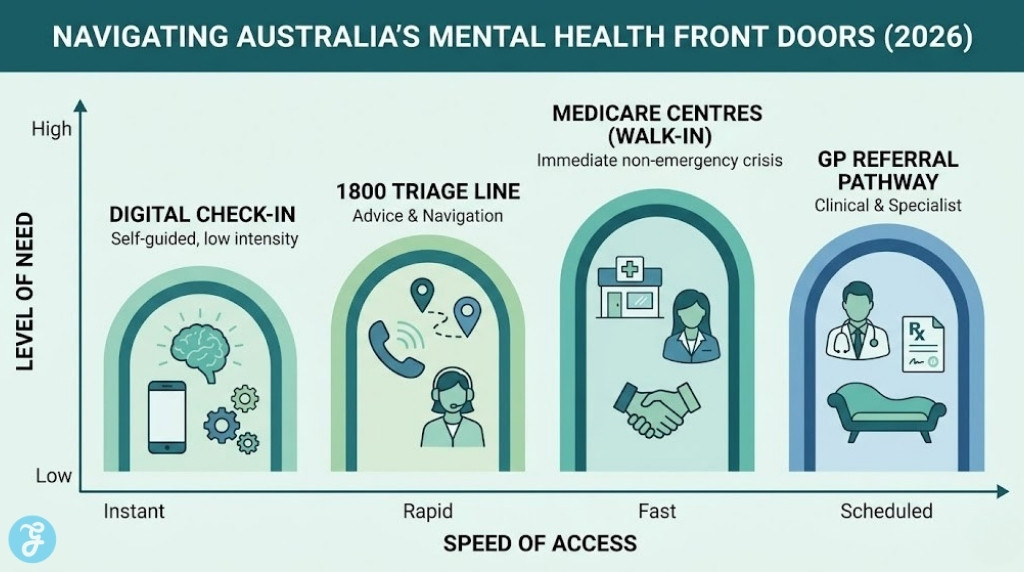
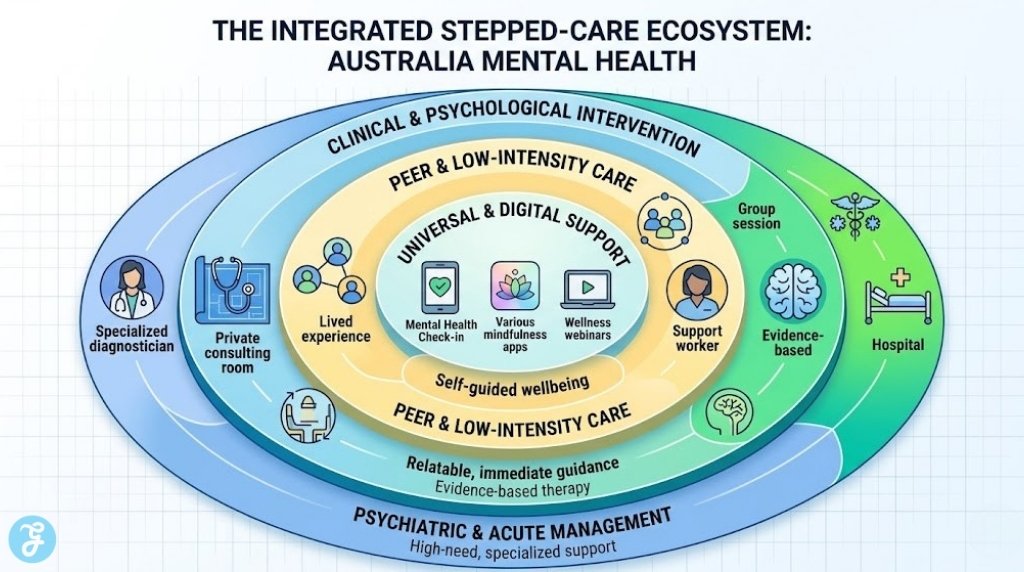
Navigating the mental health landscape in Australia has become increasingly complex as the government introduces a range of new “Medicare Mental Health” services. In 2026, the focus has shifted toward making early intervention more accessible by removing traditional barriers like GP referrals for certain entry-level supports. Understanding these shifts is vital for anyone seeking timely assistance for themselves or their loved ones.
How We Selected Our 10 Best Facts About the Australian Mental Health System 2026
To curate this list, we analyzed current federal health department updates and the latest 2026-27 pre-budget submissions from major psychiatric bodies. Our focus was on identifying changes that directly impact patient access, cost, and the variety of care formats available to the public.
-
Accessibility: We prioritized facts regarding new “walk-in” and “referral-free” services.
-
Financial Relevance: We looked at Medicare rebate structures and bulk-billing trends for the current year.
-
Technological Integration: We evaluated the rollout of the new 2026 digital check-in platforms.
