As we move through the first quarter of 2026, the NHS continues to face a historic elective care challenge, with waiting lists hovering around 7.3 million people. However, the 2025/26 operational year has introduced significant digital and legal shifts designed to put power back into the hands of the patient. While the headline figures can be daunting, savvy users of the system are increasingly using “insider” pathways—ranging from mutual aid systems to enhanced app features—to shave months off their wait times. Understanding NHS waiting times 2025 tips is no longer just about patience; it is about active navigation within a reforming system.
Our Selection Methodology
To curate this list, we analyzed the latest 2025/26 NHS England Operational Planning Guidance, current data from the Patient Initiated Digital Mutual Aid System (PIDMAS), and the updated NHS Choice Framework. We prioritized tips that leverage the newest 2026 digital features of the NHS App and the recently expanded powers of Integrated Care Boards (ICBs). Our criteria focused on “legitimate shortcuts”—legal rights and technical tools that are available to all patients but often go underutilized because they are not proactively offered by overstretched GP surgeries.
10 Insider Tips for NHS Waiting Times in 2025/26
The key to reducing your wait is moving from a passive “waiting list” mindset to an active “care management” approach.
1. Activate the NHS App “Waiting List” Transparency Feature
In early 2026, the NHS App received a major update allowing patients to see their exact position on a waiting list and the estimated “8 in 10” wait time for their specific specialty.
-
Best for: Patients who want a realistic timeline to plan their lives, work, and finances.
-
Things to consider: The data is refreshed weekly; if your estimated wait suddenly jumps, it is often due to a surge in high-priority clinical emergency cases in your trust.
This visibility prevents you from being “lost in the system” and provides the data you need to decide if you should explore alternative providers.
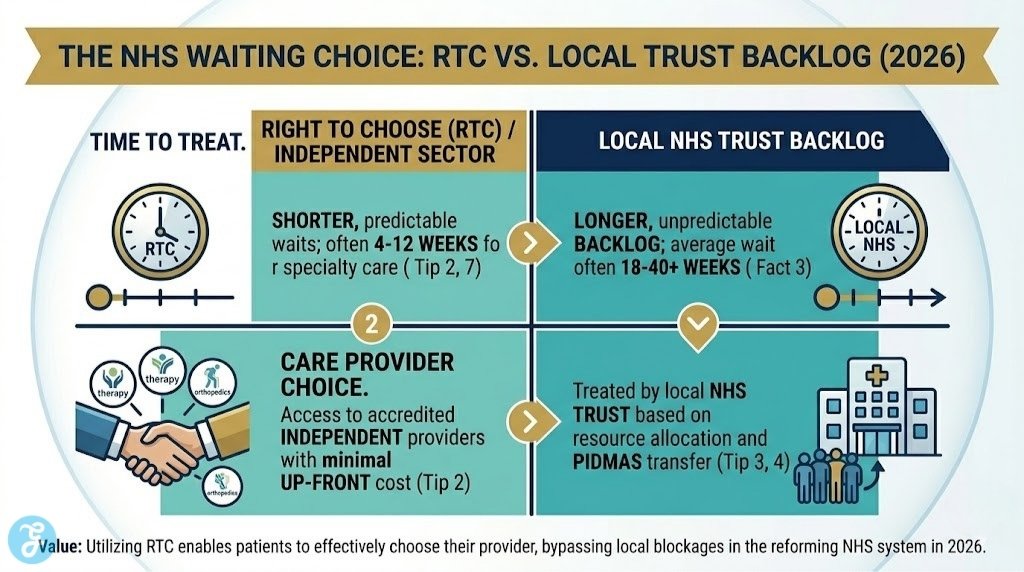
2. Leverage “Right to Choose” for Mental Health and ADHD
The 2025/26 “Indicative Activity Plans” have changed how Right to Choose (RTC) works. You still have the legal right to choose any provider (including private ones with NHS contracts) if your local wait is too long.
-
Best for: Neurodiversity assessments and mental health therapy where local NHS waits often exceed two years.
-
Things to consider: Some Integrated Care Boards (ICBs) have “activity pauses” in place until April 2026 for certain private providers, so always check the current “accepted referrals” status of your chosen clinic first.
Using RTC is the single most effective way to access specialist private-sector care at zero cost to you.
3. Utilize the 40-Week “PIDMAS” Transfer
Under the Patient Initiated Digital Mutual Aid System (PIDMAS), if you have been waiting for more than 40 weeks and do not have a TCI (To Come In) date, you can request to be moved to a hospital with a shorter list.
-
Best for: Patients stuck in high-demand specialties like Orthopaedics (hips and knees) or Ophthalmology.
-
Things to consider: The “mutual aid” might require you to travel to a different city, but the NHS will often provide support for travel and accommodation if you meet certain criteria.
Initiating a PIDMAS request forces the system to look for capacity elsewhere in the country on your behalf.
4. Request “Advice and Guidance” (A&G) via Your GP
Before a formal referral is made, your GP can use the “Advice and Guidance” digital platform to get a specialist’s opinion within days rather than months.
-
Best for: Complex conditions that might not require a physical hospital visit if a specialist can suggest a treatment plan for your GP to follow.
-
Things to consider: A&G can sometimes lead to a “Straight to Test” pathway, bypassing the initial outpatient consultation entirely.
This “consultant-lite” approach can often resolve your issue without you ever having to join a formal hospital waiting list.
5. Opt for a Community Diagnostic Centre (CDC)
The NHS has rolled out over 160 CDCs in shopping centers and community hubs as of 2026, specifically to separate “well” diagnostic patients from “sick” hospital patients.
-
Best for: Getting MRI, CT scans, and ultrasounds done faster and in a more convenient location.
