sit back and issue orders. Instead, they work side by side with you to spot the real problems.
US therapists often use a technique called “Socratic Questioning.” Rather than telling you your thoughts are wrong, they ask open-ended questions. This guided discovery helps you examine the evidence and reach your own conclusions.
This collaborative style makes psychotherapy feel less like a doctor visit and more like a trusted friend helping you find your own answers. You build a treatment plan that fits your specific needs. This back-and-forth communication creates trust and keeps you engaged.
Structured and goal-oriented sessions
Therapy sessions work best when they follow a clear roadmap. Structured sessions give you exactly that. Your therapist helps you set specific goals, then builds each session around reaching those targets.
- Session Check-In: You and your therapist review your mood and discuss progress since the last appointment.
- Agenda Setting: You establish a clear outline of specific problems to tackle during that exact session.
- Action-Oriented Work: You actively develop practical solutions and challenge distorted thoughts together.
- Progress Tracking: You measure outcomes to ensure your emotional regulation and coping strategies are actually improving.
- Homework Assignment: You receive specific tasks to practice your new skills in the real world before the next session.
Use of practical tools and strategies
CBT therapists give you real tools that work outside the office. These practical strategies help you tackle mental health challenges in your daily life. They fall into two main categories.
First, your therapist provides cognitive tools to help reframe your negative thoughts:
- Thought Records: You write down triggering situations, automatic negative thoughts, and the resulting emotions to examine them clearly.
- Coping Cards: You carry small notes with helpful statements and strategies to read during high-stress moments.
- Behavioral Experiments: You test whether your worried thoughts match reality by doing the feared action and observing the actual result.
- Problem-Solving Worksheets: You break overwhelming challenges into manageable steps by brainstorming and evaluating solutions.
Second, they offer behavioral tools to change your physical responses and actions:
- Behavioral Activation: You schedule and complete positive activities to naturally lift your mood, even when depressed.
- Exposure Hierarchies: You list scary situations and face them gradually, starting with the easiest challenge.
- Relaxation Techniques: You practice deep breathing or progressive muscle relaxation to calm your nervous system.
- Activity Logs: You track your daily actions to see exactly which habits boost your wellbeing and which ones drain you.
Key Techniques in CBT
CBT therapists use specific methods to help you break free from harmful thought patterns. These practical tools work together to rewire your brain and give you real control over your mental health.
