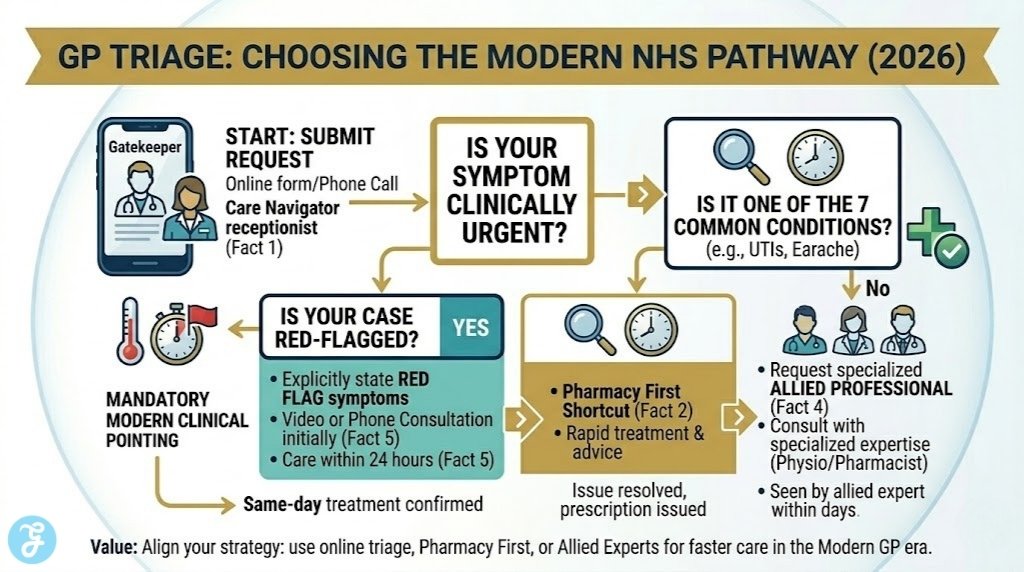
The traditional “8 a.m. scramble” for a doctor’s visit is officially becoming a relic of the past. As of early 2026, the NHS has fully transitioned into the “Modern General Practice Access” model, a structural overhaul that replaced first-come-first-served queues with sophisticated digital triage and multi-professional teams. While the system is designed to be more equitable, it requires a new set of skills from patients to ensure they are seen by the right person at the right time.
Navigating NHS GP appointments 2025 tips in this new era is less about “beating the system” and more about providing the high-quality data that clinical teams need to prioritize your care.
Our Selection Methodology
To develop this guide, we synthesized the 2025/26 NHS GP Contract changes, the 2026 Healthwatch England “Experience Reports,” and the latest digital roadmap for the NHS App. We prioritized strategies that align with the new mandatory “continuous online access” rules and the “no call-back tomorrow” policy. Our selection criteria focused on steps that provide the greatest time-saving impact for patients—specifically those that leverage the newly integrated Pharmacy First pathways and the shift toward specialized allied health professionals like first-contact physiotherapists and clinical pharmacists.
8 Proven Steps to Get the Most from Your NHS GP Appointments in 2025/26
The secret to a successful consultation in 2026 lies in your preparation before you even pick up the phone or open an app.
1. Use the Online “Triage” Form During Core Hours
Under the latest 2025/26 contract, every GP surgery in England is now legally required to keep their online consultation forms open from 8:00 a.m. to 6:30 p.m. for all routine and administrative queries.
-
Best for: Patients with non-urgent symptoms or those who need sick notes, test results, or medication reviews without waiting on a phone line.
-
Things to consider: These forms are reviewed by a “Care Navigator” or a GP, so being extremely detailed about your symptoms—including duration and severity—increases your chance of getting an earlier slot.
Submitting your request digitally creates a clear audit trail and allows the clinical team to assess your needs far more accurately than a brief 30-second phone call.
2. Adopt the “Pharmacy First” Shortcut
If you have one of the seven common conditions (including earache, sore throat, or uncomplicated UTIs), you can now bypass the GP surgery entirely by going directly to a community pharmacist.
-
Best for: Rapid treatment for minor ailments where you might otherwise wait several days for a GP review.
-
Things to consider: Pharmacists can now issue prescription-only medicines for these conditions; if your case is too complex, they have a direct digital link to escalate you back to your GP immediately.
Utilizing your local pharmacy as the first point of call is the most effective way to protect GP slots for patients with chronic or complex illnesses.
3. Assert Your “Next Day Response” Right
The 2026 GP contract mandates that practices must not ask you to “call back tomorrow.” Every request must receive a response by the end of the next working day confirming exactly what will happen next.
-
Best for: Reducing the anxiety of the unknown and preventing the cycle of daily phone calls.
-
Things to consider: This “response” might not be an immediate appointment; it could be a request for more information, a referral to another service, or a scheduled call for the following week.
Understanding this right allows you to hold your surgery accountable if they attempt to push you back into a daily booking loop.
4. Request a Specific “Multi-Professional” Slot
Modern surgeries are no longer just staffed by GPs; they include clinical pharmacists, physiotherapists, and mental health practitioners who are often better suited to specific issues.
