Before you get a bad rap like the villain in some cheesy cholesterol commercial, let’s peel back the layers and expose the important things to know about cholesterol. Buckle up, grab a carrot stick (we’ll get to that!), and get ready to bust myths, banish confusion, and empower your heart health with insider knowledge.
Forget the scary charts and jargon-filled pamphlets. We’re doing this plainly, playfully, and packed with real-life examples. Think of it as a spy mission into the cholesterol underworld, where we’ll uncover its secret identities (“good” HDL vs. “bad” LDL), its sneaky effects (think clogged arteries like traffic jams), and the superpowers you wield to keep it in check (think diet, exercise, and maybe even a sprinkle of laughter).
Ready to swap confusion for confidence? Let’s crack the cholesterol code, one juicy truth at a time.
Content Highlights
- Cholesterol classifications include “bad” LDL, “good” HDL, and disease-indicating triglyceride varieties.
- Optimal reference levels for total volumes and type ratios differ between ages and health statuses.
- Both dietary intake and liver synthesis contribute to blood concentrations.
- Nutrition quality and routine activity strongly support heart-protective lipid balancing.
- Looking beyond total scores to focus more on particle type functionality and oxidation reduction better promotes wellness.
- Work with knowledgeable practitioners, closely monitoring person-specific treatment responses over time.
Important Things to Know About Cholesterol
These fundamentals underpin all subsequent details of this multifaceted blood lipid:
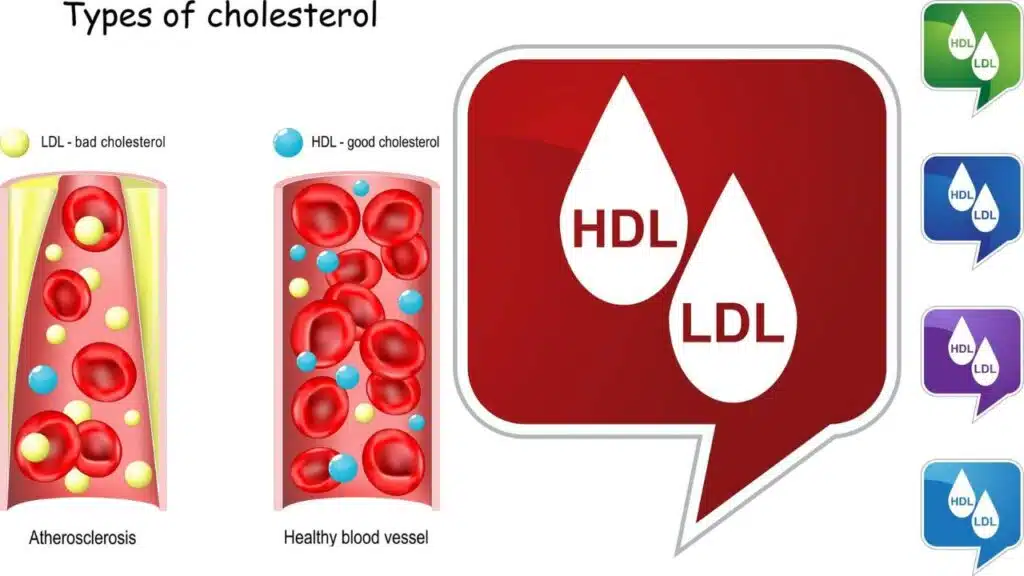
1. Cholesterol Classifications
