GAs of early 2026, Ireland’s Health Service Executive (HSE) is navigating a period of unprecedented structural change. While the 2026 National Service Plan has allocated a record €29 billion budget to the sector, the frontline reality remains defined by a persistent staffing gap that threatens service delivery. This crisis is no longer just a matter of graduation numbers; it is a complex intersection of global competition for talent, domestic cost-of-living pressures, and an aging demographic that requires more intensive care than the system was originally designed to provide.
How We Selected Our 7 Best Ireland Healthcare Staffing Crisis Insights
To provide an accurate assessment of the healthcare landscape in 2026, we analyzed several key data points from the first quarter of the year. Our selection process was guided by recent legislative changes, the 2026 Pay and Numbers Strategy (PNS), and frontline reports from major Irish medical organizations.
-
HSE National Service Plan 2026: We reviewed the specific Whole Time Equivalent (WTE) targets and the €29bn investment priorities.
-
Economic Indicators: We factored in the impact of the €14.15 per hour minimum wage and the 2.25% annual public service pay increase.
-
Migration Trends: We cross-referenced the registration data for Irish medics in Australia and the 12-16 week processing times for international recruits.
-
Operational Metrics: We analyzed the performance of the newly established six Health Regions under the Sláintecare reform.
The following data points illustrate the current pressures and targets within the 2026 staffing ecosystem.
| Metric Evaluated | 2026 Status / Target | Impact Level |
|---|---|---|
| HSE Net Staff Growth | +1,050 WTE (Target) | Moderate |
| Total Health Budget | €29 Billion | High |
| NMBI Registration Time | 12–16 Weeks (Average) | Moderate |
| Aged 65+ Population | 15% of total (Driving demand) | Critical |
The 7 Core Reasons for the Ireland Healthcare Staffing Crisis 2026
Understanding the root causes of the vacancy rates in 2026 is essential for identifying which government interventions are working and which are falling short.
1. The “Australia Lure” and Competitive Emigration
As of 2026, the migration of Irish doctors and nurses to Australia remains a primary concern for the HSE. Australian health boards continue to offer aggressive recruitment packages, including relocation bonuses and significantly higher starting salaries than the Irish public system. For many young Irish graduates, the promise of better work-life balance and sunnier climates outweighs the current domestic public service pay agreements.
Best for: Newly qualified doctors and nurses seeking high-income potential and improved workplace culture abroad.
Why We Chose It:
-
It is the leading cause of “brain drain” among the 21,000 registered doctors in Ireland.
-
It highlights the ongoing struggle to make the Irish public sector competitive on a global scale.
-
It directly impacts the “pipeline” of future consultants and specialists within the HSE.
Things to consider: While the 2.25% annual pay increase helps, it often struggles to keep pace with the lifestyle incentives offered in the Southern Hemisphere.
2. Housing Affordability and “Key Worker” Displacement
High housing costs in urban centers like Dublin, Cork, and Galway are preventing healthcare staff from living near their places of work. In 2026, the vacancy rates for nurses and healthcare assistants (HCAs) are highest in areas where the rent-to-income ratio is most skewed. This has led to a “displacement” effect where staff either leave the profession or move to more affordable rural regions, leaving major teaching hospitals understaffed.
Best for: Understanding why major metropolitan hospitals face higher vacancy rates than smaller regional facilities.
Why We Chose It:
-
It is cited by healthcare unions as the number one barrier to staff retention in 2026.
-
It undermines the Sláintecare goal of providing “community-based care” in high-demand urban zones.
-
It forces many frontline workers into long commutes, which contributes to burnout and attrition.
Things to consider: The 2026 budget for disability and older person services includes home support hours, but these are difficult to fill without local, affordable housing.
3. The Complexity Gap of an Aging Population
With over 15% of the Irish population now aged 65 or older, the complexity of care required in 2026 has surged. Patients now present with more chronic conditions and multi-morbidities, requiring more staff-hours per patient than a decade ago. This “complexity gap” means that even when staff numbers remain stable or grow slightly, the perceived workload on the ward feels significantly heavier.
Best for: Long-term healthcare planners trying to align workforce numbers with actual patient needs.
Why We Chose It:
-
It explains why a 3% growth in nurse numbers (to 92,385) still feels insufficient on the frontline.
-
It drives the need for specialized roles like Advanced Nurse Practitioners and Geriatric Specialists.
-
It places immense pressure on the 26.7 million hours of home support targeted for 2026.
Things to consider: As the population continues to age, the demand for healthcare staff will likely outstrip supply for the remainder of the decade.
4. Registration and Accreditation Bottlenecks
Ireland relies heavily on international recruitment to fill immediate gaps, yet the 2026 registration process remains slow. The Nursing and Midwifery Board of Ireland (NMBI) currently averages 12 to 16 weeks to process international applications. For a system in crisis, these three-to-four-month delays mean that qualified staff are often stuck in administrative limbo while wards remain short-staffed.
Best for: International healthcare professionals planning a move to Ireland in 2026 or 2027.
