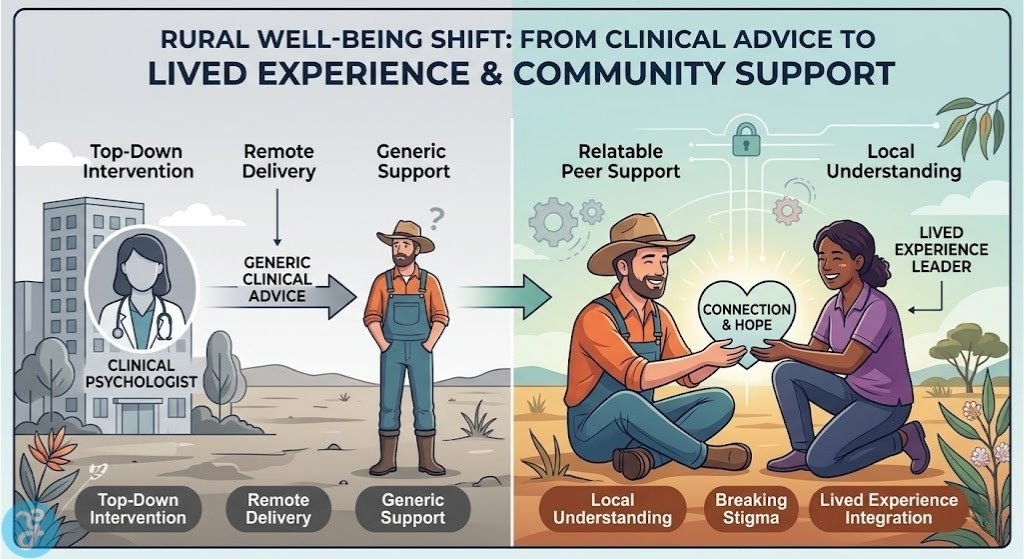
The emotional toll of loss in rural landscapes often feels more profound due to the tight-knit nature of small towns where every person is known by name. As we navigate 2026, the data indicates that Australians living outside capital cities continue to face significantly higher rates of distress compared to their urban counterparts. Addressing this gap requires more than just clinical intervention. It demands a robust commitment to Community Suicide Prevention Australia through local empowerment and specialized support systems.
This guide explores nine practical ways to strengthen the social fabric and protective factors in regional and rural settings.
How We Selected Our 9 Best Rural Suicide Prevention Tips for 2026
To provide actionable and evidence-based guidance for the current year, we examined the 2025 and 2026 reports from the National Suicide Prevention Office and the latest Community Tracker data. Our selection process focused on strategies that prioritize “lived experience” and grassroots involvement rather than top-down clinical models. We specifically looked for programs that have shown measurable success in remote environments where traditional health services are limited.
The following benchmarks were used to evaluate which community-led actions offer the most sustainable path to reducing distress in regional Australia.
-
Lived Experience Integration: Prioritizing the voices of those who have personally navigated suicidal distress to inform local responses.
-
Cultural Competency: Ensuring that support frameworks respect and integrate First Nations knowledge and connection to country.
-
Accessibility in Remote Areas: Evaluating how well a strategy overcomes physical distance through mobile or digital means.
-
Demographic Target Accuracy: Focusing on high-risk groups including older men in agricultural sectors and young people in isolated towns.
By applying these criteria, we identified the most effective ways for local leaders and residents to take charge of their community’s well-being.
9 Practical Ways to Support Community Suicide Prevention Australia
Effective prevention in a rural context often looks like neighbors checking in on neighbors rather than a formal hospital admission. The focus for 2026 is on building “gatekeeper” capacity and ensuring that no one is forced to navigate their darkest moments alone. These nine strategies provide a roadmap for regional areas to build resilience from the ground up.
1. Establish Local Lived Experience Networks
Empowering people with a personal history of suicidal distress to lead local conversations is a cornerstone of modern prevention. Organizations like Roses in the Ocean provide the training needed to ensure these individuals can safely share their insights. This ensures that community programs are designed by people who truly understand the barriers to seeking help in a small town.
Best for:
-
Regional councils and health hubs looking to create authentic and relatable support programs.