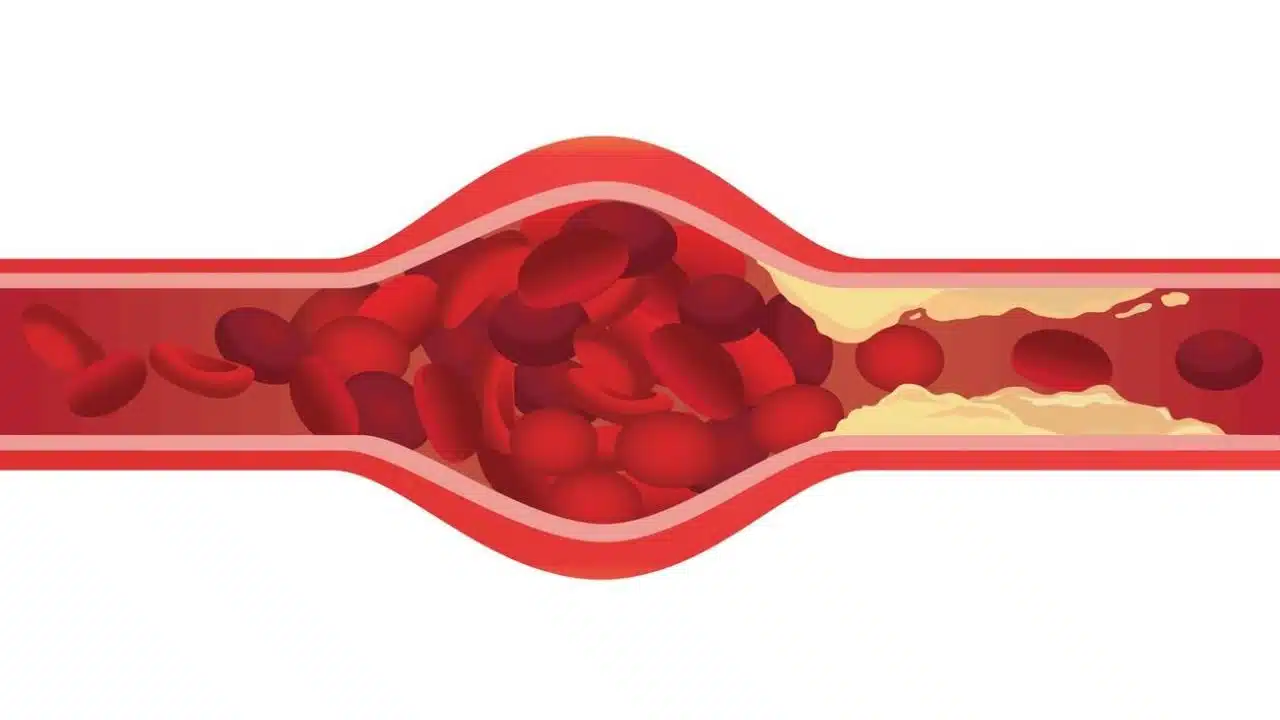
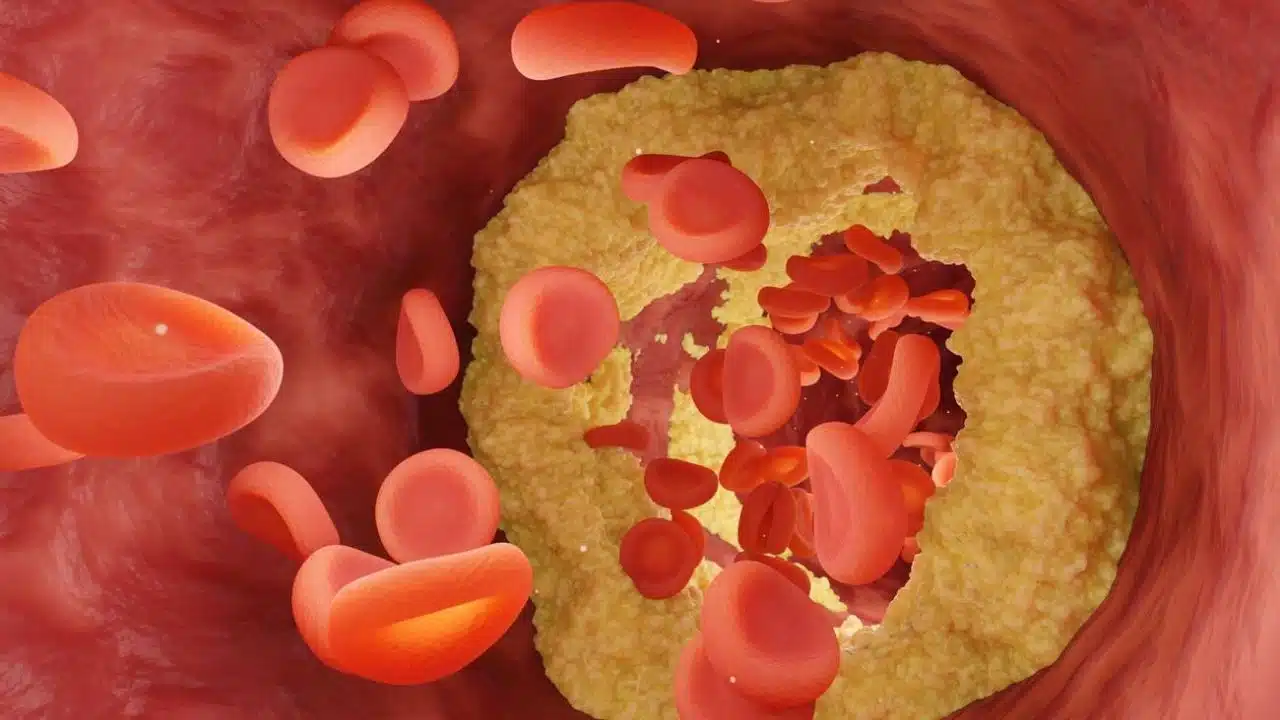
LDL “Bad” Cholesterol transports lipids throughout for cellular needs, but excess accumulation along arterial walls causes atherosclerotic “plaque,” gradually narrowing essential blood flow. HDL “Good” Cholesterol: Circles capturing excess lipids for disposal and protecting arterial health. Higher levels may balance other elevated risks. Triglycerides are directly linked to heart health via interactions impacting HDL and LDL ratios, as well as diabetes and obesity risk factors. Lifestyle hugely influences levels.
2. Main Functions
Despite potential cardiovascular risks at unchecked levels, cholesterol serves critical biological purposes:
- Facilitates vitamin D synthesis
- Bolsters cell wall flexibility and permeability
- It insulates nerve cell axons, speeding signal transmission.
- Participates in producing key hormones and compounds
- Enables fat digestion and absorption
3. Sources
Diet has a big effect on cholesterol levels in the blood, but liver biosynthesis makes about 80% of it so that it can work well and have enough volume. Hence, both intake and individual processing variability affect profiles.
Healthy Cholesterol Levels
Identifying elevated types and ratios against “normal” reference ranges provides generalized risk estimations. But individual health histories determine their significance.
1. Total Cholesterol Goals
- Low Risk: Below 200 mg/dL
- Borderline Risk: 200–239 mg/dL
- High Risk: Over 240 mg/dL
2. LDL “bad” cholesterol goals
- Low Risk: Under 100 mg/dL
- Borderline Risk: 130–159 mg/dL
- High Risk: Over 190 mg/dL
3. HDL “Good” Cholesterol Goals
- Low Risk Under 40 mg/dL (men), 50 mg/dL (women)
