As we move through 2026, the New Zealand healthcare system is undergoing a massive shift under the latest Government Policy Statement on Health. While a new national access target is set to launch in July 2026—aiming for 80% of patients to be seen within a week—the current reality for many Kiwis remains one of “closed books” and month-long wait times. Navigating this landscape requires a strategic approach that moves beyond the traditional phone call to your local medical center.
How We Selected Our 7 Pro Tips for Access a GP New Zealand 2026
To identify the most effective ways to secure medical care today, we analyzed the 2026 Health NZ (Te Whatu Ora) guidelines and the latest digital health service expansions. Our selection criteria focused on methods that provide immediate clinical outcomes while reducing the administrative burden on the overstretched primary care workforce.
-
Speed to Consultation: We prioritized tips that offer same-day or same-week access to a clinician.
-
Regulatory Accreditation: All suggested services are New Zealand-registered and Health NZ accredited.
-
Cost-Effectiveness: We evaluated the balance between casual patient fees and long-term enrollment benefits.
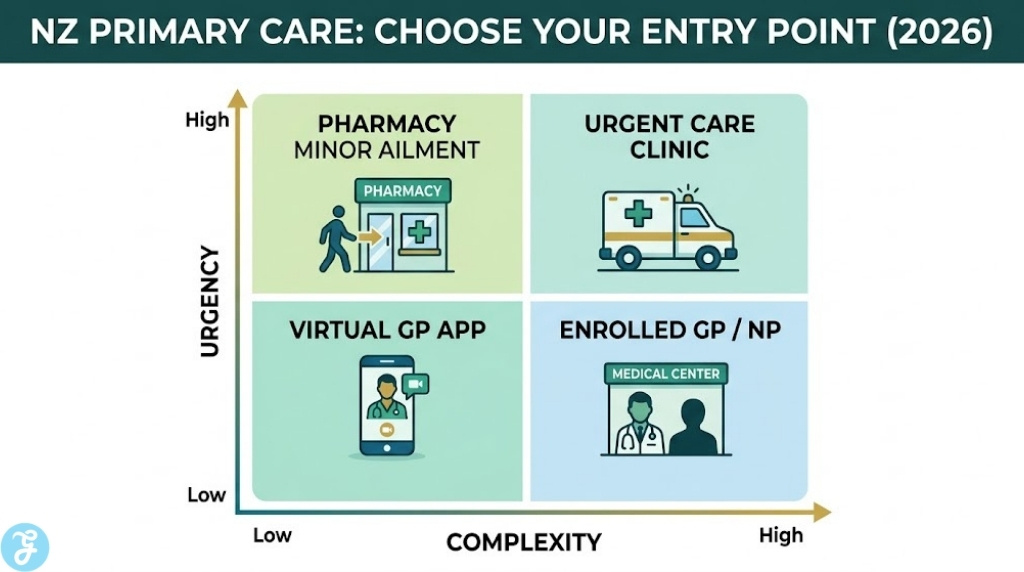
The following table provides a high-level comparison of the different “entry points” into the New Zealand primary care system in 2026.
| Access Method | Typical Wait Time | Best For | Average Casual Fee |
| Enrolled GP | 1 – 4 Weeks | Chronic Care / Referrals | $20 – $60 |
| Virtual GP App | Same Day | Scripts / Minor Ailments | $69 – $95 |
| Urgent Care Clinic | 2 – 6 Hours | Acute Injury / Sudden Illness | $90 – $150 |
| Nurse Practitioner | 1 – 3 Days | Diagnoses / Prescriptions | $30 – $70 |
7 Pro Tips for Access a GP New Zealand 2026
Securing a medical appointment in the current environment is less about waiting for an opening and more about knowing which alternative “front doors” are currently open. These seven strategies are designed to help you bypass traditional bottlenecks safely and legally.