The following criteria were used to filter and rank the most essential information for the current health environment.
| Selection Factor | Priority Level | Goal of Inclusion |
|---|---|---|
| Direct Patient Cost | High | Clarifying out-of-pocket expectations |
| Referral Pathways | High | Explaining how to access care faster |
| Service Rollout Status | Medium | Confirming if services are live in 2026 |
| Workforce Availability | Medium | Managing expectations on wait times |
Essential Insights: 10 Australian Mental Health System 2026 Facts
These ten pillars define the current state of support in Australia, highlighting a system that is moving toward a more decentralized and digital-friendly model. Knowing these facts can save you time and ensure you are using the most cost-effective pathways available.
1. Medicare Mental Health Centres Offer Walk-In Support
A major shift in 2026 is the widespread availability of Medicare Mental Health Centres, formerly known as Head to Health. These physical locations allow any Australian to walk in and speak with a professional without a prior appointment or a doctor’s referral, providing a critical safety net for those in immediate distress.
Best for: Immediate, face-to-face support without a pre-booked appointment.
Why We Chose It: It represents the largest physical expansion of the “no-barrier” care model in recent years.
Things to consider: While walk-ins are free, specialized long-term therapy may still require a transition to a different provider.
2. The Digital “Check In” Service Is Now Fully Operational
Launched at the start of 2026, the Medicare Mental Health Check-In is a free digital service providing low-intensity therapy. This platform uses evidence-based cognitive behavioral techniques and offers the choice between self-guided tools or support from a trained practitioner via phone or video.
Best for: Early intervention and building practical skills through digital tools.
Why We Chose It: It addresses the “missing middle” for people who need support but do not have a formal clinical diagnosis.
Things to consider: The full suite of interactive tools is scheduled to reach maturity by the middle of 2026.
3. Medicare Still Subsidizes 10 Individual Therapy Sessions
The Better Access initiative remains a cornerstone of the system, providing Medicare rebates for up to 10 individual and 10 group therapy sessions per calendar year. This benefit is intended for patients with a clinically diagnosed mental disorder who are working through a structured treatment plan with a psychologist or social worker.
Best for: Individuals with a diagnosed mental health condition seeking structured therapy.
Why We Chose It: It is the primary financial mechanism for affordable private psychological care in Australia.
Things to consider: You must visit a GP first to obtain a Mental Health Treatment Plan to unlock these rebates.
4. Dedicated Kids Hubs Target Early Childhood Development
By mid-2026, the government aims to have 17 Kids Hubs established across the country to support children aged 0 to 12. these centers provide a multidisciplinary approach, bringing together pediatricians, psychologists, and social workers to assist families dealing with developmental or emotional challenges.
Best for: Families and children aged 0 to 12 needing developmental or emotional support.
Why We Chose It: It addresses a significant gap in specialist pediatric mental health services.
Things to consider: These hubs are still rolling out, so availability may vary depending on your specific region.
5. New Pathways Bypass the Need for a GP Referral
One of the most significant changes in 2026 is the “Referral-Free” entry point. While the 10 sessions mentioned earlier still need a doctor’s note, the new Medicare Mental Health phone lines and walk-in centers do not, allowing people to get professional advice much faster than waiting for a GP opening.
Best for: People experiencing mild distress who want to avoid the GP referral wait time.
Why We Chose It: This removes one of the most cited barriers to seeking help: the “GP gatekeeper” delay.
Things to consider: A GP referral is still necessary if you want to see a specific private psychologist under Medicare.
6. Specialist Psychiatrist Shortages Impact Regional Wait Times
Despite increased funding, Australia currently only has approximately 16 psychiatrists for every 100,000 people. This workforce shortage is particularly acute in rural and regional areas, where patients may face months of waiting for a specialist assessment or medication review.
Best for: Understanding why wait times for specialists remain a challenge in regional areas.
Why We Chose It: It provides a realistic perspective on the limitations of the current system.
Things to consider: Telehealth is the primary tool being used to bridge this gap for regional patients in 2026.
7. A Centralized Phone Service Now Coordinates Care
The 1800 595 212 number has been established as a nationwide “front door” for mental health support. Trained professionals on this line can perform brief assessments and directly link callers to free or low-cost local services that match their specific needs.
Best for: First-time help-seekers who are unsure where to start their journey.
Why We Chose It: It simplifies a very fragmented system into a single, easy-to-remember point of contact.
Things to consider: This is a navigation and advice service, not a long-term counseling line.
8. Bulk Billing Incentives Are Targeting Mental Health Care
In 2026, there is a renewed push to increase bulk-billing rates for mental health consultations to reduce rising out-of-pocket costs. Many practitioners now receive higher government incentives to bulk-bill children and concession card holders, making care more affordable for vulnerable groups.
Best for: Concession card holders and low-income earners seeking reduced costs.
Why We Chose It: Financial pressure is a leading cause of psychological distress in the current economy.
Things to consider: Many private psychologists still charge a “gap fee” that is not covered by Medicare.
9. Telehealth Has Become a Permanent System Feature
Telehealth is no longer a temporary measure and is fully integrated into the Australian health system in 2026. This includes Medicare rebates for video and phone consultations, as well as specialized group therapy sessions for those living in remote areas.
Best for: Rural residents or those with mobility issues needing specialist access.
Why We Chose It: It has fundamentally changed how Australians in remote areas access city-based specialists.