Why We Chose It:
-
It is a fixable “bureaucratic hurdle” that significantly hampers rapid recruitment efforts.
-
It often leads to candidates choosing other countries (like the UK or Canada) with faster processing times.
-
It creates a backlog for the 12 nursing specialties currently seeing active hiring.
Things to consider: The 2026 National Service Plan aims to streamline these processes, but improvements are still in the early implementation phase.
5. Public vs. Private Sector Pay Divergence
The pay gap between the public and private healthcare sectors has widened to approximately 15–20% for many frontline roles in 2026. While the HSE offers excellent job security and pensions, private hospitals and nursing homes are increasingly attracting staff with better rosters, sign-on bonuses, and higher immediate hourly rates. This internal competition makes it difficult for the HSE to maintain a stable workforce.
Best for: Healthcare professionals prioritizing immediate take-home pay and flexible scheduling over long-term public pensions.
Why We Chose It:
-
It drives the reliance on expensive “agency staff,” which the HSE is trying to reduce through its 2026 conversion strategy.
-
It creates a “hiring war” for experienced surgical and theatre nurses in major cities.
-
It forces the public sector to continuously innovate its recruitment campaigns to stay relevant.
Things to consider: The 2026 minimum wage increase to €14.15 has also pushed up costs for private providers, narrowing their ability to offer massive bonuses.
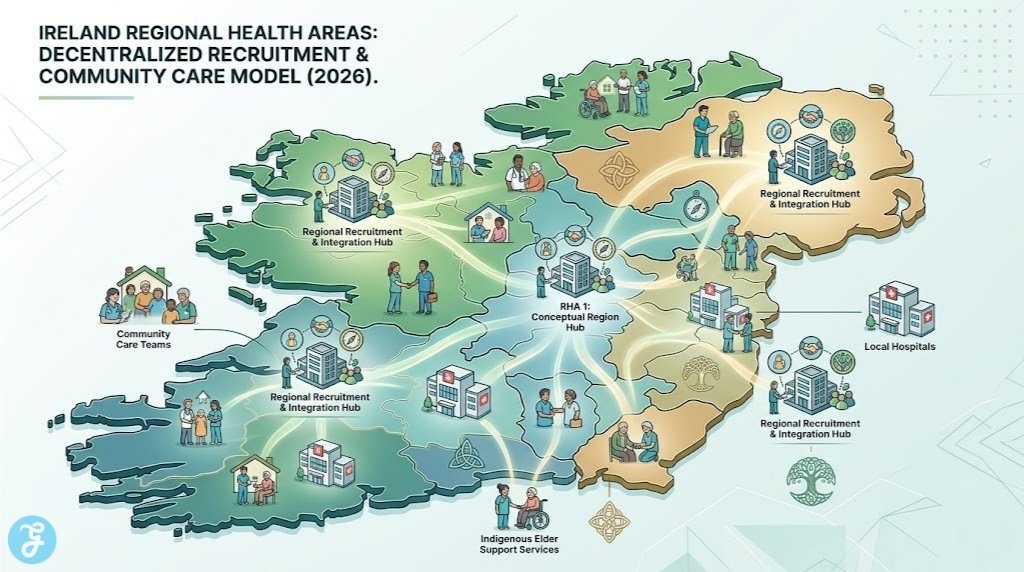
6. Transition to Regional Health Areas (RHAs)
The 2026 establishment of six new HSE Health Regions under Sláintecare is a massive organizational shift. While this move toward “integrated care” is designed to be more efficient, the transition phase has created temporary recruitment bottlenecks. Local regions are still finding their feet in terms of autonomous hiring, leading to inconsistencies in how vacancies are filled across the country.
Best for: Staff looking for roles in “integrated care” settings closer to their local communities.
Why We Chose It:
-
It represents the most significant structural reform in the history of the Irish health service.
-
It aims to plan and deliver services around the specific needs of local populations.
-
It empowers local managers but requires a settling-in period for the new 20 Integrated Health Areas.
Things to consider: 2026 is considered the “first major step” toward this decentralized model of resource allocation.
7. Frontline Burnout and the Retention Vicious Cycle
High vacancy rates in 2026 naturally lead to increased pressure on the staff who remain. This creates a “vicious cycle” of burnout: short-staffing leads to stress, stress leads to resignation, and resignation further increases the short-staffing. Despite the lifting of the recruitment freeze, many staff report that the pace of work in 2026 is becoming unsustainable without a massive influx of new colleagues.
Best for: Understanding the psychological and operational impact of long-term staffing shortages on the existing workforce.
Why We Chose It:
-
It is the primary reason why experienced mid-career professionals leave the public service.
-
It impacts patient flow and waiting times for both emergency and scheduled care.
-
It necessitates the “Retention and Recruitment” initiatives highlighted in the 2026 National Service Plan.
Things to consider: Employers who prioritize “flexibility, culture, and retention” are currently seeing the best results in the 2026 market.
An Overview Of Ireland Healthcare Staffing Crisis
The current crisis is being addressed through a combination of record-breaking investment and structural decentralization.