Why We Chose It:
-
Lived experience leaders break down the stigma that often prevents people from speaking up.
-
It ensures that resources are spent on initiatives that actual survivors find helpful.
-
It builds a local workforce of peers who can provide unique emotional support.
Things to consider:
-
Participants require ongoing clinical supervision and support to prevent personal burnout.
Once a network is established, the community can begin targeting specific high-risk groups with tailored projects.
2. Utilize Small Grants for Targeted Men’s Projects
Men in rural areas represent over 75 percent of suicide deaths, making them a primary focus for Community Suicide Prevention Australia in 2026. Local grants for “grassroots” organizations allow for the creation of walking groups, coffee meetups, and yarning circles. These informal settings allow men to connect without the pressure of a clinical environment.
Best for:
-
Community groups and local sporting clubs looking to support their male members.
Why We Chose It:
-
It meets men where they already gather, such as sheds or sports grounds.
-
Informal settings reduce the “shame” often associated with traditional therapy.
-
Small grants empower local leaders to solve problems in ways that fit their specific town culture.
Things to consider:
-
These groups should have a clear path to professional help if a crisis is identified.
Focusing on specific demographics is vital, but the broader community also needs the skills to identify when someone is struggling.
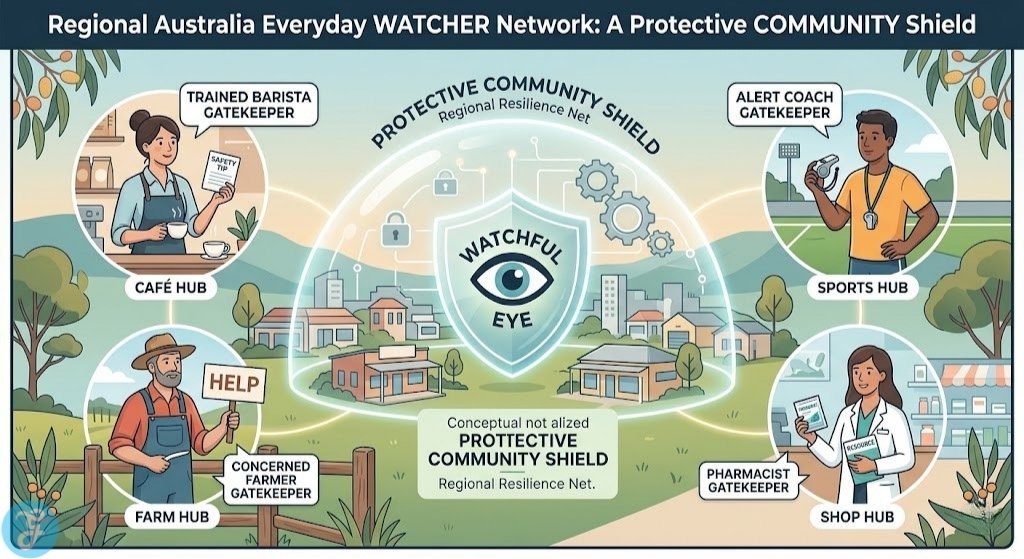
3. Implement Gatekeeper Training for Everyday Leaders
You do not need to be a doctor to save a life. Programs like Wesley LifeForce and Mental Health First Aid train baristas, coaches, and pharmacists to spot the signs of distress. In 2026, the goal is to have at least one trained gatekeeper in every regional business or community hub.
Best for:
-
Business owners, teachers, and community volunteers in remote towns.
Why We Chose It:
-
Gatekeepers are often the first to notice changes in someone’s behavior.
-
Training gives ordinary people the confidence to ask the “suicide question” directly.
-
It creates a safety net that covers the gaps between formal doctor visits.
Things to consider:
-
Skills need to be refreshed every two years to ensure the training remains effective.
While gatekeepers watch over the general population, specific attention must be paid to the cultural safety of First Nations residents.
4. Partner with Aboriginal Community Controlled Health Organisations
The suicide rate among Aboriginal and Torres Strait Islander people remains twice the national average. Effective prevention must be led by the community and centered on cultural wellbeing. Partnering with local ACCHOs ensures that support is grounded in a connection to culture, family, and land.