- High Risk: Over 60 mg/dL
4. Triglyceride Goals
- Low Risk: Under 150 mg/dL
- High Risk: Over 200 mg/dL
5. Key Ratios
Total/HDL Ratio: This quantifies the overall balance between good and bad. Below 5 proves ideal. Triglycerides/HDL Ratio: Assesses related metabolic heart disease risks. Under 2 stays safest.
How Does Diet Affect Cholesterol?
While cholesterol intake alone doesn’t determine blood levels as once assumed, quality nutrition remains vital in preventing atherosclerosis.
1. Limit animal-saturated fats
Red meats, full-fat dairy and fried foods contain saturated fats and dietary cholesterol, increasing bad LDL quantities. Leaner proteins and plant fats improve profiles.
2. Increase unsaturated fats
Monounsaturated and omega-3 polyunsaturated fats from olive oil, avocados, nuts and oily fish raise good HDL concentrations, mitigating LDL effects.
3. Reduce refined carbohydrates
Sugary foods and highly processed grains adversely influence triglycerides and other diabetes risk factors, also exacerbating cholesterol troubles.
4. Eat more fiber
Soluble fibers from oats, beans, apples and carrots bind cholesterol excreting rather than absorbing excess from food intake for cleaner arterial balance.
5. Lose excess weight
Obesity stresses and oxidizes cholesterol while shrinking HDL and elevating triglycerides and LDL concentrations. Shedding pounds proves vital.
So wholesome, balanced nutrition beneficially regulates cholesterol health beyond just numerical intake levels.
How Does Exercise Impacts Cholesterol?
Vigorous, regular aerobic activity substantially affects lipid profiles through positive cardiovascular conditioning and body composition improvements.