Overview Comparison Table
The following comparison illustrates how different sectors of the Irish healthcare workforce are being targeted for growth and reform in 2026.
| Staff Category | 2026 Focus Area | Primary Incentive |
|---|---|---|
| Doctors | Public-Only Consultant Contract | High Salary & Research Time |
| Nurses | Community & Disability Care | 2.25% Pay Rise & Sponsorships |
| Mental Health | +300 New Clinical Posts | Specialized Crisis Response Roles |
| International | Faster Onboarding | Adaptation Programs & Relocation |
Our Top 3 Picks and Why?
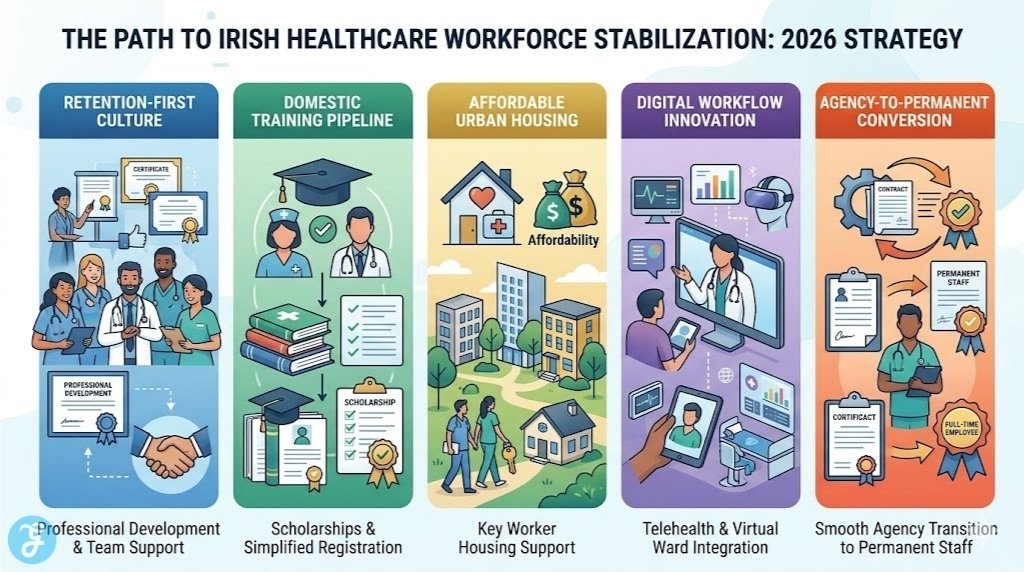
Of all the strategies currently in play, the Regional Health Areas (RHAs), the Pay and Numbers Strategy (PNS), and Digital Health Solutions are the most critical. The RHAs provide the localized structure needed for integrated care, the PNS provides a clear target for converting high-cost agency roles into permanent WTE positions, and Digital Health (such as virtual wards) allows the existing workforce to manage demand more efficiently through technology.
How to Choose the Right Ireland Healthcare Staffing Crisis Strategy by Yourself?
Navigating a career or a business within the Irish healthcare sector in 2026 requires a proactive understanding of where the growth is happening.
The Selection Framework:
-
Verify Regional Demand: Check the six new HSE Health Regions to see which areas (like Dublin, Cork, or Galway) have the highest concentration of your specialty.
-
Assess Pay vs. Benefits: Compare the 2026 HSE pay scales against private sector “sign-on” bonuses to determine your long-term financial goals.
-
Look for Sponsorships: If you are in nursing, investigate the Public Health Nurse Sponsorship Programme for 2026/27 to get postgraduate training funded.
-
Monitor the Agency Cap: If you are an agency worker, be aware that the HSE is actively trying to convert these roles into permanent positions with different benefit structures.
Decision Matrix:
This matrix helps healthcare professionals decide on their next move based on the 2026 market conditions.
| If your priority is… | Then you should choose… |
|---|---|
| Maximum Flexibility | Agency or Bank work in urban hotspots. |
| Specialized Training | Public Sector roles with postgraduate sponsorships. |
| Work-Life Balance | Community care or “Step-down” facility roles. |
The Final Checklist
-
Have you checked your eligibility for the 2.25% annual salary increase or the €1,125 minimum uplift?
-
Is your NMBI or Medical Council registration current and linked to the correct 2026 pay grade?
-
Have you explored the 5 new surgical hubs for potential specialist openings?
-
Are you registered for MyMedicare or equivalent digital staff portals for real-time RHA updates?
-
Have you reviewed the HSE National Service Plan 2026 for your specific department’s WTE ceiling?
Navigating Toward a Resilient Irish Health Service
The Ireland healthcare staffing crisis of 2026 is a significant hurdle, but the “foundations of organizational reform” are now firmly in place. By shifting to six Regional Health Areas and committing to a record €29 billion investment, the state is attempting to build a more sustainable and responsive system. The success of these reforms will ultimately hinge on the ability of the HSE to close the “Australia gap” and make Ireland an attractive, affordable place for medical professionals to build a lifelong career. As we move deeper into 2026, the focus remains clear: use every resource, existing and new, to deliver the right care in the right place at the right time.