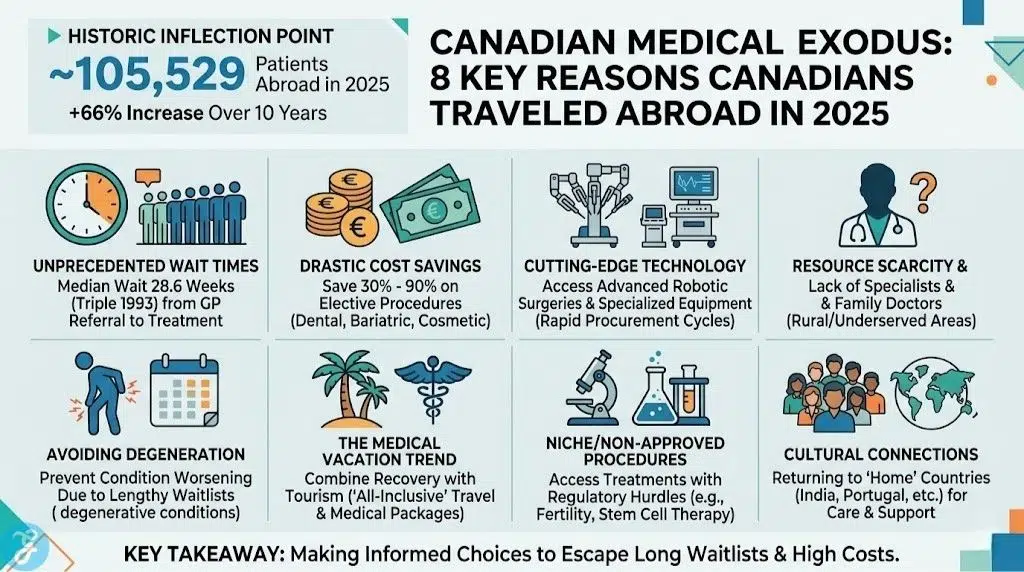
The landscape of Canadian healthcare reached a historic inflection point in 2025. As provincial systems grappled with an aging population and chronic workforce shortages, the number of Canadians seeking medical treatment abroad 2025 surged to an estimated 105,529 patients. This represents a staggering 66% increase over the last decade, signaling a fundamental shift in how residents view their “universal” coverage. For many, the choice to leave the country was not a luxury but a desperate maneuver to escape a system defined by record-breaking queues and deteriorating quality of life.
This guide examines the eight primary drivers that fueled this unprecedented medical migration last year.
Our Selection Methodology
To compile this 2025 retrospective, we analyzed the latest Fraser Institute “Leaving Canada for Medical Care” 2025 report, wait-time data from the Canadian Institute for Health Information (CIHI), and global medical tourism cost indices. We prioritized reasons that directly correlate with the 2025 median wait time of 28.6 weeks—the second-longest in history. Our selection highlights the specific specialties most affected, such as urology and general surgery, while incorporating real-world cost comparisons from emerging medical hubs like Turkey, Mexico, and India.
8 Reasons Canadians Traveled Abroad for Care in 2025
From fiscal necessity to physical survival, the motivations for seeking international care are increasingly diverse.
1. Historical Peaks in Surgical Wait Times
In 2025, the national median wait time from GP referral to actual treatment hit 28.6 weeks, triple the wait recorded in 1993.
-
Best for: Patients in “High-Wait” provinces like New Brunswick and British Columbia.
-
Why We Chose It: This is the undisputed primary driver; for over 1.4 million Canadians, “waiting your turn” has become a months-long period of medical limbo.
-
Things to consider: These waits include a 15.3-week delay just to see a specialist, meaning the clock often starts long before a surgery is even booked.
2. Drastic Cost Savings on Elective Procedures
While medically necessary care is “free” in Canada, many residents opted to pay out-of-pocket abroad to save on procedures with high local private costs, such as dental implants or bariatric surgery.
-
Best for: Individuals requiring comprehensive dental work or cosmetic enhancements not covered by provincial plans.
-
Why We Chose It: Canadians can save between 30% and 90% by traveling to destinations like Mexico or Costa Rica.
-
Things to consider: A hip replacement costing $40,000 in a private US clinic can be as low as $6,000 in India, making global options financially life-changing.
3. Access to Cutting-Edge Medical Technology
Many Canadians seeking medical treatment abroad 2025 did so to access advanced robotic surgeries or specialized diagnostic equipment not yet widely available in their home province.
-
Best for: Patients seeking minimally invasive oncological or neurological procedures.