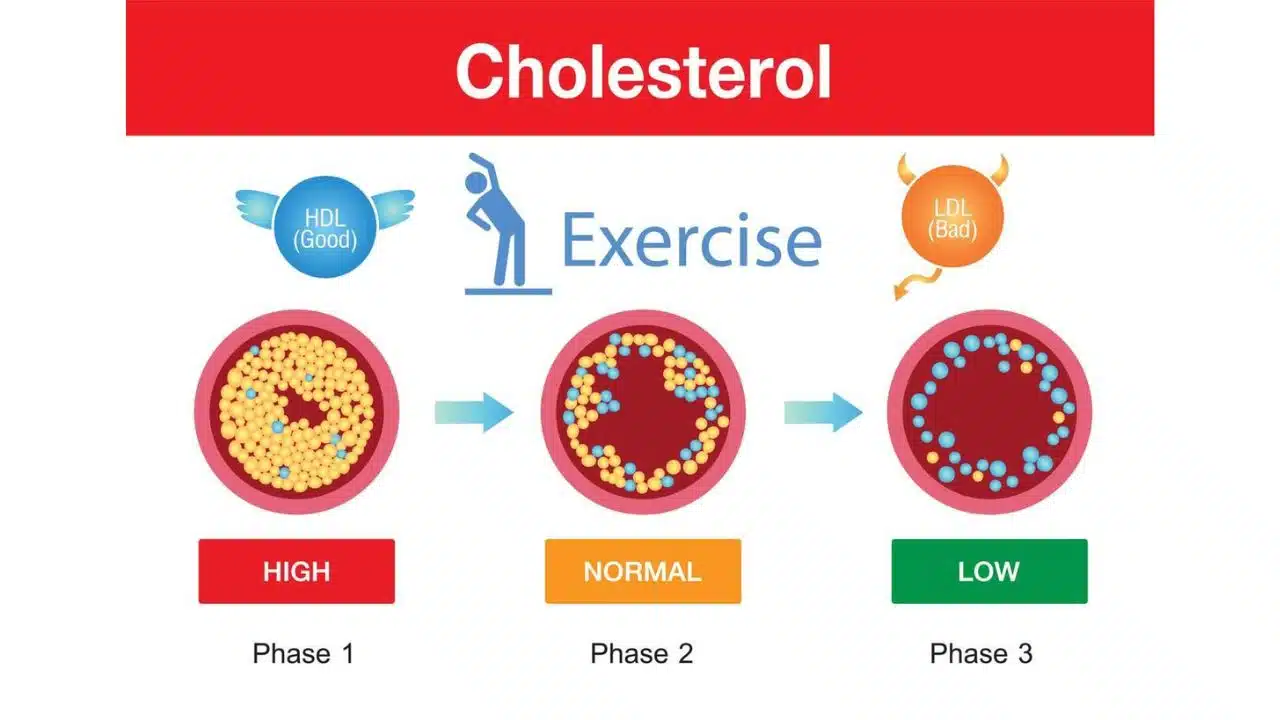
1. Aerobic exercise boosts HDL
Interval running, swimming and similar vigorous cardio workouts increase HDL by up to 10%, vastly improving the ratio between good and bad cholesterol.
2. Exercise lowers triglycerides
Active individuals often maintain triglyceride scores 20–30 percentage points below those of more sedentary people, keeping this predictive risk marker in check.
3. Movement Assists Weight Loss
Since adipose fat cells interact adversely with blood lipids, burning excess weight through calorie-burning workouts reduces all detrimental cholesterol markers.
So alongside nutrition, consistent physical activity keeps cholesterol ratios leaning favorably, even despite genetic predispositions.
Key Perspectives on High Cholesterol
Cholesterol levels exceeding guidelines or desired ratios between types certainly warrant medical interventions through prescription medications, nutrition planning and lifestyle alterations. But contextualizing test results prevents counterproductive anxiety.
1. Range Above “Normal” Differs Between Ages
Standard reference ranges reflect middle-aged adults. Younger individuals normally register slightly higher, while elderly people tend to trend lower naturally. So compare appropriately.
2. Understand Transient Variances
Temporary illnesses, injuries and emotional stresses alter results. Unless consistent diagnoses reveal chronic imbalances, consider natural variances between screenings before overreacting.