Cognitive restructuring
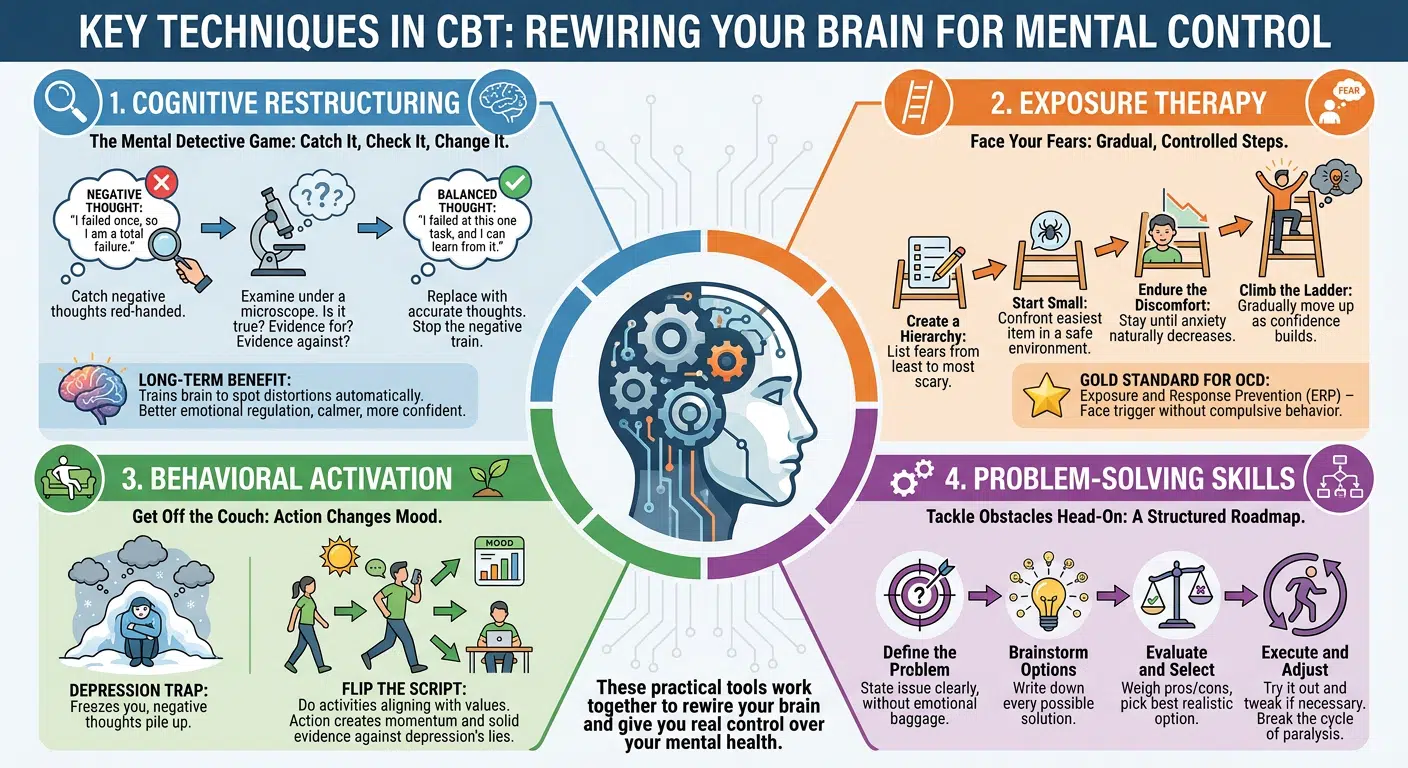
Cognitive restructuring works like a mental detective game. Your therapist helps you catch negative thoughts red-handed. Then, you examine them under a microscope. Many US therapists use a simple three-step method: Catch It, Check It, Change It.
You ask yourself tough questions. Is this thought actually true? What evidence supports it? What evidence contradicts it? You might think, “I failed once, so I am a total failure.” Cognitive restructuring stops that train of thought cold. You replace it with something more accurate, like, “I failed at this one task, and I can learn from it.”
This behavior modification tool sticks around long after therapy ends. You train your brain to spot distorted thoughts automatically. People notice real changes in their emotional regulation within just a few weeks. You start feeling calmer, more confident, and less trapped by your own mind.
Exposure therapy
Exposure therapy puts you face-to-face with the things that scare you. Instead of running away from anxiety triggers, this technique asks you to stay in the situation. Your therapist guides you through gradual, controlled steps.
A specific type of this therapy, called Exposure and Response Prevention (ERP), is considered the gold standard for OCD treatment in the US. You face the trigger without performing the usual compulsive behavior.
Exposure therapy typically follows these specific steps:
- Create a Hierarchy: You list your fears from least scary to most terrifying.
- Start Small: You confront the easiest item on the list in a safe, controlled environment.
- Endure the Discomfort: You stay in the situation until your physical anxiety naturally decreases.
- Climb the Ladder: You gradually move up the list as your confidence builds.
Behavioral activation
Behavioral activation sounds fancy, but it is really just getting you off the couch and back into life. Depression loves to keep you stuck. It freezes you in place while negative thoughts pile up like snow.
This technique flips the script by having you do activities that matter to you. Your therapist helps you pick actions that align with your personal values. This might be taking a walk, calling a friend, or finishing a project.
You start small and build momentum. The magic happens because action changes your mood, not the other way around. You track what you do and how it makes you feel. This creates solid evidence that challenges the lie depression tells you.
Problem-solving skills
As you work through behavioral activation, you will face real problems that need real solutions. Problem-solving skills teach you how to tackle these obstacles head-on instead of avoiding them. Your therapist guides you through a structured process.
Many people stuck in depression or anxiety get paralyzed when problems pop up. They freeze, overthink, or give up before even trying. Problem-solving skills break that cycle by giving you a concrete roadmap to follow.
