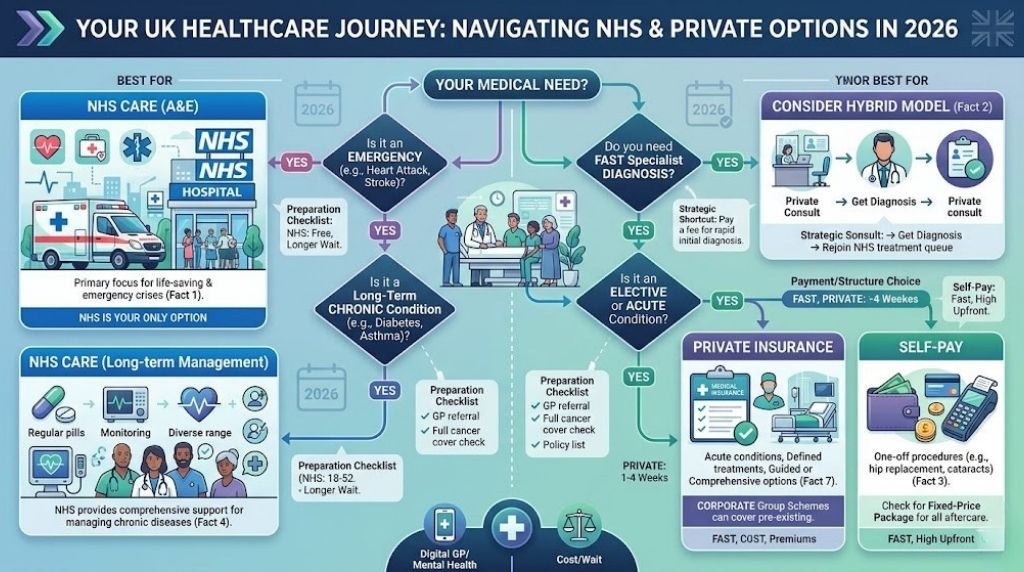
The British healthcare system is often viewed as a binary choice between the publicly funded NHS and the premium world of private clinics. However, in 2026, the lines between these two have blurred significantly, creating a nuanced environment that many residents don’t fully understand. Whether you are considering a policy for the first time or looking to speed up a specific procedure, knowing the inner workings of private healthcare in UK is essential for making an informed decision about your well-being.
Our Selection Methodology
To identify these seven critical insights, we analyzed the latest 2026 healthcare market reports, insurance policy data, and patient outcome statistics from the Independent Healthcare Providers Network (IHPN). We focused on areas where public perception frequently clashes with the reality of how private medical insurance (PMI) and self-pay treatments actually function. Each point was selected based on its impact on the average patient’s wallet, wait time, and quality of care, with a specific focus on the shifting trends of the post-pandemic era.
Unveiling the Reality of Private Healthcare in UK
As NHS waiting lists remain a primary concern for many, the private sector has adapted to fill specific gaps. Here are the most important things you likely didn’t know about how private care operates today.
1. The Absence of Private Accident & Emergency (A&E)
A common misconception is that paying for private care guarantees a faster response during a life-threatening emergency. In reality, almost no private hospital in the UK operates a full-scale A&E department. For heart attacks, major trauma, or strokes, the NHS is your only option.
Best for: Elective surgeries, specialist consultations, and planned diagnostic tests rather than emergency medical crises.
Things to consider: If you are admitted to a private hospital and your condition becomes critical, you will likely be stabilized and then transferred via ambulance to an NHS facility that has an Intensive Care Unit (ICU).
While private hospitals excel at planned care, they also offer a strategic shortcut for those who ultimately want to stay within the NHS.
2. The Private-to-NHS Referral “Fast-Track”
Many people don’t realize you can use private healthcare in UK to get a rapid diagnosis from a consultant and then use that diagnosis to rejoin the NHS queue for treatment. This “hybrid” approach allows you to skip the long wait for an initial specialist appointment.
Best for: Patients who can afford a one-off consultation fee (approx. £200–£300) but cannot afford the full cost of a private surgery.
Things to consider: You must ensure your private consultant also works within the NHS or can provide a formal referral letter that your GP can process to place you on the public surgical list.
This hybrid model is part of a larger trend where more people are paying for individual treatments out of pocket.
3. The Rise of the “Self-Pay” Patient
You don’t need a monthly insurance policy to access private clinics. In 2026, roughly 20% of all private patients in the UK are “self-funders” who pay for specific one-off procedures, such as cataract surgery or hip replacements, directly from their savings.
Best for: Individuals with specific, non-urgent medical needs who want to avoid the long-term commitment of insurance premiums.
Things to consider: Costs can be high; a hip replacement can range from £12,000 to £15,000, so it is vital to get a “fixed-price package” quote that includes all aftercare and follow-up appointments.
Regardless of how you pay, it is crucial to understand that private care is not a “fix-all” for every health issue.