Best for:
-
Government agencies and non-profits working in regions with high Indigenous populations.
Why We Chose It:
-
ACCHOs provide a holistic model of care that integrates physical and spiritual health.
-
It respects the self-determination of First Nations people in managing their own health.
-
Cultural safety increases the likelihood that individuals will engage with the support offered.
Things to consider:
-
Funding must be long-term and directed by the Aboriginal community themselves.
In addition to cultural frameworks, the physical distance of the outback requires a technological bridge for aftercare.
5. Deploy Digital Aftercare and Follow-Up Services
The period immediately following a hospital discharge or a suicide attempt is the highest risk time for an individual. In regional areas, the WayBack Support Service provides digital and phone-based follow-up to ensure patients are not left alone after a crisis. This bridge is essential when the nearest clinic is hundreds of kilometers away.
Best for:
-
Patients who have recently been discharged from regional emergency departments.
Why We Chose It:
-
It provides a consistent point of contact during the most vulnerable recovery phase.
-
Digital delivery overcomes the “tyranny of distance” in the Australian outback.
-
Regular check-ins can identify a relapse before it leads to another attempt.
Things to consider:
-
Reliable internet and mobile coverage are still barriers in the most remote parts of the country.
While supporting adults is a priority, early intervention in schools can change the trajectory for the next generation.
6. Support School-Led Models like Live4Life
The Live4Life model has been highly successful in rural Victoria by training entire year levels in mental health first aid. This strategy creates a “peer-supported” environment where students look out for one another. By normalizing these conversations in school, the community builds a more resilient future workforce.
Best for:
-
Regional high schools and youth community centers.
Why We Chose It:
-
It targets young people (aged 15 to 24) who are at high risk for self-harm.
-
Peer-to-peer support is often more effective for teenagers than adult intervention.
-
It helps reduce the stigma surrounding mental health from a very early age.
Things to consider:
-
Ongoing funding is required to keep the program running for each new school year.
Supporting schools is just one piece of the puzzle. Bringing different sectors together creates a more unified defense.
7. Coordinate Regional Suicide Prevention Collaboratives
A “Collaborative” brings together police, paramedics, local councils, and health workers to share data and resources. By working together, these stakeholders can identify “hotspots” of distress in a region and deploy resources where they are needed most. This coordinated approach prevents individuals from falling through the cracks between different agencies.
Best for:
-
Regional leaders and local government health planners.
Why We Chose It:
-
It ensures a whole-of-community response rather than isolated efforts.
-
Shared data allows for “real-time” monitoring of suicide trends in a specific area.
-
It creates a unified voice when advocating for federal or state funding.
Things to consider:
-
Privacy and data-sharing agreements must be carefully managed between agencies.
Collaboration is essential, but the way we talk about the issue also plays a role in safety.
8. Normalize Safe Language through Mindframe Training
The way suicide is discussed in local newspapers or on social media can either help or harm. Mindframe provides guidelines for journalists and community members to ensure that language is safe and does not lead to “contagion.” Promoting these standards helps maintain a supportive environment that encourages help-seeking.
Best for:
-
Local media outlets, social media moderators, and community influencers.
Why We Chose It:
-
It prevents the glamorization or sensationalization of a tragic event.
-
Safe language reduces the risk of copycat behavior in vulnerable individuals.
-
It focuses the conversation on help-seeking and available support services.
Things to consider:
-
Monitoring private social media groups for unsafe language can be difficult.
Finally, the unique challenges of rural life require a solution that can move as the community does.
9. Launch Mobile Mental Health Support Hubs
For many in the bush, a trip to the nearest city for a therapy session is not feasible. Mobile hubs bring mental health professionals and peer workers directly to farms and small townships. These vans or pop-up clinics provide a physical presence that signals the community is cared for and supported.
Best for:
-
Remote agricultural communities and isolated mining towns.
Why We Chose It:
-
It removes the transportation barrier for those who cannot leave their work or land.
-
Pop-up hubs are highly visible and act as a reminder that support is available.
-
It allows for face-to-face connection which is often preferred over video calls.