-
Best for: Musculoskeletal issues (physios) or medication adjustments (pharmacists) where a general doctor might simply refer you elsewhere anyway.
-
Things to consider: Seeing an “allied professional” is often much faster than waiting for a GP, and they have the same power to prescribe or order tests within their specialty.
Explicitly asking for a specialist clinician can often move your appointment forward by days or even weeks.
5. Optimize Your “Same-Day” Urgent Request
For clinically urgent issues, the 2026 standard requires a same-day response, with 90% of these patients receiving care within 24 hours.
-
Best for: Sudden-onset illnesses or worsening chronic conditions that cannot wait for a routine review.
-
Things to consider: To qualify for “Same-Day” care, you must be prepared to accept a phone or video consultation initially, as this is how clinicians now triage the most urgent cases.
Clear, concise communication of your “red flag” symptoms is essential to ensure your request is categorized correctly by the triage team.
6. Master the NHS App “Self-Serve” Features
By early 2026, the NHS App has become a comprehensive portal for viewing test results, managing referrals, and even checking your position on hospital waiting lists.
-
Best for: Avoiding a 10-minute phone call just to hear that your blood tests were “normal.”
-
Things to consider: Many surgeries now release results to the app as soon as they are reviewed by a doctor, meaning you often see them before the surgery staff have time to call you.
Moving your administrative tasks to the app frees up phone lines for elderly or vulnerable patients who cannot use digital tools.
7. Leverage the “Call-Back” Telephony Feature
The vast majority of GP surgeries have now implemented “Cloud Telephony,” which allows you to request a call-back rather than waiting in a “Position 40” queue.
-
Best for: Patients who need to call but cannot afford to spend 45 minutes on hold during their workday.
-
Things to consider: Ensure your phone is not on “Silent” or “Do Not Disturb,” as the automated system will often only try to reach you once before moving to the next person.
Using the call-back feature is the most stress-free way to maintain your place in the morning queue without active waiting.
8. Prep Your “Patient Deal” Summary
Surgeries are increasingly adopting “The Patient Deal,” a transparency charter that encourages patients to bring a written summary of their concerns to the consultation.
-
Best for: Making the most of the standard 10–15 minute appointment window.
-
Things to consider: Focus on your “one main concern” first; trying to address three separate issues in one short slot often leads to a rushed and less effective consultation.
Coming prepared with your symptoms, their duration, and what you’ve already tried (like over-the-counter meds) helps the doctor reach a diagnosis faster.
Strategic Analysis
The 2026 primary care landscape is defined by “Choice of Access.” The table below outlines how to select the right entry point based on your specific needs.
| Your Need | Recommended Entry Point | 2026 Response Standard |
| Common Ailment (e.g., Earache) | Pharmacy First | Immediate / Walk-in |
| Routine Review / Admin | Online Triage Form | Response by next working day |
| Urgent Symptom | Phone or Digital Triage | Same-day assessment |
| Chronic Condition Management | NHS App Messaging | Scheduled review |
Our Top 3 Picks And Why?
-
Online Triage during Core Hours: This is our top pick because it is the most reliable way to provide detailed information without the pressure of a phone queue. It ensures your case is handled based on clinical need, not just who dialed fastest.
-
Pharmacy First Direct Access: We chose this because it is a true “shortcut.” It allows for professional clinical care and prescriptions for common issues in a high-street setting, often with zero wait time.
-
Multi-Professional Appointments: This pick is critical for 2026 because the “GP-only” mindset is a bottleneck. Accessing a physio or pharmacist directly is almost always faster and provides more specialized care for specific ailments.
Preparation Checklist
-
[ ] Log into your NHS App and ensure your “Online Consultations” feature is linked to your surgery.
-
[ ] Identify your nearest “Pharmacy First” provider for quick access to minor ailment care.
-
[ ] Draft a “three-point summary” of your symptoms before submitting any online or phone request.
-
[ ] Check your surgery’s website for their specific “Patient Charter” to understand their local response times.
-
[ ] Update your contact details in the NHS App to ensure you receive automated appointment reminders and “Call-Back” notifications.
Taking Control of Your Primary Care Journey
The NHS GP system in 2026 is no longer a passive service—it is a partnership. By following these NHS GP appointments 2025 tips, you move from being a frustrated voice in a phone queue to a proactive manager of your own health. The combination of digital triage, the Pharmacy First initiative, and a broader range of clinical specialists means that while the front door looks different, it is actually more accessible than ever for those who know how to use it. Your next appointment isn’t just a booking; it’s a strategic step toward faster, more effective care.
FAQs
What if I can’t use a smartphone or the internet?
Surgeries must still provide “equitable access.” You can still phone or walk in, and a receptionist (trained as a Care Navigator) will fill out the triage form on your behalf.
Can a pharmacist really give me antibiotics?
Yes, for the seven specific common conditions covered by Pharmacy First, provided you meet the clinical criteria during your consultation.
Is “Call Back Tomorrow” officially banned?
Yes, under the 2026 contract, surgeries must provide a definitive “next step” within one working day rather than asking you to start the process over again.