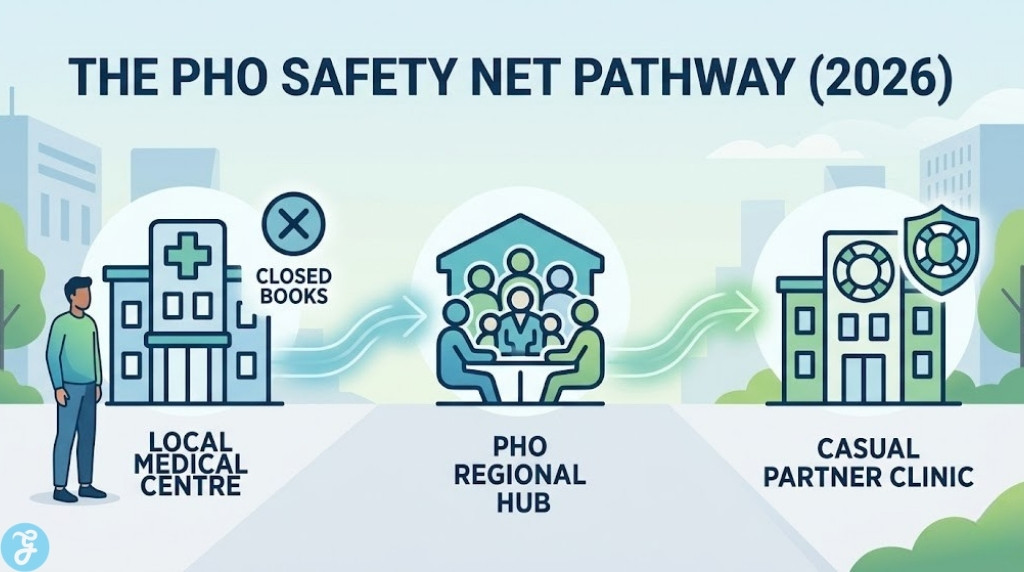
1. Utilize the PHO “Direct Intervention” Route
If you have tried multiple local clinics and found their “books are closed,” do not simply stop searching. Every medical center belongs to a Primary Health Organisation (PHO). In 2026, PHOs are mandated to assist patients who cannot find a doctor. By contacting your regional PHO directly, you can be placed on a centralized waitlist, and they can often facilitate “casual” care at a partner clinic in the interim.
Best for: Families moving to a new region where every local practice is at capacity.
Why We Chose It: It moves the administrative burden of finding a doctor from the patient to the health authority.
Things to consider: You may be assigned a doctor slightly further away than your preferred local suburb.
2. Pivot to Accredited Virtual “Casual” Services
For issues that do not require a physical exam—such as repeat prescriptions, medical certificates, or skin rashes—virtual GP services are the fastest “backdoor” in 2026. Accredited providers like Pocket Lab, Tend, and CareHQ offer same-day video consultations. Because they operate on a national scale, they can load-balance appointments across doctors in different time zones, effectively bypassing your local town’s waitlist.
Best for: Working professionals needing a quick script or a certificate for work.
Why We Chose It: It is the most reliable way to speak to a NZ-registered doctor within hours rather than weeks.
Things to consider: These services charge a “casual” fee if you are not enrolled, which is typically higher than a standard GP visit.
3. Optimize Healthpoint Filters for “Open Books”
Healthpoint remains the source of truth for New Zealand healthcare availability, but most users do not use the advanced filters correctly. When searching, specifically filter for “Enrolling New Patients” and “Virtual Care Clinics.” In 2026, many practices only open their books for 48-hour windows; checking Healthpoint at 9:00 AM on a Monday is the “pro move” to catch these newly opened spots before they fill.
Best for: Individuals who are determined to find a permanent, enrolled GP near their home.
Why We Chose It: It provides real-time data on which practices have received extra funding to expand their patient lists.
Things to consider: Information can change daily, so a follow-up phone call to confirm the Healthpoint status is essential.
4. Prioritize Nurse Practitioner (NP) Led Clinics
A significant trend in 2026 is the rise of independent Nurse Practitioner clinics. In New Zealand, NPs have the full authority to diagnose, order lab tests, and prescribe medications just like a GP. Because the public is often still looking specifically for “doctors,” NP waitlists are frequently much shorter, and the consultations are often longer and more holistic.
Best for: Managing long-term conditions like asthma, diabetes, or mental health support.
Why We Chose It: NPs provide high-level clinical care with significantly better availability than traditional GPs.
Things to consider: Ensure the clinic is “NP-led” specifically, as some standard practices still use nurses primarily for triage.
5. Leverage the Pharmacy Minor Ailment Service
Under the 2025/2026 pharmacy agreements, many community pharmacists are now funded to provide consultations and medications for minor ailments that previously required a GP visit. If you have a minor eye infection, skin condition, or uncomplicated urinary tract infection (UTI), your local pharmacist can often treat you on the spot without an appointment.
Best for: Immediate treatment of low-complexity health issues.
Why We Chose It: It completely removes the need for a GP appointment, freeing up the queue for more serious cases.
Things to consider: If the condition is complex, the pharmacist will still refer you back to a GP or Urgent Care.
6. Use the Healthline Triage Advantage
Calling Healthline (0800 611 116) is not just for advice; it is a clinical triage tool. If Healthline’s registered nurses determine your case is “urgent but non-life-threatening,” they can send a direct referral to an after-hours or urgent care clinic. This referral sometimes allows you to bypass the general waiting room or at least flags your case as “clinically pre-screened,” which can speed up your processing.
Best for: Weekend or late-night health scares where you are unsure if you need a hospital.