3. Remember, ratios matter more
While total scores simplify reporting, the ratio comparisons between protective HDL, transportive LDL and metabolism-influencing triglycerides better indicate cardiovascular risk potential and treatment progress.
4. Consider inflammation problems
Often, underlying chronic inflammatory conditions like autoimmunities and insulin resistance drive consistent lipid imbalance and oxidation rather than transient dietary influence alone. Identifying and addressing root causes empowers lasting management.
5. Recognize the Limitations of Lipid Panels
Statistics show that cholesterol is somewhat linked to overall heart health risks. However, each person’s biomarker responses are very different, and only more in-depth tests like lipoprotein particle counts can tell the difference. Context matters.
So avoid knee-jerk anxiety over borderline cholesterol scores. Ensure holistic understanding through thoughtful physician consultations, personalizing care for your situation. Trends prove more informative than single data points.
Emerging Research on HDL and LDL Functionality
Ongoing scientific insights continue to evolve perspectives surrounding cholesterol’s role in transporting and storing fatty lipids. Core assumptions now undergo closer scrutiny, suggesting far greater intricacies involved.
1. All LDL Particles Are Not Equally “Bad”
Measuring total LDL volume misses nuance. Particle size and composition determine the driving factors behind plaque accumulation. Larger, fluffier LDL molecules transport differently than small, dense ones, predicting problems better.
2. HDL Particles Vary in Protective Capacities
Similar to LDL range variabilities, good HDL contains subsets with less anti-inflammatory action. Dysfunctional versions accelerating atherosclerosis exist despite contributing to scored quantities on lipid panels.
3. Oxidative stress alters function.
Excess free radicals oxidize cholesterol, making both HDL and LDL particles dysfunctional and directly accelerating foam cell plaque formation. Reducing inflammation and oxidation minimizes associated cardiovascular risks as much or more than managing score levels alone.
4. Genetics Influence Lipid Behaviors
ApoE status and other hereditary factors change how cholesterol is transported throughout the body, affecting risks. Beyond scored volumes, particle contents prove vital in comprehending person-specific disease predispositions.
Research momentum Questioning prior dogmas opens doors towards vastly more nuanced, individualized future management. Raising “good” HDL may prove less protective without simultaneous efforts to address underlying inflammation or lipid oxidation sources. Holistic care accounts for wider biological synergy.
Conclusion: Apply Smarter Cholesterol Smarts
Rather than reactively avoiding all dietary cholesterol out of confusion and anxiety upon receiving high test results, instead implement positive lifestyle changes: emphasize anti-inflammatory nutrition, increase activity levels, manage body composition and consult capable practitioners, accurately interpreting what personalized scores mean and monitoring realistic health threats for your situation.
There exist no predefined optimally “normal” cholesterol levels universally. But aggregating incremental knowledge allows deft navigation, promoting properly balanced lipid transport mechanisms vital to sustaining health through holistic, multifaceted strategies. Now put smarter cholesterol smarts into action!
FAQs (Frequently Asked Questions) About Cholesterol
If you want to know more important things to know about cholesterol, check out the answers below.
How often should blood lipid panels occur?
Unless diagnosed imbalances are resolved, annual cholesterol screening suffices for low-risk younger adults. Frequency increases with age or concerning test results, often needing 3-6 month testing intervals during active treatment.
Do eggs raise my cholesterol dangerously?
Dietary cholesterol affects but does not directly determine blood levels. Unless medically eliminating whole nutrition groups like eggs improves risk ratios substantially through testing, most healthy individuals tolerate whole eggs in moderation when following wise lifestyle habits overall.
Is medication taken if levels remain high?
After trying different lifestyle changes and therapeutic doses but still not being able to fix imbalances in high-risk individuals, statin drugs and other drugs carefully prescribed by a doctor can help lower LDL and triglycerides or raise HDL, which is good for long-term heart health.
What blood markers assess cardiovascular risks?
Aside from scored lipid panels, predictive tests like fasting glucose assessments for insulin resistance, high-sensitivity CRP assessments for inflammation, and advanced lipoprotein particle profiles make it more accurate to diagnose heart health risks in patients. This is true even though total cholesterol numbers can be very different from one person to the next.