-
Things to consider: When your GP refers you for a scan, specifically ask if there is a CDC nearby; they often have significantly shorter queues than major acute hospitals.
CDCs are the “engine room” of the 2026 backlog recovery, designed specifically to break the diagnostic bottleneck.
6. Get on the “Short-Notice Cancellation” List
Hospital departments frequently deal with “DNAs” (Did Not Attend) and last-minute cancellations.
-
Best for: People with flexible schedules who can travel to a clinic or theatre within 24–48 hours.
-
Things to consider: You must proactively call the “Booking Office” or the “Consultant’s Secretary” to ask to be noted as “available at short notice.”
Being the person who fills a gap in a surgeon’s morning list can jump you ahead of hundreds of other patients.
7. Assert Your “18-Week Right” via the ICB
The NHS Constitution states you have the legal right to start non-urgent consultant-led treatment within 18 weeks of referral.
-
Best for: Patients who have hit the 18-week mark and have not been offered a definitive treatment date.
-
Things to consider: If the 18-week target is missed, you can contact your local ICB (Integrated Care Board) and demand they find you an alternative provider who can see you sooner.
The ICB has a legal obligation to investigate and offer you a range of suitable alternative hospitals or clinics.
8. Use the “My Planned Care” Portal for Data-Driven Choices
The “My Planned Care” website provides the most up-to-date average wait times for every hospital in England, broken down by department.
-
Best for: Comparing local trusts before your GP sends the referral.
-
Things to consider: Use this data during your GP appointment to ensure the referral is sent to the trust with the shortest current backlog, not just the closest one.
Choosing the right hospital at the point of referral can save you 20–30 weeks of waiting before you even start.
9. Push for “Straight to Test” Pathways
In 2026, many trusts have adopted “Straight to Test” for suspected cancer or heart issues, where you go directly for a diagnostic scan before seeing a consultant.
-
Best for: Fast-tracking the 28-day “Faster Diagnosis Standard.”
-
Things to consider: If your GP is referring you for a “2-week wait” (urgent) pathway, ask if the trust uses “Straight to Test” to ensure you get your results as quickly as possible.
This removes the unnecessary middle-man appointment, getting you to a diagnosis and treatment plan much faster.
10. The “Patient Deal”: Preparing for Surgery
Under the 2026 “Patient Deal” initiative, patients who are “pre-habilitated” (fit for surgery) are prioritized for theatre slots.
-
Best for: Reducing the risk of your surgery being cancelled on the day due to health complications.
-
Things to consider: Use the time on the waiting list to improve your fitness, quit smoking, or manage blood pressure; the NHS is increasingly using “fitness for surgery” as a secondary triage tool.
Being in the best possible shape ensures that when a slot opens up, you are the first choice to fill it.
Strategic Analysis
The shifting landscape of 2026 means that “location” is no longer the primary factor in how fast you are treated. The table below compares the traditional “passive” approach with the modern “active” navigation strategies.
| Feature | Traditional Waiting (Passive) | Modern Navigation (Active) | 2026 Benefit |
| Referral Choice | Nearest Hospital | “My Planned Care” Comparison | Save 4–6 Months avg. |
| Long Wait Help | Wait for Letter | PIDMAS Transfer (40 weeks) | Move to a shorter list. |
| Mental Health | Local NHS Wait | “Right to Choose” (RTC) | Access Private at £0 cost. |
| Diagnostics | Hospital X-ray Dept. | Community Diagnostic Centre | Faster “Straight to Test.” |
Our Top 3 Picks And Why?
-
The NHS App Waiting List Feature: This is our top pick because “knowledge is power.” Seeing your real-time position removes the anxiety of the unknown and allows you to hold your trust accountable.
-
Right to Choose (RTC): We chose this because it is the most effective “legal loophole” to bypass the worst of the NHS backlogs, particularly for specialist mental health services.
-
The 40-Week PIDMAS Move: This is a critical pick for 2026 because it represents the first time the NHS has created a national “mutual aid” system that allows patients to effectively “shop” for the shortest queue across the entire country.
Preparation Checklist
-
[ ] Log into the NHS App and verify your “Waiting List” status is visible and correct.
-
[ ] Use “My Planned Care” to check the current wait time for your specific specialty at your local trust.
-
[ ] Ask your GP for “Advice and Guidance” (A&G) if your condition is stable but needs specialist input.
-
[ ] Identify your local Integrated Care Board (ICB) contact details for “Choice” complaints.
-
[ ] If you have waited 40+ weeks, proactively ask your consultant’s secretary about a PIDMAS transfer.
-
[ ] Check if there is an NHS Community Diagnostic Centre (CDC) within a 30-mile radius of your home.
Mastering the New Era of Patient Choice
The era of “blindly waiting” for the NHS is coming to an end. By utilizing the digital tools and legal rights established in 2025 and expanded in 2026, patients can take control of their own healthcare journeys. Whether it’s moving your care to a different city via PIDMAS or choosing a private specialist through the Right to Choose framework, the system is now designed to reward those who are proactive. While the backlogs remain a challenge, these NHS waiting times 2025 tips provide the roadmap needed to navigate the system with confidence and speed.
FAQs
Can the NHS refuse my “Right to Choose” request?
Only in limited circumstances, such as if the provider doesn’t have a valid NHS contract or if the referral is for emergency or maternity care.
Does moving via PIDMAS cost me money?
No, the treatment remains free. If you are on a low income, you may even be able to claim back travel costs for the new hospital.
Is the 18-week target still a legal right?
Yes, it is part of the NHS Constitution, though in practice, it is currently an “interim target” rather than a guaranteed reality for every single patient.