Things to consider:
-
These services are expensive to run and require consistent government investment.
Overview of Community Suicide Prevention Australia in 2026
The current strategy for regional well-being is focused on shifting the power back to the local residents. The table below outlines the primary areas of investment and the key groups benefiting from these programs this year.
The following information summarizes the 2026 focus for regional and rural mental health initiatives.
| Initiative Type | Key Focus | Primary Target Group | 2026 Trend |
| Lived Experience | Peer-led networks | General community | Increasing |
| Men’s Health | Informal hubs/sheds | Older men/Farmers | Growing |
| First Nations | ACCHO-led care | Aboriginal Australians | Priority One |
| Youth Support | School programs | 14-17 year olds | High Demand |
| Digital Support | Video/Phone follow-up | Remote patients | Expanding |
Our Top 3 Critical Factors and Why?
While every tip helps, these three factors will likely have the most immediate impact on the health of regional Australia in 2026.
-
Lived Experience Integration: It is the only way to ensure programs are relevant and free from the stigma that stops rural residents from asking for help.
-
ACCHO Partnership: Given the disproportionate rates of distress in First Nations communities, this is a non-negotiable priority for national safety.
-
Gatekeeper Training: In a region with few doctors, the pharmacist or the footy coach is the most likely person to save a life through early intervention.
How to Support Local Mental Health by Yourself?
You do not need to wait for a government grant to start making a difference in your town. By becoming more aware of your neighbors and the resources available, you can be a vital part of the safety net today.
-
Learn the Signs: Familiarize yourself with the warning signs of distress, such as social withdrawal or giving away possessions.
-
Save Crisis Numbers: Keep the numbers for Lifeline (13 11 14) and 13YARN (13 92 76) in your phone and share them with your local groups.
-
Ask Directly: If you are worried about someone, ask them “Are you thinking about suicide?” in a calm and non-judgmental way.
-
Connect to Culture: Support local First Nations events and initiatives that build a sense of belonging and pride.
The following table can help you determine which resource is most appropriate to share depending on the situation.
| Share Lifeline/13YARN if… | Share Head to Health if… |
| Someone is in immediate distress or crisis. | Someone is looking for long-term therapy or support. |
| You need advice on how to support a friend right now. | You need to find a local mental health service nearby. |
| The person needs a confidential, 24/7 ear to listen. | The situation is stable but requires professional help. |
The Final Checklist
-
[ ] Download the “Safe Conversations” guide from the Mindframe website.
-
[ ] Check if your local Men’s Shed or community center has a mental health liaison.
-
[ ] Save the 13YARN number (13 92 76) for culturally safe support.
-
[ ] Ask your local GP if they offer “Right to Choose” style referrals to digital providers.
-
[ ] Set a “Check-in” reminder to call a neighbor who lives in an isolated area once a week.
Building a Stronger Regional Social Fabric
The challenges of distance and isolation in regional Australia are significant, but the strength of our rural communities is an even greater asset. By embracing a model of Community Suicide Prevention Australia that values lived experience, cultural connection, and everyday gatekeepers, we can turn the tide on these tragic statistics. The goal for 2026 is to ensure that no matter how remote your location, you are part of a network that listens, understands, and acts with compassion.
Frequently Asked Questions About Community Suicide Prevention Australia
Why are suicide rates higher in regional Australia?
Answer: Factors include limited access to health services, higher rates of social isolation, and economic pressures related to weather and industry fluctuations in rural areas.
How do I find a local lived experience network?
Answer: You can contact Roses in the Ocean or your local Primary Health Network to find out which peer-led groups are operating in your specific region.
Is 13YARN different from Lifeline?
Answer: Yes, 13YARN is a national crisis support line specifically for Aboriginal and Torres Strait Islander people, staffed by Indigenous crisis supporters.
Can a school refuse to implement mental health training?
Answer: While schools have autonomy, most regional high schools in 2026 are strongly encouraged to adopt evidence-based programs like Live4Life through government funding.
What is the first thing I should do if someone says they are not okay?
Answer: Listen without judgment, ask them if they are thinking about suicide, and stay with them while you help them contact a crisis service like Lifeline.