-
Why We Chose It: Private clinics in Germany and Thailand often invest in the latest technology faster than the public Canadian system can navigate procurement cycles.
-
Things to consider: Seeking “advanced” care abroad requires careful verification of international accreditation, such as JCI (Joint Commission International) standards.
4. Resource Scarcity and “Dental Deserts”
The 2025 healthcare crisis was exacerbated by a lack of specialists, with over 6.5 million Canadians living without a regular family doctor.
-
Best for: Residents in rural or underserved urban areas where specialist lists are permanently closed.
-
Why We Chose It: When local referrals are impossible to obtain, international hubs provide an immediate “open-door” policy for self-funded patients.
-
Things to consider: Urology saw the highest percentage of patients going abroad (3.7%) due to specific equipment and specialist shortages in Canada.
5. Avoiding “Deterioration on the List”
Wait times in 2025 were linked to increased pain, suffering, and in the most tragic cases, death. Over 23,000 patients died while on a Canadian surgical or diagnostic waiting list last year.
-
Best for: Patients with degenerative conditions where every week of delay leads to permanent mobility loss.
-
Why We Chose It: Traveling abroad is often a preemptive strike against a worsening condition that the Canadian system cannot address fast enough.
-
Things to consider: The “hidden cost” of waiting is estimated at over $3,000 per patient in lost wages and productivity.
6. The Rise of the “Medical Vacation” Trend
Combining recovery with tourism became a significant sub-sector of the 2025 travel industry.
-
Best for: Patients undergoing low-risk procedures who can benefit from a peaceful recovery environment.
-
Why We Chose It: Destinations like Turkey and Thailand offer “all-inclusive” medical packages that include luxury hotel stays, translation services, and post-op care.
-
Things to consider: Tourism is generally encouraged only before the procedure or after an initial recovery period to minimize the risk of blood clots during flights.
7. Seeking Non-Approved or Niche Procedures
Certain specialized treatments, particularly in fertility and stem cell therapy, face regulatory hurdles in Canada that are absent in other jurisdictions.
-
Best for: Couples seeking specific IVF protocols or patients interested in emerging regenerative therapies.
-
Why We Chose It: It provides a pathway for those whose medical needs fall outside the standardized “one-size-fits-all” public coverage.
-
Things to consider: Post-operative follow-up care can be difficult in Canada if domestic doctors are unfamiliar with the specific overseas procedure.
8. Cultural and Linguistic Connections
A significant portion of medical travelers in 2025 were second- or third-generation immigrants returning to their “home” countries for care.
-
Best for: Indo-Canadians and those with family ties in Europe or Asia.
-
Why We Chose It: Combining a family visit with high-quality, affordable care in places like India or Portugal reduces the “stranger anxiety” of foreign hospitals.
-
Things to consider: Having a local support system can significantly improve recovery outcomes and ease the logistical burden of travel.
2025 Global Healthcare Cost Comparison
To understand the economic incentive, we compared the average 2025 out-of-pocket costs for common procedures across popular medical tourism destinations.
| Procedure Type | Canada (Private/Out-of-Pocket) | Mexico / Turkey | India / Thailand |
| Hip Replacement | $25,000 – $35,000 | $12,000 | $7,000 |
| Knee Replacement | $22,000 – $30,000 | $11,000 | $6,500 |
| Dental Implants (Full Mouth) | $35,000+ | $12,000 | $8,000 |
| IVF Cycle | $15,000+ | $7,500 | $5,000 |
Note: Canadian costs are estimates based on private surgical centers; public care remains $0 but with significant wait times.
Refining the 2025 Medical Exit Strategy
The phenomenon of Canadians seeking medical treatment abroad 2025 is the clearest indicator of a system struggling to fulfill its mandate. While the Canadian model excels in acute, life-saving emergency care, the “waiting list” for quality-of-life procedures has reached a breaking point. For over 105,000 residents last year, the decision to leave was a rational response to an irrational wait. As we look toward the future of Canadian health policy, these patients serve as a living testament to the need for structural reform—or, at the very least, a robust “Plan B” for those who simply cannot afford to wait any longer.
FAQs
Is medical tourism safe?
Yes, provided you choose hospitals with JCI or similar international accreditation and verify the surgeon’s credentials.
Will my provincial insurance reimburse me?
Rarely. Most provinces only reimburse out-of-country care if it was pre-approved due to a total lack of that specific service in Canada.
What are the biggest risks?
The primary risks are post-surgical complications (like DVT) during long-haul flights and the lack of integrated follow-up care once you return home.