4. Strict Exclusions for Chronic Conditions
Private medical insurance is almost exclusively designed to cover “acute” conditions—illnesses that are curable and short-term. Most policies will not cover long-term management for chronic diseases like diabetes, asthma, or certain autoimmune disorders.
Best for: Sudden injuries, new illnesses, and conditions that require a specific surgical intervention or a defined course of treatment.
Things to consider: If you develop a chronic condition while on a policy, the insurer may cover the initial “flare-up” but will eventually refer you back to the NHS for long-term management.
Interestingly, the demographic of people seeking this type of acute care has shifted dramatically in recent years.
5. Surprising Adoption Among Younger Generations
While private healthcare was once seen as a luxury for the elderly, 2026 data shows that the 18–34 age group is now the fastest-growing demographic for private insurance. This shift is driven by a desire for rapid mental health support and virtual GP access.
Best for: Young professionals who value time-efficiency and want 24/7 access to digital medical consultations through their smartphones.
Things to consider: Many “youth-focused” policies offer lower premiums but higher excesses, meaning you pay more out of pocket for the first claim each year.
This surge in demand has also opened doors to treatments that simply aren’t available on the public purse.
6. Access to Non-NICE Approved Medications
The NHS is bound by the National Institute for Health and Care Excellence (NICE) guidelines, which determine which drugs are “cost-effective.” Private healthcare providers can often offer life-extending or cutting-edge drugs that have not yet been approved for general NHS use.
Best for: Patients seeking specific oncology treatments or specialized medications that are common in the US or Europe but restricted by NHS budgets.
Things to consider: Even if a drug is available privately, it can be prohibitively expensive if not covered by a very high-level “comprehensive” insurance plan.
Even with the best insurance, your choice of doctor might be more limited than you expect.
7. The Hidden Limitation of “Guided” Specialists
Many modern insurance policies offer a “Guided” or “Pathway” option which reduces premiums by about 20%. However, this means the insurer chooses your consultant for you from a small, pre-approved list, rather than letting you pick the top specialist in the country.
Best for: Budget-conscious individuals who prioritize lower monthly costs over having a specific surgeon.
Things to consider: If you have a very rare condition, a guided list might not include the one specialist who is most qualified to treat your specific issue.
Strategic Analysis
Choosing how to navigate private healthcare in UK depends on your financial flexibility and your specific health risks. The table below compares the three primary ways to access care in 2026.
| Feature | NHS Care | Private Insurance | Self-Pay (One-off) |
| Average Wait Time | 18–52 Weeks | 1–4 Weeks | 1–2 Weeks |
| Cost Profile | Free at point of use | Monthly Premiums | High Upfront Cost |
| Specialist Choice | Assigned by hospital | Limited by policy | Full Choice |
| Chronic Coverage | Full Support | Usually Excluded | Per-procedure only |
Our Top 3 Picks And Why?
-
Hybrid Pathway (Private Diagnosis): This is the best value for most people, as it uses a small investment to bypass the longest part of the NHS wait (the initial referral).
-
Corporate Group Schemes: If your employer offers health insurance as a benefit, it is almost always worth taking, as they often cover pre-existing conditions that personal policies would exclude.
-
Comprehensive Personal Insurance: For those over 50, a full policy is the most reliable way to ensure that age-related elective surgeries are handled quickly and comfortably.
Preparation Checklist
Before committing to a policy or a private procedure, make sure you have addressed the following:
-
Obtain a referral letter from your NHS GP (even for private care, this is often required).
-
Check if your “acute” condition has any “chronic” overlap that might lead to a claim rejection.
-
Verify if your preferred local hospital is on your insurer’s “approved list.”
-
Compare the cost of 12 months of premiums against the one-off “self-pay” price for the procedure you actually need.
-
Confirm whether your policy includes “Full Cancer Cover,” as some basic plans have strict financial caps on chemotherapy.
Mastering Your Healthcare Strategy in 2026
Understanding the nuances of private healthcare in UK allows you to use the system as a tool rather than a replacement for public services. By identifying which conditions are best suited for the private sector—such as rapid diagnostics and elective surgeries—you can protect your health without overspending on unnecessary coverage. In an era where the NHS is under sustained pressure, a targeted approach to private care is the most effective way to ensure you receive the right treatment at the right time.
FAQs
Is private healthcare better than the NHS?
Private care is generally faster and more comfortable for elective issues, but the NHS is superior for emergency care and complex, long-term chronic conditions.
Do I need a GP referral to see a private consultant?
While some clinics allow self-referral, most consultants and all insurance companies require a GP referral letter to ensure the specialist is appropriate for your symptoms.
Will my premiums go up if I make a claim?
Most UK health insurance providers use a “no claims discount” system, so your premium will typically increase the following year if you have utilized the service.
Can I switch from private back to the NHS?
Yes. Using private care does not forfeit your right to NHS treatment; you can move between the two systems as your needs and budget change.