You can apply this structured approach using these steps:
- Define the Problem: State the exact issue clearly without adding emotional baggage.
- Brainstorm Options: Write down every possible solution, even the silly ones.
- Evaluate and Select: Weigh the pros and cons, then pick the best realistic option.
- Execute and Adjust: Try the solution out in the real world and tweak it if necessary.
Who Can Benefit from CBT?
If you struggle with anxiety, depression, OCD, or PTSD, CBT offers real tools that work. Read on to discover how this therapy can transform your life.
Individuals with anxiety disorders
Anxiety disorders hit hard. Thankfully, CBT offers real relief for people stuck in worry cycles. Your mind gets trapped in loops of fearful thoughts, and your body responds with racing heartbeats, sweating, and tension.
Cognitive behavioral therapy breaks these chains. A 2025 report from the National Institutes of Health indicates a 60 to 70 percent response rate for patients using CBT for anxiety. You learn that most worries never actually happen.
CBT provides several key benefits for anxiety sufferers:
- Fast Relief: It breaks the catastrophic worry cycle quickly.
- Physical Calm: It reduces physical symptoms like tension and racing heartbeats.
- Skill Building: It teaches lifelong coping strategies for future stress.
- Relapse Prevention: It lowers the chance of anxiety returning after therapy ends.
People coping with depression
Depression makes people feel stuck, hopeless, and drained of energy. CBT helps break this cycle by targeting the thought patterns that fuel depression. Your therapist works with you to spot negative thinking, challenge it, and build new mental habits.
You learn that your thoughts shape your feelings, and your feelings shape your actions. By shifting your thoughts, you shift everything else. This approach gives you real tools to fight back against depression, rather than just talking about your problems.
Behavioral activation is a powerful technique for depression. You schedule activities that matter to you, start small, and build momentum. Over time, these actions lift your mood and prove that depression lies to you. Emotional regulation improves as you take action and solve problems.
Those managing obsessive-compulsive disorder (OCD) or PTSD
OCD traps people in cycles of unwanted thoughts and repetitive behaviors that feel impossible to break. Cognitive behavioral therapy works by helping individuals recognize these patterns. They learn to understand what drives the intense anxiety.
For trauma survivors, specific approaches offer immense hope. In the US, Trauma-Focused CBT (TF-CBT) is highly utilized for PTSD. It helps individuals process their experiences and reduce the power those painful memories hold.
Therapists work collaboratively with clients. They teach emotional regulation skills and problem-solving strategies that help them reclaim their lives. Many people find that CBT offers real solutions when other approaches simply have not worked.
Duration and Effectiveness of CBT
Most people finish CBT in 12 to 20 sessions, though some need more time depending on their situation. Research shows that CBT works remarkably well for anxiety, depression, and other mental health challenges.
Typical length of therapy
CBT therapy typically runs between 12 and 20 sessions. This varies based on your specific needs. Your therapist works with you to set clear goals early on, and you track your progress together throughout the treatment process.
Short-term therapy appeals to many people because it fits their schedules and budgets. Under the Affordable Care Act in the US, most health insurance plans are required to cover these essential mental health benefits. You learn practical coping strategies that you can use long after your final session ends.
The time you spend in therapy generally follows these guidelines:
- Mild Symptoms: Often requires only 8 to 12 sessions.
- Moderate Symptoms: Typically takes 12 to 20 sessions.
- Severe Symptoms: May require 6 months or longer of consistent work.
- Maintenance: Occasional check-in sessions are scheduled as needed.
Evidence-based outcomes
Research shows that CBT delivers measurable results for people seeking mental health support. Recent 2025 statistics highlight exactly how effective this approach is across different conditions.
| Condition Treated | Success Rate | Key Finding |
|---|---|---|
| Depression | 50-60% remission rate | Clients see significant improvement within 12-16 sessions. Many experience lasting relief without medication. |
| Anxiety Disorders | 60-70% response rate | Symptoms decrease noticeably after 8-12 weeks. Effects remain stable long after therapy ends. |
| OCD | 65-75% improvement | Exposure and response prevention produce strong outcomes. Intrusive thoughts become less distressing over time. |
| PTSD | 45-55% recovery rate | Trauma-focused CBT reduces nightmares and flashbacks. Clients regain a sense of safety and control. |
| Panic Disorder | 70-80% effectiveness | Panic attacks decrease in frequency and intensity. Many patients become panic-free within several months. |
Studies from the National Institute of Mental Health confirm that CBT outperforms many other treatment approaches. Clients often notice changes within the first few weeks. The improvements stick around, which makes this approach cost-effective long-term.
