As we navigate through 2026, the British dental system is no longer just “under pressure”—it has fundamentally fractured. While government headlines focus on the 2024 recovery plan’s legacy, the ground reality for millions is a stark landscape of “dental deserts” and the rise of high-risk self-treatment. Understanding the structural shifts in how dentists are paid and why geographic location now determines your oral health is essential for survival in this new era. This guide uncovers the UK dentistry crisis 2026 nuances that explain why a simple check-up has become one of the UK’s most elusive services.
Our Selection Methodology
To compile this 2026 crisis report, we analyzed the latest March 2026 Healthwatch findings, the April 2026 NHS Dental Contract reforms, and the General Dental Council (GDC) workforce patterns. We prioritized data that goes beyond “long waits,” focusing on the “poverty penalty” and the specific legislative changes—such as the 76% increase in urgent care tariffs—that are reshaping practice priorities this year. Our selection highlights the systemic health links and the specific regional statistics that define the current state of British oral healthcare.
7 Things Most People Don’t Know About the UK Dentistry Crisis 2026
The crisis in 2026 is defined by a shift from public provision to a “two-tier” system where wealth dictates health.
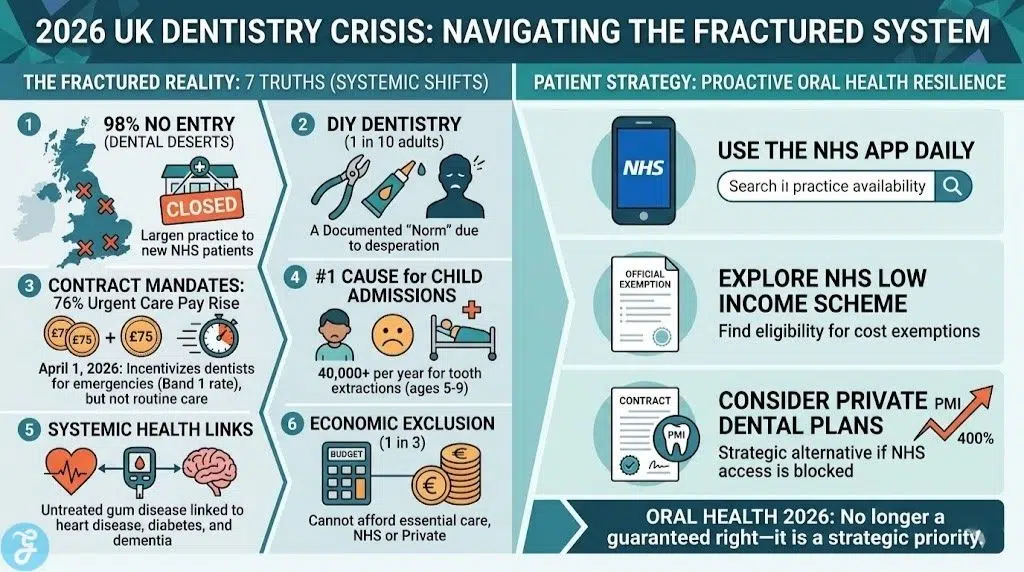
1. The 98% “No Entry” Rule in Dental Deserts
In 2026, “dental deserts” have expanded significantly, with 98% of practices in regions like the South West, North West, and Yorkshire refusing new NHS adult patients.
-
Best for: Residents in isolated or high-deprivation communities looking for care.
-
Why We Chose It: This statistic illustrates that for nearly an entire region, the NHS dental “safety net” has effectively ceased to exist for newcomers.
-
Things to consider: Many practices in these red zones have also closed their waiting lists entirely, meaning “waiting” is no longer an option.
2. DIY Dentistry is Now a Documented “Norm”
Resorting to self-treatment, such as using superglue for lost crowns or extracting one’s own teeth, is no longer an urban legend; it is a reported reality for 1 in 10 UK adults in 2026.
-
Best for: Public health advocates and policymakers tracking the human cost of the crisis.
-
Why We Chose It: It highlights the desperate measures patients are taking when they find themselves in the “revolving door” of untreated urgent pain.
-
Things to consider: DIY dentistry often leads to severe infections that eventually require emergency hospital admission, placing further strain on the wider NHS.
3. The 2026 Contract Mandates a 76% “Urgent Care” Pay Rise
Starting April 1, 2026, the way dentists are paid for urgent work has changed drastically, with payments for unscheduled care rising by 76% to a national rate of £75.
-
Best for: Practice owners and associates managing their NHS commitment.
-
Why We Chose It: This is the most significant contract reform in twenty years, designed to incentivize dentists to keep slots open for emergencies.
-
Things to consider: While better for urgent cases, this reform does not necessarily improve access for routine check-ups or preventative care.
4. The “Poverty Penalty” Has Doubled Private Care Use
New data shows that the number of “financially struggling” households using private dentistry has almost doubled since 2023, rising from 14%
-
Best for: Families on low incomes who are trying to balance essential healthcare with the cost-of
-
Why We Chose It: It proves that even those who cannot afford it are being forced into the private sector simply to stop the pain.