Why We Chose It: It provides a professional clinical “sorting” that helps you reach the right level of care faster.
Things to consider: Expect long hold times during peak flu season or public holidays.
7. Enroll in “Hybrid-First” Large Practices
Large multi-site practices, such as “The Doctors” or “Tend,” utilize a shared pool of clinicians across multiple physical locations. In 2026, these groups often allow enrolled patients to book a “virtual-first” appointment with any doctor in their network if their local GP is busy. This “internal roaming” feature ensures you stay within the subsidized funding loop while accessing a much larger pool of available timeslots.
Best for: People who value the subsidised cost of enrollment but need the flexibility of a large network.
Why We Chose It: It combines the cost benefits of a local GP with the technological efficiency of a tech startup.
Things to consider: You may not see the same doctor every time, which can impact “continuity of care.”
Our Top 3 Picks and Why?
-
Virtual “Casual” Services (Pocket Lab/Tend): This is our top pick for 2026 because it solves the “immediate need” problem. When you are sick today, a GP appointment in three weeks is useless. These platforms solve the problem in real-time.
-
Nurse Practitioner Clinics: We chose this because it is the most underutilized resource in the Kiwi system. Tapping into NP expertise is the smartest way to get high-quality care without the “doctor” wait times.
-
The PHO Intervention Route: This is essential for long-term health. While virtual tools are great for one-offs, everyone needs a “medical home.” Forcing the PHO to help you find one is the only way to ensure you don’t fall through the cracks of the system.
How to Choose the Right GP Access Strategy for You?
Choosing a strategy depends on whether your need is urgent, administrative, or for a long-term health partnership. Use the following framework to decide your next move.
The Selection Framework
-
Determine the Urgency: If it is a life-threatening emergency, skip the GP and call 111. If it is an acute injury (like a broken bone), go straight to Urgent Care.
-
Assess the Complexity: Can this be solved with a conversation and a script? Choose a virtual GP. Does it need a physical exam or a sensitive procedure? Choose a physical clinic.
-
Evaluate Your Budget: Are you willing to pay a $70+ casual fee for speed, or do you need the $20 subsidized enrolled rate?
-
Check Your Enrollment Status: If you are already enrolled but can’t get in, check if your practice offers “Practice Plus” or an internal virtual overflow.
The following matrix helps you match your symptoms to the most efficient 2026 access point.
| Symptom / Need | Best Access Point | Reason |
| Simple Script Renewal | Virtual GP App | Done in 10 mins via phone. |
| Minor Eye/Skin Infection | Community Pharmacy | No appointment needed; walk-in. |
| New Chronic Concern | Enrolled GP / NP | Needs long-term management & records. |
| Sudden Fever / Pain | Urgent Care / Healthline | Needs immediate clinical assessment. |
The Final Checklist
-
Have you checked Healthpoint this morning for “open books” in your area?
-
Is your current issue something a Pharmacist or Nurse Practitioner could handle?
-
If you can’t find a doctor, have you emailed your local PHO for assistance?
-
Do you have a virtual GP app (like Tend or CareHQ) downloaded and set up for emergencies?
-
Have you checked if your Community Services Card is up to date to reduce casual fees?
Navigating the Future of Kiwi Primary Care
The “traditional” GP model in New Zealand is evolving into a multi-channel system where digital tools and specialized nurses play a much larger role. While waitlists are currently a challenge, the system is more accessible than it appears if you are willing to use the “backdoors” provided by technology and expanded clinical roles. By 2027, the goal is for these “pro tips” to become standard practice, ensuring every Kiwi can access a healthcare professional within days, not weeks.
Frequently Asked Questions About Access a GP New Zealand 2026
Why are GP waitlists so long in 2026?
Answer: A combination of an aging population, a workforce shortage, and a shift toward more complex chronic disease management has placed unprecedented pressure on traditional local clinics.
Is a Virtual GP as good as a physical GP?
Answer: For about 70% of primary care needs (scripts, advice, simple diagnoses), virtual care is identical in quality. However, for anything requiring physical palpation, heart monitoring, or physical tests, a face-to-face visit is still required.
Can I be enrolled at two different GP practices?
Answer: No. You can only be enrolled (and therefore subsidized) at one practice at a time. However, you can see any other doctor in the country as a “casual” patient if you pay the full fee.
What is the difference between a GP and a Nurse Practitioner?
Answer: In terms of what they can do for you in a clinic, very little. Both can diagnose, treat, and prescribe. The difference lies in their training background—GPs come from a medical doctor track, while NPs come from an advanced nursing clinical track.
Does Healthline cost money to call?
Answer: No, Healthline (0800 611 116) is a free, 24/7 service funded by the government for everyone in New Zealand.