Insurance companies recognize these strong results and often cover CBT sessions. What is more, research demonstrates that combining CBT with medication boosts outcomes for severe depression. People who complete the full course of therapy report the highest satisfaction rates.
Getting Started with CBT
Finding a qualified therapist matters most. You will want someone trained in CBT methods who fits your needs and personality.
Finding a qualified therapist
A qualified therapist can completely change your mental health journey. Your search for the right professional requires a few specific steps.
- Check Credentials: Verify they hold valid state licenses and have specific training in cognitive behavioral therapy.
- Ask About Experience: Ensure they have successfully treated your specific condition, like anxiety or OCD.
- Verify Insurance: Confirm they accept your US health insurance plan to keep out-of-pocket costs low.
- Read Client Reviews: Look at online feedback from past clients to understand the therapist’s personal style.
- Schedule a Consultation: Book a brief phone call to see if you click with them before committing to a session.
Preparing for your first session
Your first therapy session sets the tone for your entire treatment journey. Getting ready helps you make the most of your time with your therapist.
- Gather History: Compile your mental health history, past diagnoses, and current medications.
- List Symptoms: Write down your main concerns and specific triggers so you do not forget them during the appointment.
- Set Goals: Define two or three specific goals you want to achieve, like reducing panic attacks or sleeping better.
- Bring Paperwork: Have your insurance card, payment details, and ID ready for the front desk.
- Prepare Questions: Write down questions about their specific treatment techniques and homework expectations.
The Closing Thoughts
Cognitive behavioral therapy opens doors to real change for millions of people each year. This treatment approach gives you practical tools to reshape how you think, feel, and act. You gain control over thought patterns that once held you back. You develop coping strategies that stick with you long after therapy ends. The power lies in your hands, not in waiting for someone else to fix things.
Therapy outcomes show that people who engage fully in this process see lasting results. This is especially true when they practice what they learn between sessions.
Starting your mental health journey takes courage. However, understanding exactly how Cognitive Behavioral Therapy (CBT) actually works makes the path clearer. The collaborative relationship you build with your therapist creates a safe space to tackle anxiety and depression head-on.
Behavioral modification happens gradually, step by step. You challenge cognitive distortions and replace unhelpful behaviors with constructive ones. This is not magic, but it works because it is based on how your brain actually functions. Take that first step today. Find a qualified therapist, and discover what real emotional regulation can do for your life.
Frequently Asked Questions (FAQs) on Cognitive Behavioral Therapy
1. What is Cognitive Behavioral Therapy, and how does it actually work?
CBT helps you notice negative thoughts and swap them for healthier ones, which changes how you feel and behave. A therapist guides you through practical exercises, and research from the Beck Institute shows most people learn the core skills within 12 to 16 sessions.
2. Can CBT help with anxiety or sadness?
Yes, CBT works really well for both anxiety and depression. Studies show that around 60% of people see significant improvement after completing a full CBT program.
3. How long does it take for CBT to show results?
Many people notice positive changes within 4 to 6 weeks of weekly sessions. The more you practice the techniques between appointments, the faster those new thinking patterns become automatic.
4. Do I have to talk about my childhood during CBT sessions?
Not usually. CBT focuses on your current thoughts and what you want your life to look like going forward, rather than exploring your past in depth. Your therapist might touch on relevant memories if they connect to patterns you’re working on now, but that’s not where most of the work happens.


![Cognitive Behavioral Therapy [CBT]](https://cdn1.editorialge.com/wp-content/uploads/2026/05/Cognitive-Behavioral-Therapy-CBT-.jpg.webp)