-
Things to consider: Low-income patients who go private lose their NHS charge exemptions, effectively paying a “double penalty” for the system’s failure.
5. Extractions are the #1 Cause of Child Hospital Admissions
Tooth extraction remains the leading reason for hospital admissions among children aged 5 to 9 in the UK, a figure that has remained tragically high in 2026.
-
Best for: Parents and educators focusing on early-years oral health.
-
Why We Chose It: It serves as a stark reminder that the dentistry crisis has long-term physical consequences for the next generation.
-
Things to consider: Over 40,000 children per year still require general anesthesia for these procedures, which are almost entirely preventable.
6. The “Systemic” Link: Oral Health and 2026 Dementia Research
2026 clinical guidelines have reinforced the link between untreated gum disease and systemic illnesses like heart disease, diabetes, and even early-onset dementia.
-
Best for: Health-conscious individuals managing long-term chronic conditions.
-
Why We Chose It: This underscores that the dental crisis isn’t just about teeth; it’s a “gateway” to a lifetime of cascading health failures.
-
Things to consider: Improving oral hygiene can reduce the inflammatory markers that contribute to these broader systemic risks.
7. One in Three Britons Now Find Essential Care Unaffordable
As of March 2026, a staggering 33% of the UK population reports being unable to afford essential dental care, whether on the NHS or privately.
-
Best for: Economic analysts and citizens planning their household budgets.
-
Why We Chose It: It highlights that the crisis has moved beyond “access” and into the realm of basic economic exclusion.
-
Things to consider: Private Medical Insurance (PMI) with dental add-ons is seeing a 400% surge in interest as a result of this affordability gap.
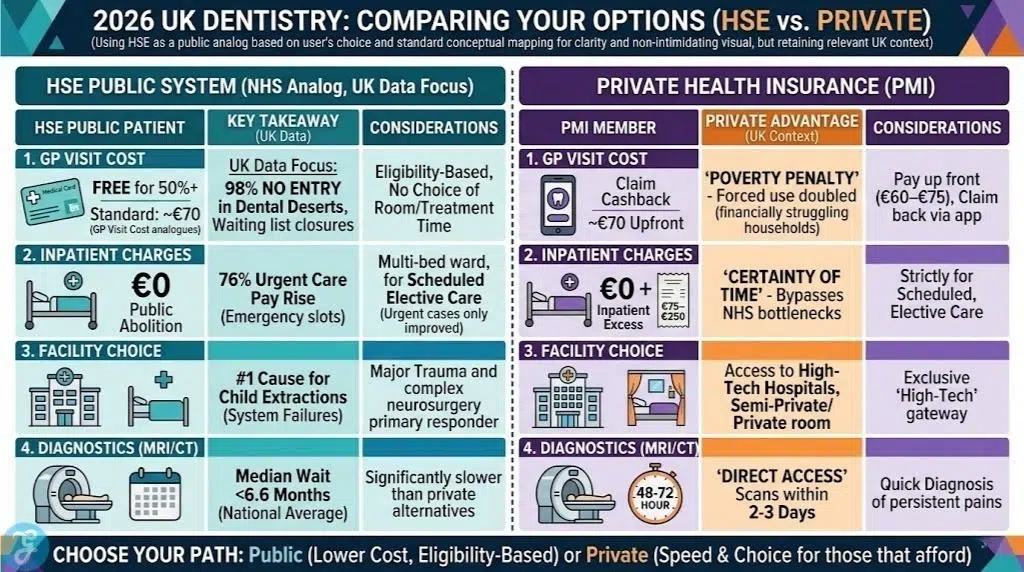
2026 Cost Comparison: NHS vs. Private Realities
Navigating the financial side of the crisis requires a clear understanding of what you are paying for. The table below compares the standard 2026 NHS charges against the average private fees currently seen in the UK.
| Treatment Type | NHS Charge (Band 1/2/3) | Average Private Fee (2026) |
| Routine Examination | £27.40 (Band 1) | £50 – £85 |
| Fillings / Extractions | £73.50 (Band 2) | £120 – £250 |
| Crowns / Dentures | £319.10 (Band 3) | £600 – £1,200+ |
| Urgent Care | £27.40 (Band 1) | £75 – £150 (Emerg. Fee) |
Note: NHS charges are fixed nationally, while private fees vary significantly by region and practice.
The Road to Oral Health Resilience
The UK dentistry crisis 2026 is a complex interplay of outdated contracts, geographic inequality, and economic pressure. While the April 2026 reforms offer a glimmer of hope for urgent care, the “prevention-first” model remains a distant goal for most. To navigate this, patients must be proactive: utilizing the NHS App to track practice availability daily, exploring the NHS Low Income Scheme for cost exemptions, and considering the long-term savings of private dental plans if NHS access remains blocked. In 2026, oral health is no longer a guaranteed right—it is a strategic priority that requires active management and informed decision-making.