Things to consider: Some practitioners may still prefer a face-to-face initial consultation for certain diagnoses.
10. Peer Workers Are Integrated into Standard Care Teams
The 2026 service model places a high value on “lived experience” workers. These are individuals who have successfully navigated their own mental health challenges and are now trained to work alongside clinicians in Medicare Mental Health Centres to provide unique, relatable support.
Best for: Users who prefer a non-clinical, peer-led approach to recovery.
Why We Ches It: Peer support has been shown to improve engagement and long-term recovery outcomes.
Things to consider: Peer workers work in tandem with clinical staff and do not replace medical advice.
An Overview Of 10 Australian Mental Health System 2026 Facts
To help you decide which service is right for you, it is useful to compare the different entry points based on your level of need and how quickly you need help. This comparison highlights the differences between the traditional referral model and the newer direct-access options.
| Service Type | Access Method | Cost to Patient | Referral Needed? |
|---|---|---|---|
| Medicare Centres | Walk-in / Phone | Free | No |
| Digital Check-In | Online / App | Free | No |
| Private Psychologist | Appointment | Rebated (Gap fee likely) | Yes (GP MHTP) |
| Kids Hubs | Walk-in / Referral | Free | No (but recommended) |
| Psychiatrist | Appointment | Rebated (Gap fee likely) | Yes (GP or Specialist) |
Our Top 3 Picks and Why?
-
Medicare Mental Health Centres: This is our top choice for immediate help. The ability to walk into a professional setting without a referral or a bill is a game-changer for people who feel overwhelmed by the complexity of the traditional medical system.
-
The Digital Check-In Service: We chose this as a top pick because it solves the “waiting list” problem. It provides instant access to evidence-based tools at the very first sign of distress, which can prevent a minor issue from becoming a crisis.
-
The 1800 595 212 Phone Line: This is essential for anyone feeling lost. Instead of calling multiple clinics to check for availability, one call can help you find a provider that is actually taking new patients and fits your budget.
How to Choose the Right Australian Mental Health System 2026 by Yourself?
Choosing the right path depends on your symptoms, your budget, and how much time you can afford to wait. The following framework helps you categorize your needs so you can act quickly and effectively.
The Selection Framework
-
Assess the Urgency: If you are in a crisis, bypass the standard system and call Triple Zero or go to an Emergency Department.
-
Evaluate Your Symptoms: For mild stress or anxiety, digital tools are the fastest. For long-term or complex issues, a GP referral to a psychologist is better.
-
Consider Your Budget: Always ask if a clinic “bulk-bills.” If they do not, ask exactly what the “out-of-pocket gap” will be before your first visit.
-
Location Check: Use the online Medicare Mental Health map to see if there is a walk-in center within your local government area.
The following matrix helps you match your current situation to the most appropriate service available in 2026.
| Choose Direct Access (Walk-in/Phone) if… | Choose the Referral Path (GP) if… |
|---|---|
| You need help today but it is not a life-threatening emergency. | You want to see a specific private therapist you have researched. |
| You do not have a regular GP or cannot get an appointment. | You need a formal diagnosis for insurance or work purposes. |
| You want free support and do not mind seeing a rotating team. | You require long-term, specialized psychological therapy. |
| You are looking for low-intensity, practical coping skills. | You need a psychiatrist for medication management. |
The Final Checklist
-
Have you checked if your local Medicare Mental Health Centre is open after hours?
-
Do you have your Medicare card ready for any phone or digital registrations?
-
If seeing a private psychologist, have you confirmed their “gap fee” in writing?
-
Has your GP uploaded your Mental Health Treatment Plan to your My Health Record?
-
Are you aware of the wait times for your specific specialist before you book?
The Future of Australian Care
The Australian mental health system in 2026 is clearly moving toward a more user-centric model that prioritizes early intervention and digital flexibility. By utilizing the new referral-free pathways and digital platforms, you can take control of your mental well-being without being slowed down by traditional administrative hurdles. The most important step is simply reaching out, as the “front door” to support is now wider and more accessible than ever before.
Frequently Asked Questions About Australian Mental Health System 2026
Do I need a diagnosis to use the new walk-in centers?
Answer: No, you do not need a formal diagnosis. These centers are designed to help anyone experiencing distress or mental health challenges, regardless of whether they have a named condition.
Can I get more than 10 Medicare sessions if I need them?
Answer: In 2026, the standard limit is 10 sessions per year. If you require more, you may need to utilize private health insurance, search for community-funded programs, or wait for the next calendar year.
Is the 1800 595 212 phone service free from a mobile?
Answer: Yes, this is a free-call number within Australia. It is staffed by trained professionals who can help you navigate the system and find local care providers.
What is the difference between a psychologist and a peer worker?
Answer: A psychologist has university training in mental health and can provide clinical therapy. A peer worker has personal experience with mental illness and provides support based on that lived understanding.
Does Medicare cover the cost of mental health apps?
Answer: Medicare does not “pay” for private apps, but it does provide free access to its own government-developed digital services like the Medicare Mental Health Check-In platform.